Virology — MCQs

On this page
All of the following statements are true regarding poliovirus, except:
What is the causative agent for a lesion on the penis?
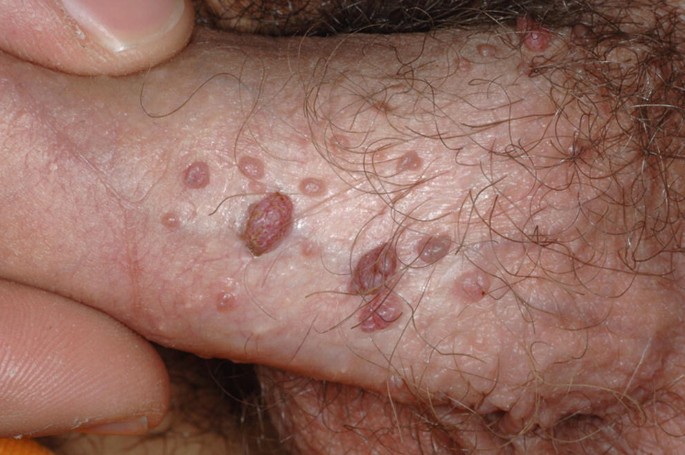
What change does HPV cause in the cervical epithelium?
Hepatitis E clinically resembles which other form of hepatitis?
Which of the following is associated with acute hemorrhagic conjunctivitis?
Presence of HBeAg in patients with Hepatitis B infection indicates what?
All of the following are true about Herpes group viruses except?
Which of the following viruses belongs to the Caliciviridae family?
Which influenza strain was isolated in 1989 and subsequently spread to many other countries?
A person had unprotected sex 3 weeks ago. What is the best test to rule out HIV infection at this stage?
Practice by Chapter
Virus Structure and Classification
Practice Questions
Viral Replication
Practice Questions
Pathogenesis of Viral Infections
Practice Questions
DNA Viruses: Herpesviruses
Practice Questions
DNA Viruses: Poxviruses and Adenoviruses
Practice Questions
Hepatitis Viruses
Practice Questions
RNA Viruses: Orthomyxoviruses
Practice Questions
RNA Viruses: Paramyxoviruses
Practice Questions
Enteroviruses and Rhinoviruses
Practice Questions
Arboviruses
Practice Questions
HIV and Retroviruses
Practice Questions
Oncogenic Viruses
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
