Arthrology and Infections — MCQs

On this page
A child presents with a swollen, painful knee and high fever, with no history of trauma. Acute osteomyelitis is suspected. Which part of the bone is earliest involved in hematogenous osteomyelitis?
Charcot's joint is another name for a joint affected by which condition?
Monoarticular joint involvement is seen in which of the following?
A patient has a history of similar symptoms at the same site two years ago, developing pain and swelling. X-ray shows the following features. What is the diagnosis?
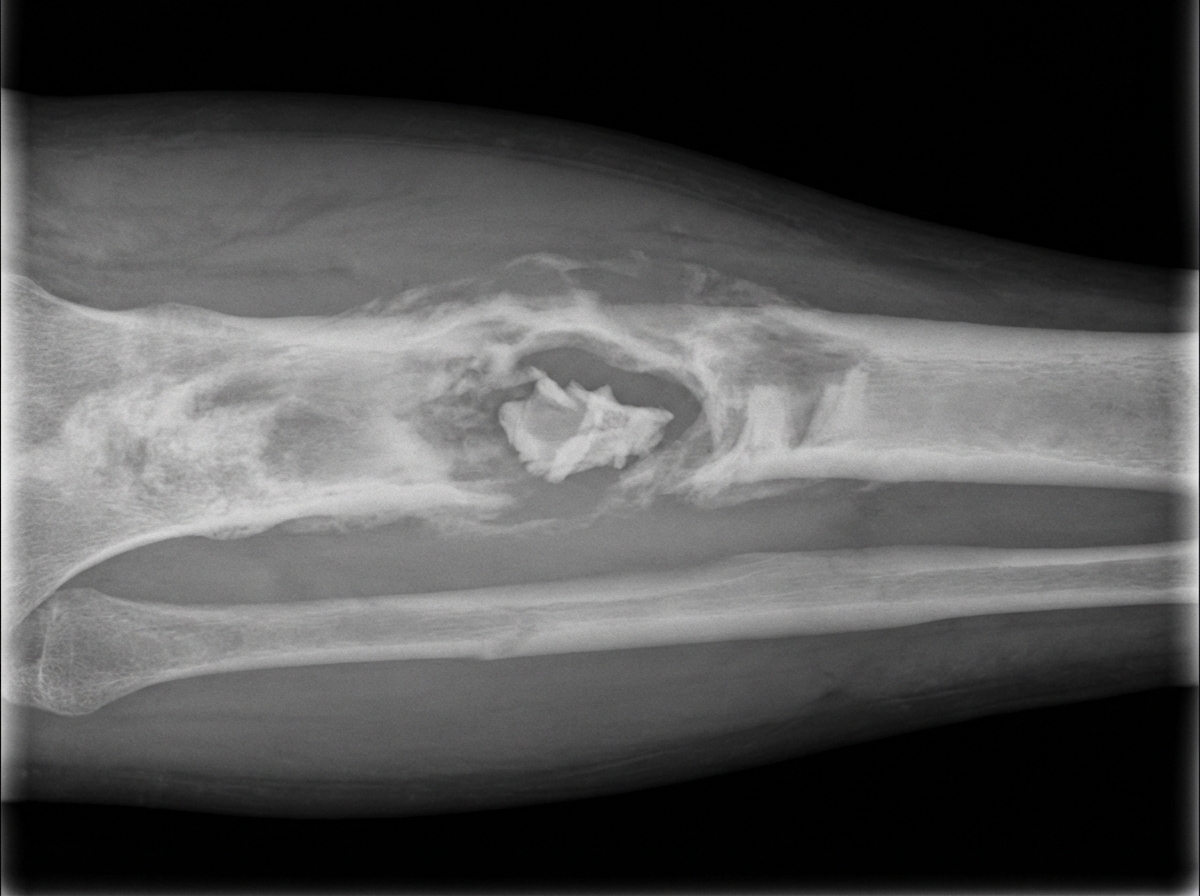
Tuberculous arthritis of a joint, in sites other than the spine, in advanced cases leads to which of the following?
Acute osteomyelitis of long bones commonly affects which part?
All of the following findings are in favor of an inflammatory joint pathology except?
What is the most common site of tuberculosis?
Brodie's abscess occurs in which type of bone?
The joint commonly involved in psoriatic arthritis is?
Practice by Chapter
Septic Arthritis
Practice Questions
Osteomyelitis
Practice Questions
Tuberculosis of Bones and Joints
Practice Questions
Fungal and Parasitic Infections
Practice Questions
Diabetic Foot Infections
Practice Questions
Prosthetic Joint Infections
Practice Questions
Reactive Arthritis
Practice Questions
Management of Joint Infections
Practice Questions
Prevention of Orthopaedic Infections
Practice Questions
Biofilms in Orthopaedic Infections
Practice Questions
Antibiotic Prophylaxis
Practice Questions
Implant-Related Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
