Prenatal Care — MCQs

On this page
The net effect of antenatal care has been the following EXCEPT:
Which one of the following statements regarding pre-conceptional counseling is NOT correct?
A 23-year-old woman presents at 10 weeks gestation with a positive rapid plasma reagin (RPR) titer of 1:64 and positive TPHA. She was treated for primary syphilis 2 years ago with appropriate penicillin therapy, after which her RPR declined to 1:2. She denies any new symptoms or sexual contacts since then. What is the most appropriate management?
What is the most appropriate topical treatment for external genital warts in pregnancy?
A 34-year-old pregnant woman at 28 weeks gestation is found to have a positive treponemal test (TPHA) but negative non-treponemal test (VDRL) during routine antenatal screening. She has no history of syphilis treatment. What is the most appropriate interpretation and management?
A pregnant woman presents with an IUD in place, and the thread is clearly visible. She wishes to continue the pregnancy. What is the most appropriate next step?
A woman has been using oral contraceptive pills (OCP) for 5 months and has had amenorrhea for the last 6 weeks. What is the best method to calculate the gestational age in this case?
A pregnant woman comes for a routine antenatal checkup. She had a history of a twin pregnancy one year ago. What is her gravida and para status?
The following cost-effective investigations are routinely recommended in the screening of antenatal mothers, EXCEPT:
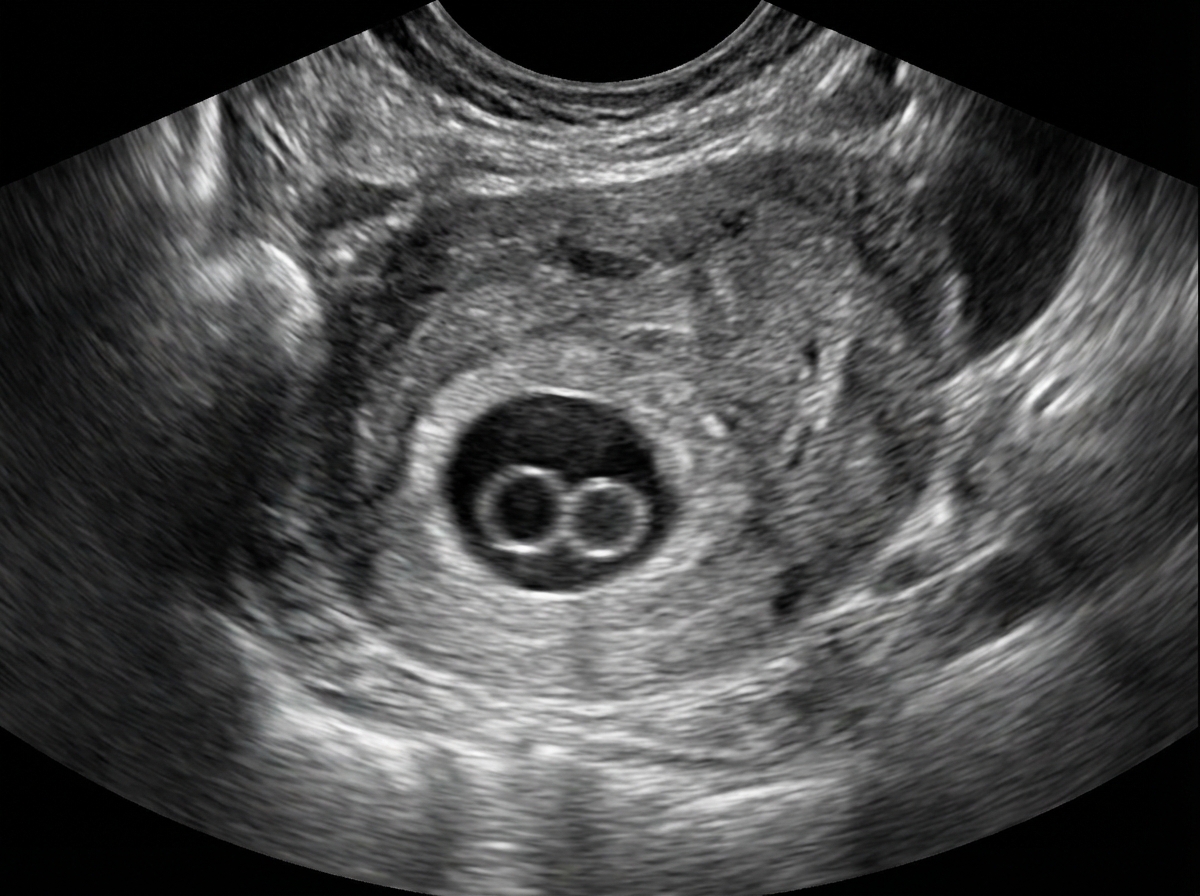
Double bleb sign seen in early pregnancy is due to?
Practice by Chapter
Preconception Counseling
Practice Questions
Pregnancy Diagnosis and Dating
Practice Questions
Routine Antenatal Assessments
Practice Questions
Maternal Physiological Changes
Practice Questions
Nutrition in Pregnancy
Practice Questions
Screening Tests in Pregnancy
Practice Questions
Fetal Growth Assessment
Practice Questions
High-Risk Pregnancy Identification
Practice Questions
Antenatal Complications Management
Practice Questions
Psychosocial Aspects of Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
