Virology — MCQs

On this page
A patient presents with genital grouped vesicles, as shown in the image. What is the most likely causative organism?
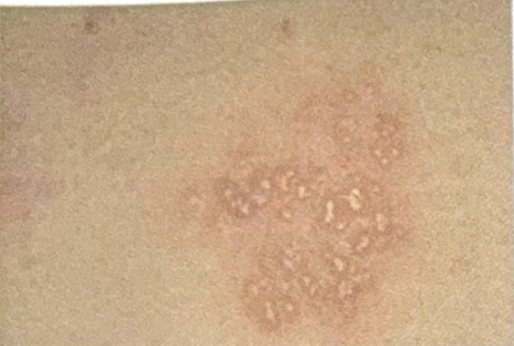
Which of the following statements about herpes simplex virus (HSV) shedding is MOST accurate?
A child presented with bluish-white spots in the mouth followed by a rash. What is the genome of the most likely causative agent?
The viruses of the Filoviridae family like Ebola and Marburg resemble which of the following morphologies?
Which of the following is true about anti-CMV IgG antibodies?
A 35-year-old woman presents with painful genital ulcers that recur every few months. Current examination reveals multiple shallow ulcers on the labia minora. PCR testing is positive for HSV-2. Which of the following best explains the mechanism of viral latency in this condition?
How does HSV establish latency in the host?
Which type of HSV is most commonly associated with recurrent genital herpes?
Which cytopathic effect would confirm molluscum contagiosum virus infection?
A viral culture shows 'ground glass' nuclear appearance. Which inclusion body would confirm cytomegalovirus infection?
Practice by Chapter
Virus Structure and Classification
Practice Questions
Viral Replication
Practice Questions
Pathogenesis of Viral Infections
Practice Questions
DNA Viruses: Herpesviruses
Practice Questions
DNA Viruses: Poxviruses and Adenoviruses
Practice Questions
Hepatitis Viruses
Practice Questions
RNA Viruses: Orthomyxoviruses
Practice Questions
RNA Viruses: Paramyxoviruses
Practice Questions
Enteroviruses and Rhinoviruses
Practice Questions
Arboviruses
Practice Questions
HIV and Retroviruses
Practice Questions
Oncogenic Viruses
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
