Spine Disorders — MCQs

On this page
A 50-year-old male with a history of chronic low back pain presents with new-onset bowel and bladder incontinence. What is the next best step in management?
What is the characteristic postural deformity observed in advanced ankylosing spondylitis?
During an examination of the back, a palpable step-off in the lower lumbar region suggests a disruption of which structure?
A 40-year-old athlete experiences sudden back pain while lifting heavy weights. An MRI reveals a herniated lumbar disc. What is the best initial management?
Craniocervical junction abnormalities are seen in all of the following except:
What is a common symptom of lumbar canal stenosis?
Schober's sign is for :
Hangman's fracture is the fracture involving which cervical vertebra?
Test used for prolapsed lumbar intervertebral disc is?
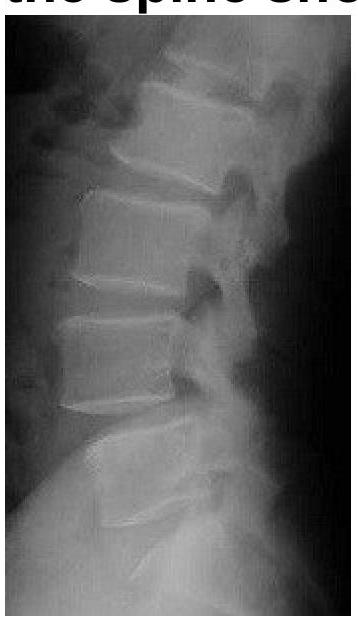
What should be the most likely diagnosis of this 65-year-old lady who presents with backache?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
