Spine Disorders — MCQs

On this page
What is the most common location of spinal tumors?
What condition is characterized by a "wind-swept deformity"?
All of the following are included as yellow flag signs of low back pain, except?
The Milwalkee brace is used in the treatment of which spinal condition?
Heberden's nodes are seen in which of the following conditions?
What is the first symptom of spinal tuberculosis?
The talocalcaneonavicular joint is a type of which joint?
A patient develops myelopathy post-trauma. What is the recommended initial dose of methylprednisolone?
What is the most common malignancy that metastasizes to the spine in females?
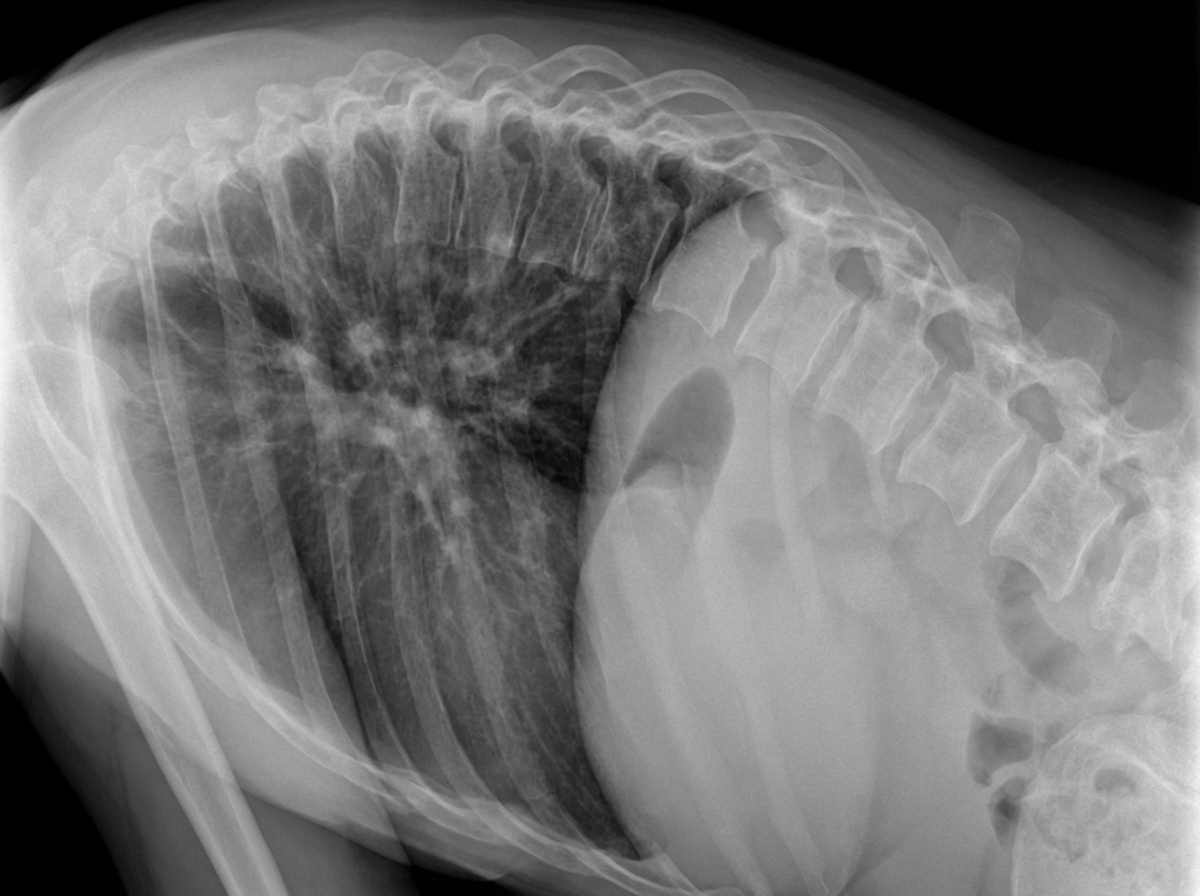
What is the commonest cause of the given condition in a young person?
Practice by Chapter
Cervical Spine Disorders
Practice Questions
Thoracic Spine Disorders
Practice Questions
Lumbar Spine Disorders
Practice Questions
Intervertebral Disc Disease
Practice Questions
Spinal Stenosis
Practice Questions
Spondylolisthesis
Practice Questions
Spinal Deformities
Practice Questions
Spinal Infections
Practice Questions
Spinal Tumors
Practice Questions
Spinal Cord Injuries
Practice Questions
Minimally Invasive Spine Surgery
Practice Questions
Rehabilitation of Spine Conditions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
