Spine Disorders — MCQs

On this page
Which of the following is the MOST common skeletal manifestation in Type-1 Neurofibromatosis?
Scheuermann's disease occurs in which age group?
Which of the following is seen more commonly in rheumatoid arthritis than in ankylosing spondylitis?
What is the most common cause of secondary tumors affecting the spinal cord?
What is the next commonest site of intervertebral disc prolapse after L4-S1?
A 46-year-old male, a known alcoholic, presents with pain in the dorsal spine. Examination reveals tenderness at the dorso-lumbar junction. Radiographs show destruction of the 12th dorsal vertebra with loss of disc space between D12 and L1 vertebrae. What is the most probable diagnosis?
Which joint is NOT involved in Rheumatoid arthritis according to the 1987 ACR Classification Criteria?
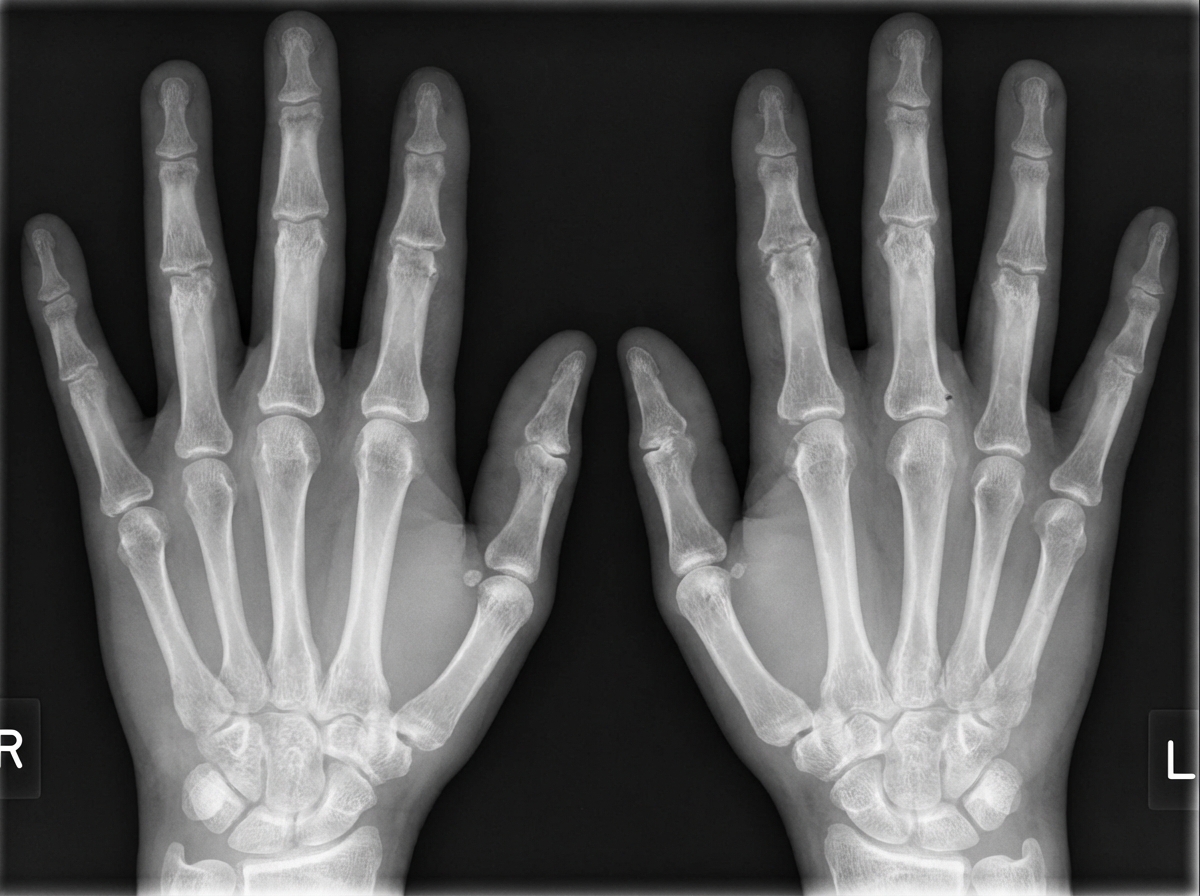
A 40-year-old female presents with a history of fever, weight loss, polyarthralgia, morning stiffness, and bilateral hand pain. Based on the provided radiological findings, what is the most likely diagnosis?
Prolapsed intervertebral disc is most common at which spinal level?
Metal on metal articulation should be avoided in which of the following situations?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
