Arthrology and Infections — MCQs

On this page
All of the following are associated with chronic osteomyelitis except?
What pathological process causes both destruction of bone and reduction of joint space?
Aspirated synovial fluid in septic arthritis will typically show which of the following characteristics?
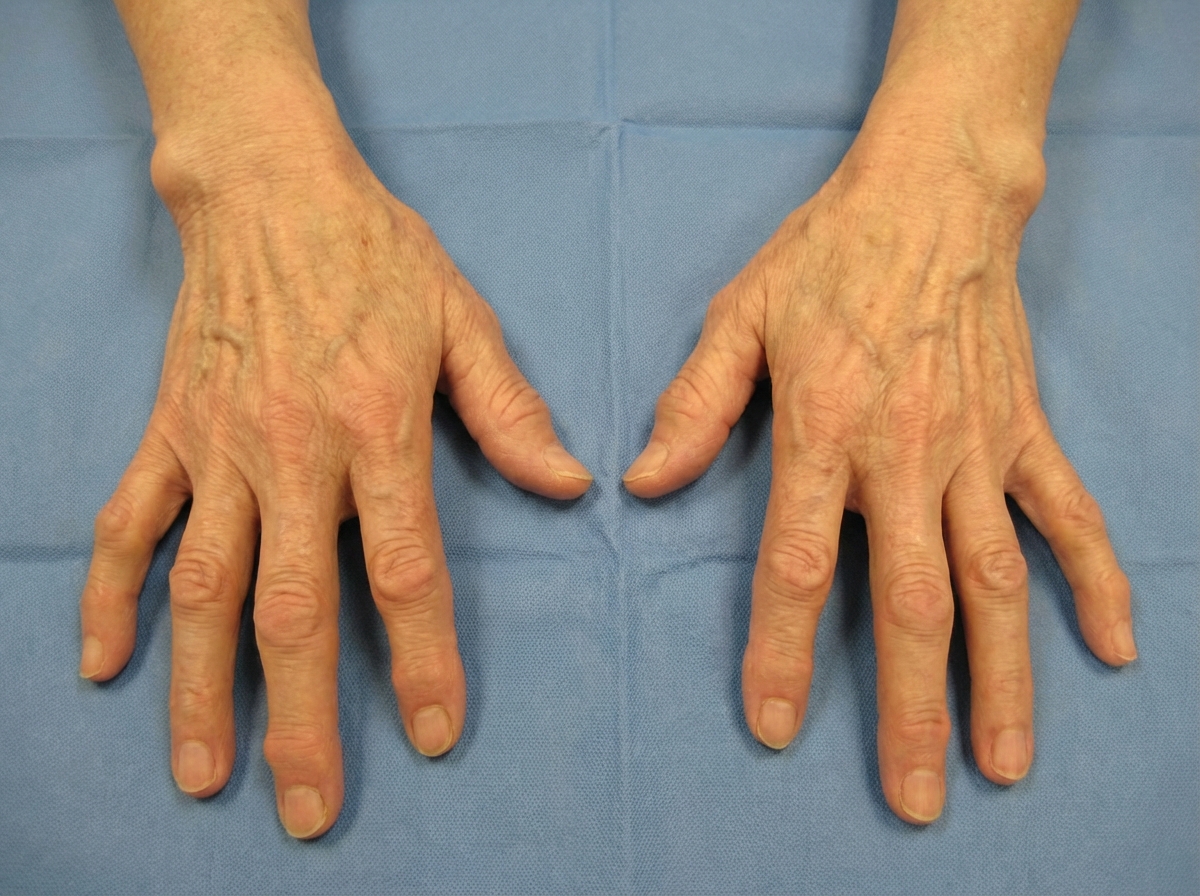
The deformity shown in the image is characteristic of which condition?
What is the term for painless effusion in congenital syphilis?
All are true about acute osteomyelitis except?
A patient presents with a ring-shaped (lytic) lesion in the bone. Which of the following is the most likely diagnosis?
An elderly patient with the following deformity was brought to the OPD. What is the most probable diagnosis? 
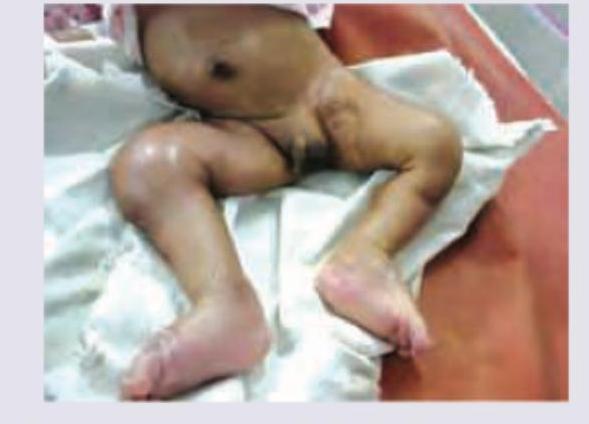
A 15-day-old neonate was brought with complaints of high grade fever for 2 days and decreased playing movements of right leg. On examination the right knee joint is red, tender and shows fluctuation. All are true about the condition shown except:
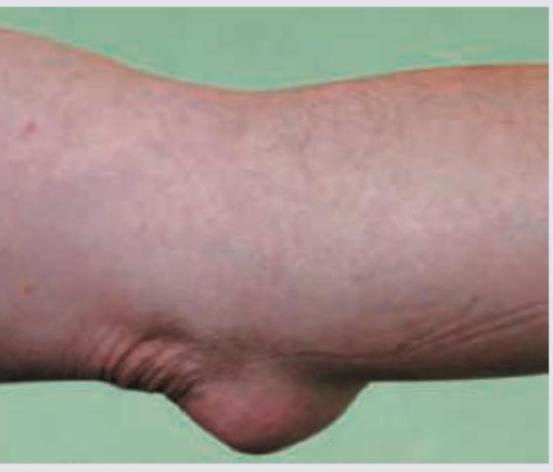
All the following statements regarding this image are true except: (Recent NEET Pattern 2016-17)
Practice by Chapter
Septic Arthritis
Practice Questions
Osteomyelitis
Practice Questions
Tuberculosis of Bones and Joints
Practice Questions
Fungal and Parasitic Infections
Practice Questions
Diabetic Foot Infections
Practice Questions
Prosthetic Joint Infections
Practice Questions
Reactive Arthritis
Practice Questions
Management of Joint Infections
Practice Questions
Prevention of Orthopaedic Infections
Practice Questions
Biofilms in Orthopaedic Infections
Practice Questions
Antibiotic Prophylaxis
Practice Questions
Implant-Related Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
