Prenatal Care — MCQs

On this page
A 20-year-old woman, gravida 2, para 0, aboa 1, presents for a prenatal visit at 30 weeks gestation. Her previous ultrasound at 18 weeks confirmed a single fetus appropriate for dates. She reports good fetal movement and has gained 9 kg. Today, her fundal height measures 25 cm, and fetal heart sounds are heard in the right upper quadrant. An obstetric ultrasound reveals an amniotic fluid index (AFI) of 4 cm. Which of the following conditions is most likely associated with this scenario?
Many professional organizations recommend that all pregnant women be routinely counseled about HIV infection and be encouraged to be tested. What is the most important reason for early identification of HIV infection in pregnant women?
What is the daily recommended dietary allowance for iodine during pregnancy?
The softening of the uterus with lateral implantation is called as?
Which of the following can be prevented by addressing modifiable risk factors?
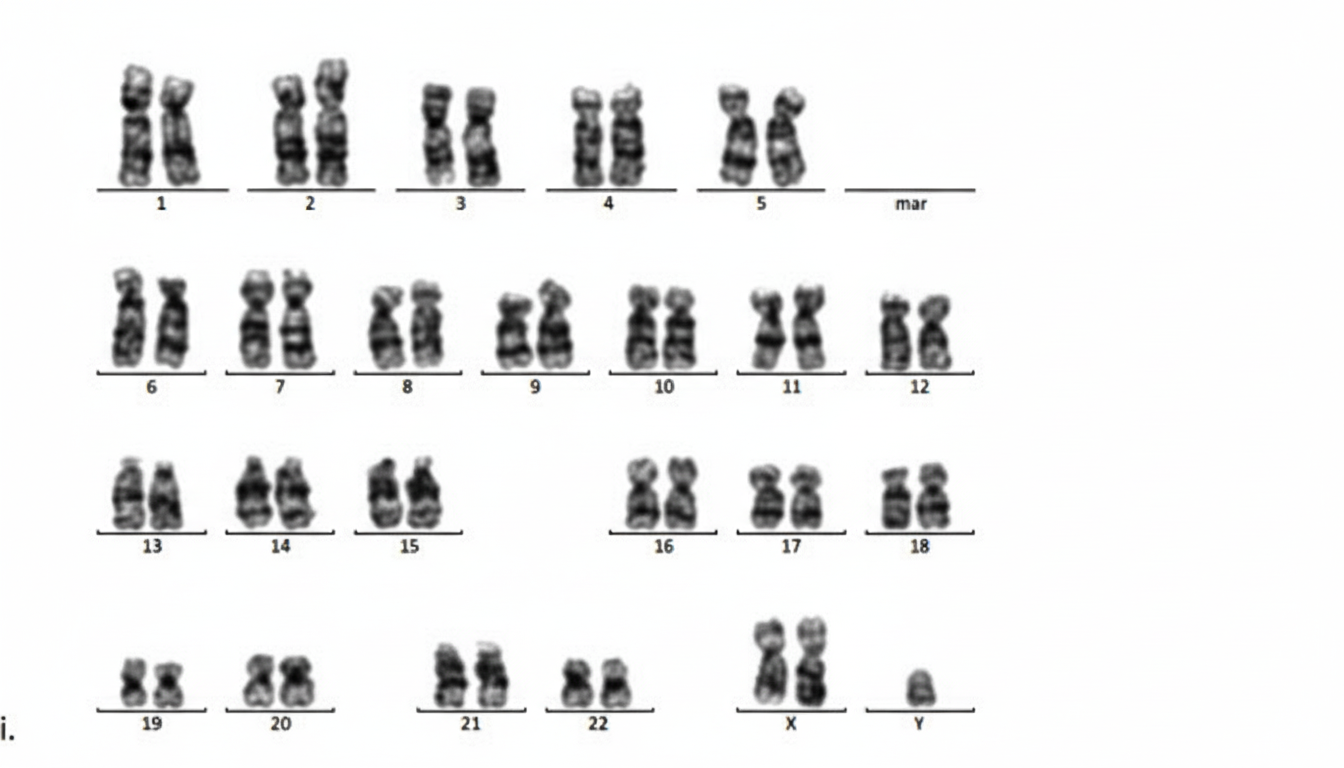
A married middle-aged female gives a history of repeated abortions for the past 5 years. The given below is a prenatal karyogram from one of her conceptions. This karyogram suggests which of the following?
Which of the following ultrasound features identified during the second trimester is NOT a marker of Down syndrome?
A 42-year-old primigravida presents to your office for a routine OB visit at 34 weeks gestational age. She voices concern because she has noticed an increasing number of spidery veins appearing on her abdomen. She is upset with the unsightly appearance of these veins and wants to know what you recommend to get rid of them. How do you advise this patient?
Which of the following tests on maternal serum is most useful in distinguishing between open neural tube defects and ventral wall defects?
Which of the following evaluation methods is most sensitive in diagnosing pregnancy early?
Practice by Chapter
Preconception Counseling
Practice Questions
Pregnancy Diagnosis and Dating
Practice Questions
Routine Antenatal Assessments
Practice Questions
Maternal Physiological Changes
Practice Questions
Nutrition in Pregnancy
Practice Questions
Screening Tests in Pregnancy
Practice Questions
Fetal Growth Assessment
Practice Questions
High-Risk Pregnancy Identification
Practice Questions
Antenatal Complications Management
Practice Questions
Psychosocial Aspects of Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
