Spine Disorders — MCQs

On this page
Lumbar canal stenosis typically presents as?
Disc herniation between L4 and L5 involves which nerve root?
Examine the provided knee X-ray carefully. What is the most likely diagnosis?
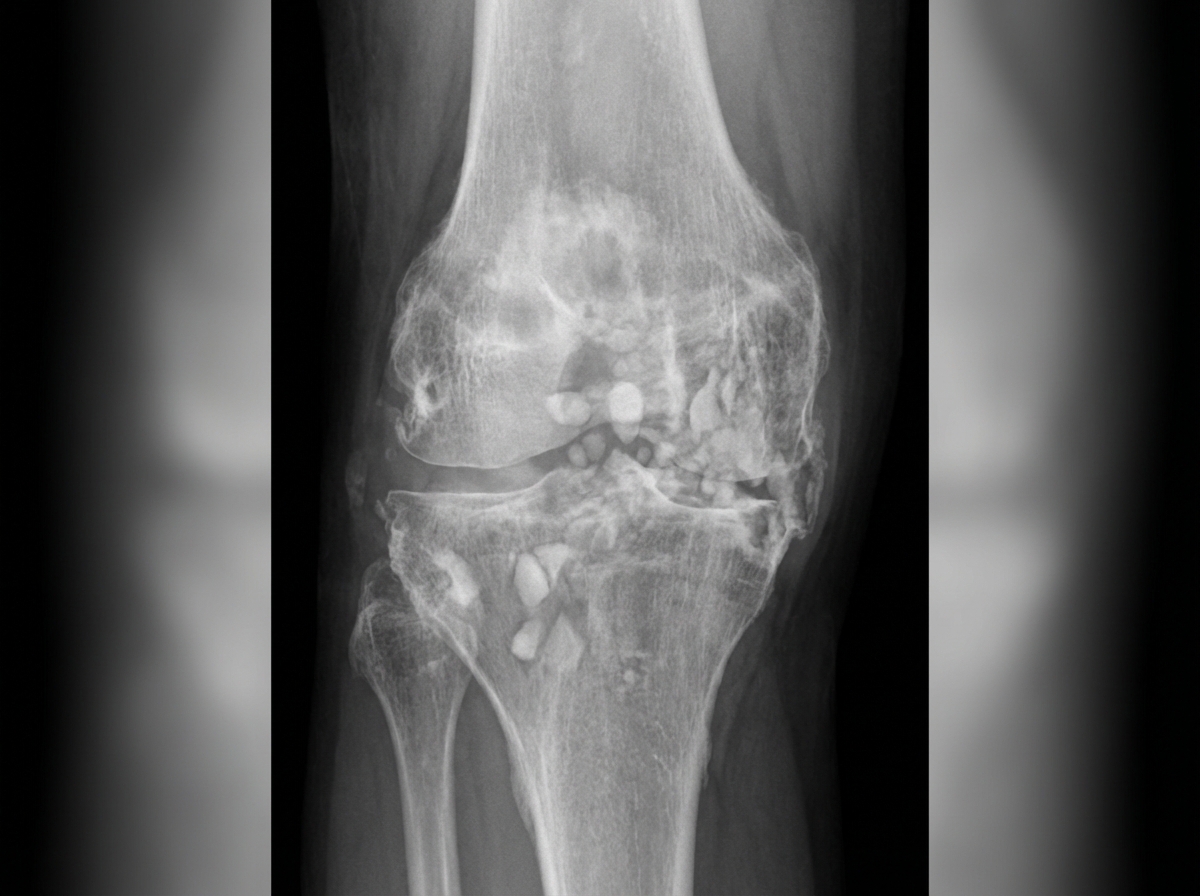
The following X-ray shows a 13-year-old child presenting with difficulty in breathing and gradually developing respiratory compromise. What is the diagnosis?
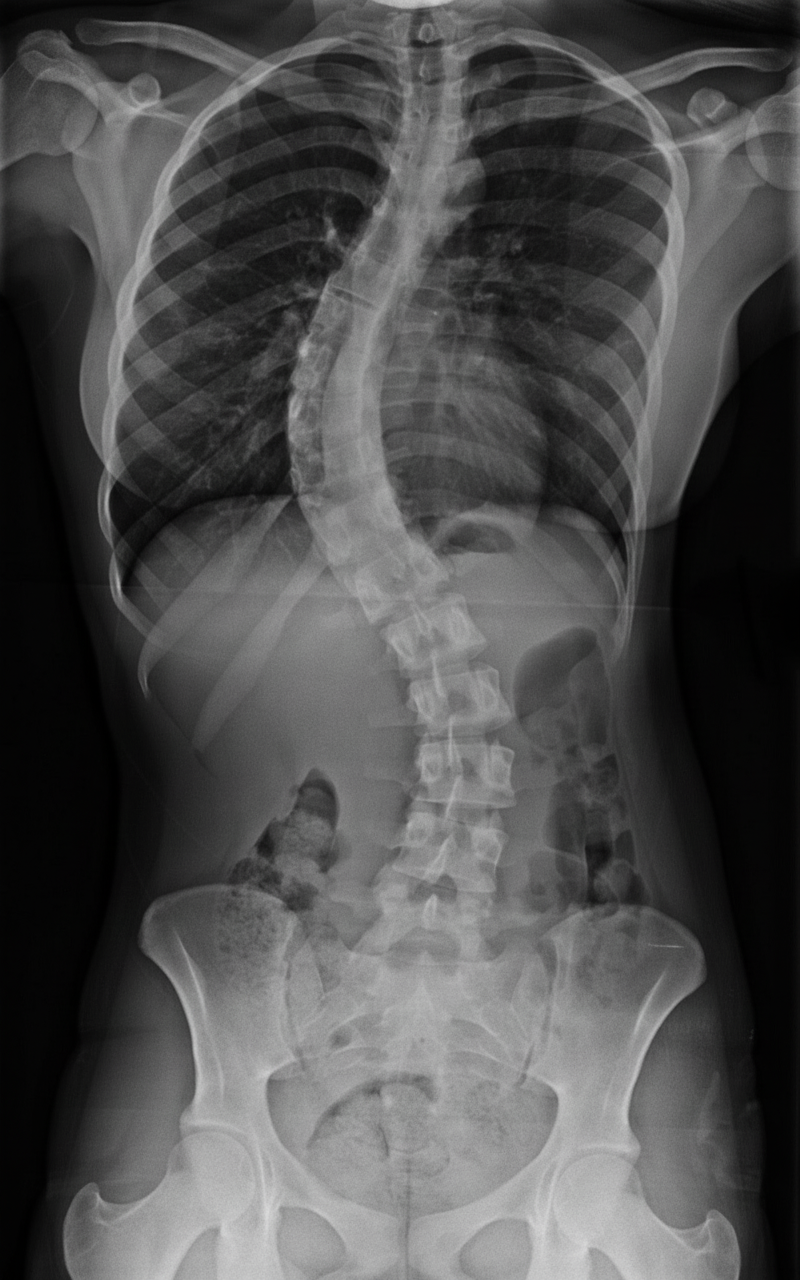
What is the most common tumor of the spine?
Needle-shaped crystals that are negatively birefringent on polarized microscopy are characteristic of which crystal-associated arthropathy?
A 40-year-old male presented with chronic back pain for 5 years. He was referred to an orthopedician after taking unspecified medications in his village. Imaging revealed an abnormality of the spine. Which of the following structures are primarily responsible for this abnormality?
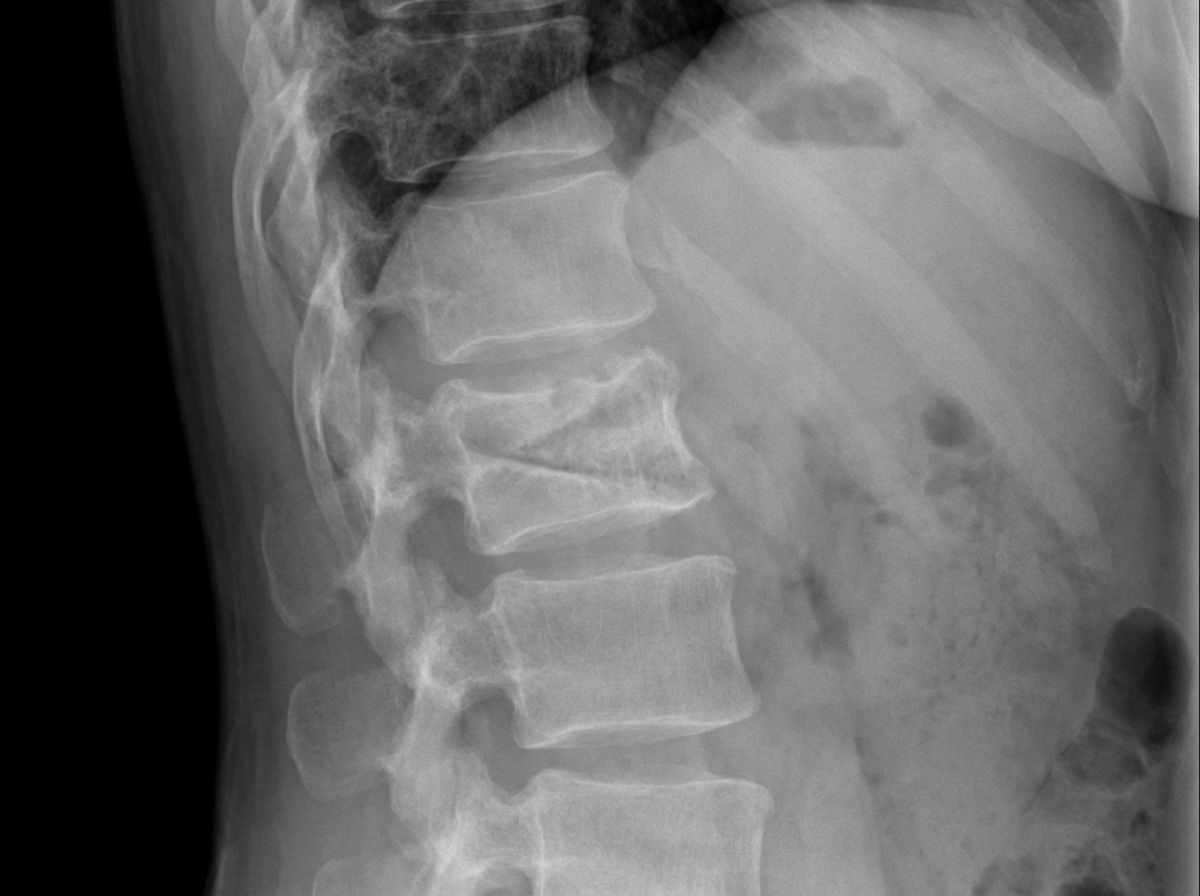
What is the most important single special investigation in lumbar disc prolapse?
A Clay Shoveler's fracture involves which part of the vertebra?
What is the commonest cause of spinal cord injuries in India?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
