Spine Disorders — MCQs

On this page
In which spinal disease are both the bone and disc spaces involved?
A burst fracture is typically caused by which type of mechanism?
What is the first symptom in tuberculous cord compression?
A patient presents with a burning sensation in the little toe, and a weak ankle reflex. Which spinal disc herniation is most likely responsible?
A 45-year-old female presented with neck pain and stiffness for 3 months. The diagnosis is a spinal condition. Which of the following is NOT an operative treatment for this condition?
Scheuermann's disease is characterized by which of the following?
An 87-year-old woman presents with lower back pain exacerbated by walking or prolonged standing, and occasionally relieved by bending over. Physical examination reveals a thin elderly woman who walks with a cane, with her lower back moderately flexed. Motor power in her lower extremities is normal, but she has impaired sensation to light touch and vibration below the L4 dermatome bilaterally. Deep tendon reflexes are normal in her upper extremities but absent in both lower extremities. MRI of the lumbosacral spine is performed. What will be the most likely finding on this study?
A 55-year-old male presents with urinary incontinence and severe back pain for 10 days. Imaging shows a lumbar disc prolapse. He has no history of weight loss or fever. What is the diagnosis?
What substance is used for vertebroplasty?
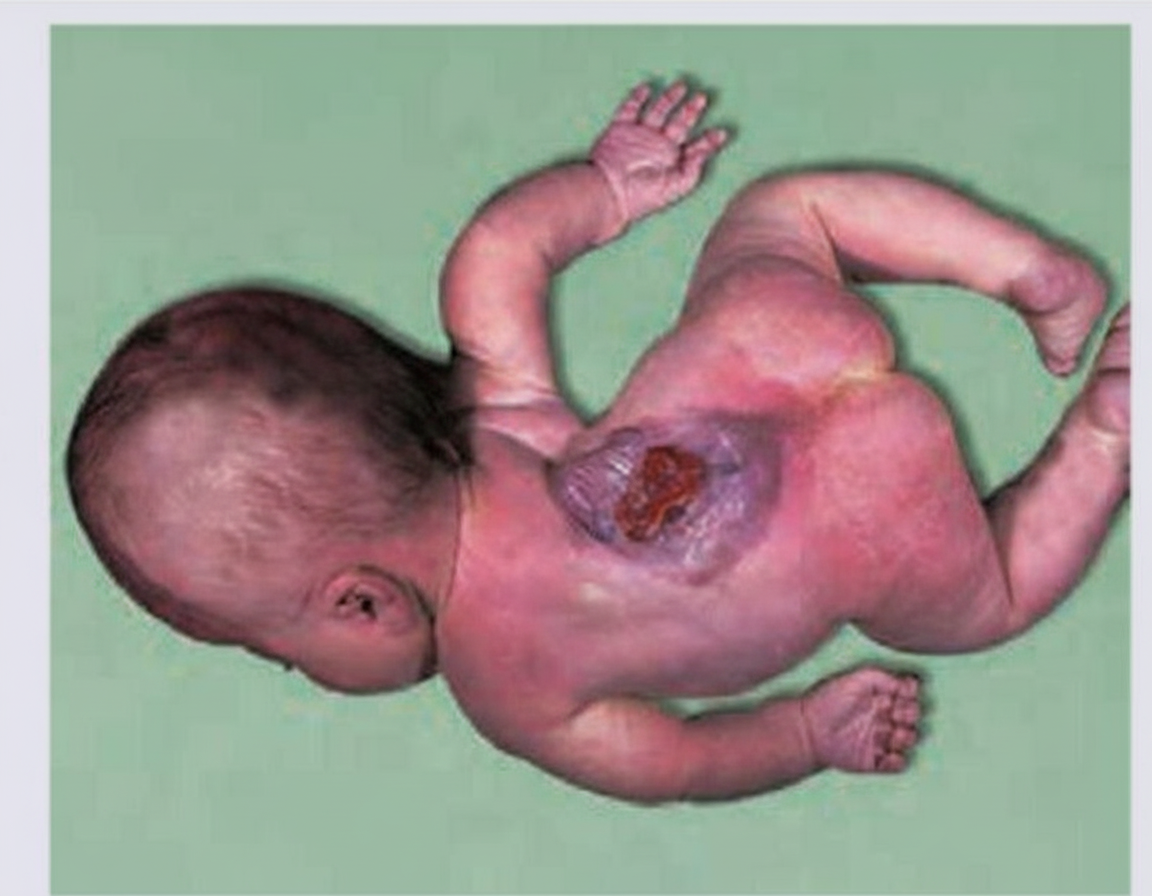
This defect most commonly involves which region of the spine?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
