Spine Disorders — MCQs

On this page
Which of the following is NOT an X-ray finding of Rheumatoid Arthritis?
Which of the following is a poor prognostic indicator of Pott's paraplegia?
Which of the following is NOT true about spinal tuberculosis?
When do you operate for a prolapsed disc?
A 42-year-old male presents with frequent attacks of joint pain. An X-ray reveals soft tissue swelling. What is the most likely diagnosis?
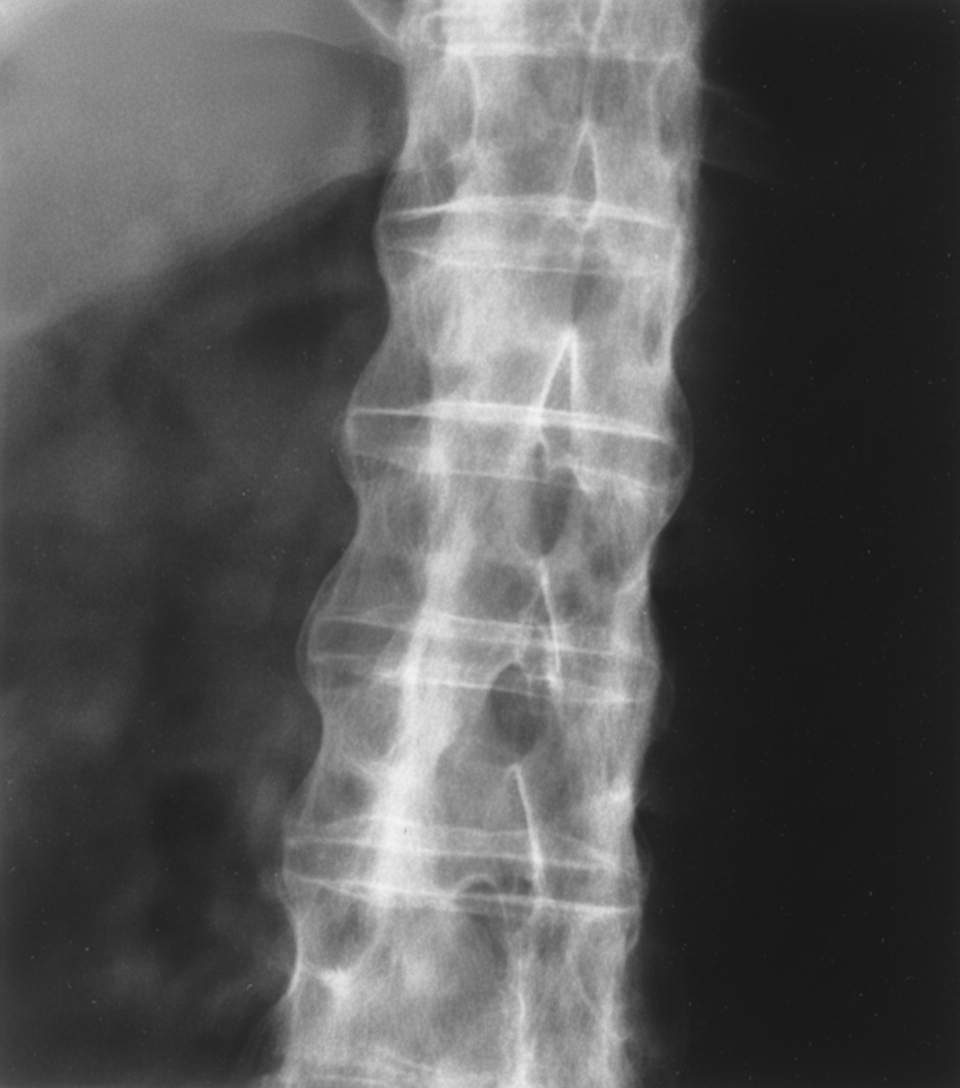
A 22-year-old man presents with low back pain and stiffness, which have progressively worsened over several months. He also reports nocturnal stiffness and hip pain. Physical examination reveals paravertebral muscle tenderness and limited lumbar spine flexion. Radiographic findings of the lumbar spine are shown. What is the most likely diagnosis?
In a patient with cervical disc prolapse, what is the recommended management?
Which of the following is not a feature of Tuberculosis of the spine?
Which of the following is FALSE regarding Charcot's joint in diabetes mellitus?
What is the investigation of choice for a lumbar prolapsed disc?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
