Spine Disorders — MCQs

On this page
A 25-year-old male presents with a three-month history of lower back pain, following a fall. He reports mild weakness in both lower limbs but can walk without support. He has approximately 30% sensory loss and exhibits bladder symptoms. Physical examination reveals tenderness over D12-L1 vertebrae. X-ray shows paradiscal destruction of vertebrae, and MRI reveals destruction with indentation of the thecal sac. What is the most appropriate management?
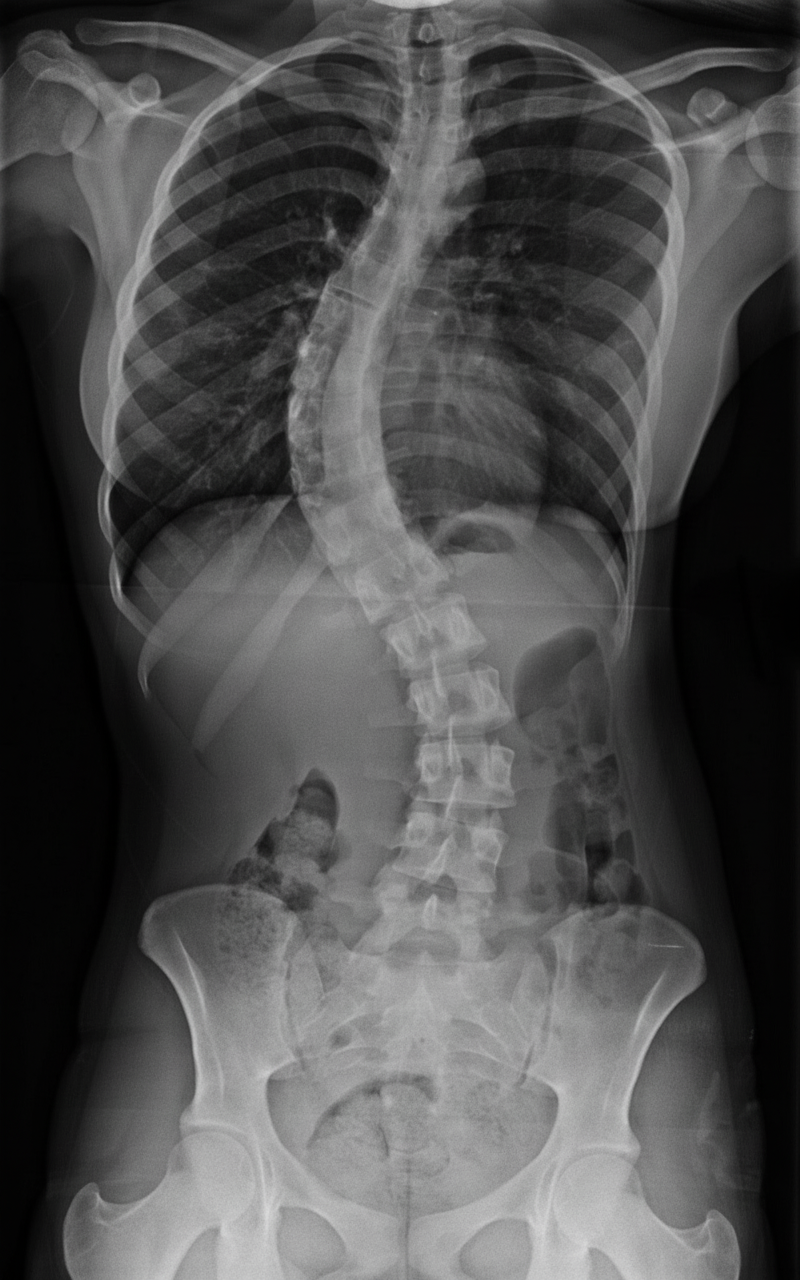
Which of the following spine deformities is being evaluated?
Which of the following statements about spinal injuries is false?
Spondylolysis is more common in which anatomical location?
In a case of tuberculosis of the thoracic spine, what is the earliest sign of cord compression?
The Denis classification is used to assess which of the following?
In which of the following conditions does pseudoclaudication occur?
What is the most common cause of acute sciatica?
Adam's test is performed for which of the following?
A patient with traumatic paraplegia due to injury of the T3 thoracic cord level presents with a blood pressure of 210/120. What should be the initial management?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
