Arboviruses — MCQs

KFD is transmitted by:
Japanese encephalitis is caused by which virus?
Vector for Zika virus disease is:
Patient: fever, joint pain, rash. Recent history of mosquito bite. Most likely diagnosis in urban area?
Which virus is most commonly recognized as a prototypical viral hemorrhagic fever in endemic regions of West Africa?
Gram stain of CSF shows gram-negative diplococci. Culture grows on Thayer-Martin medium. Most likely organism?
Subdural empyema is most commonly caused by:
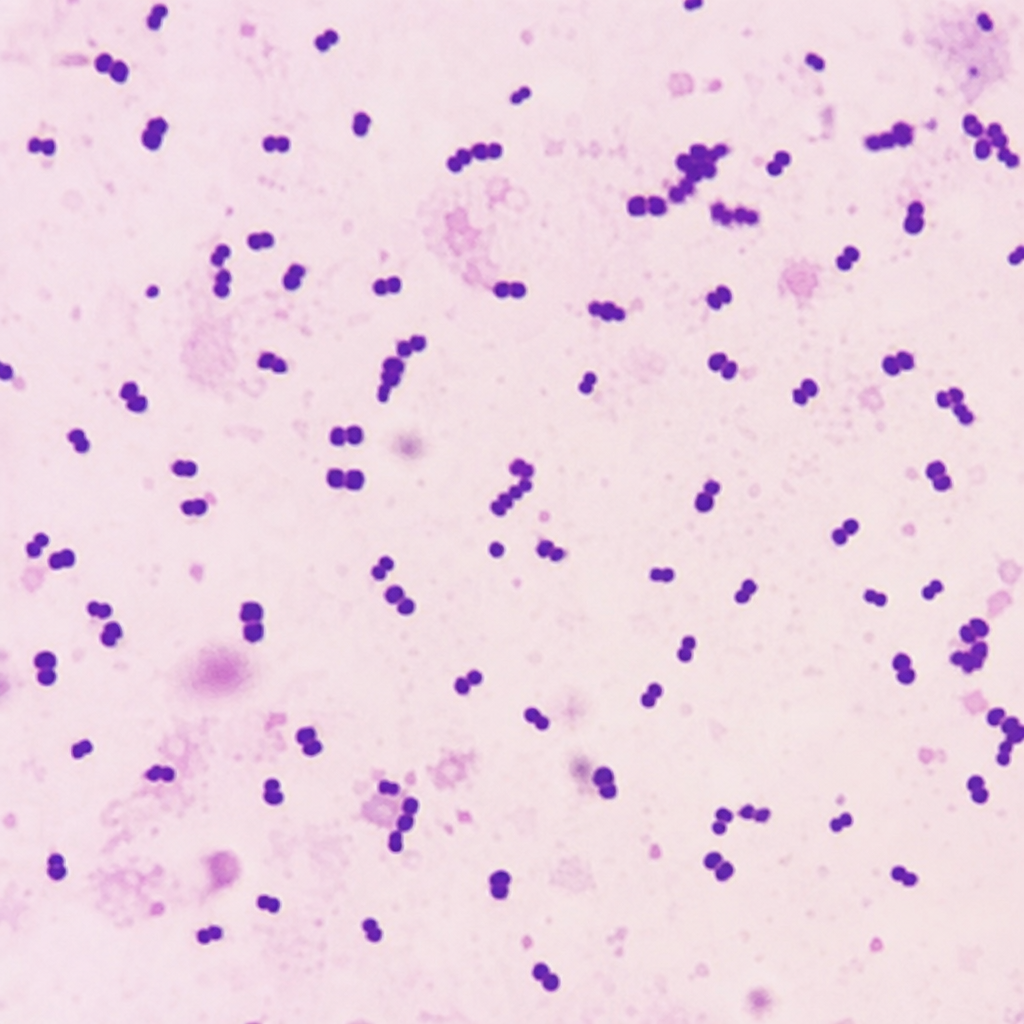
A patient presented with meningitis, and the CSF sample was subjected to gram staining and microscopy and appears as shown in the microscopic image given below. Which of the following features / tests will be characteristic of the organism?
After 5 days of birth, a baby developed poor feeding, convulsions, fever, high protein, low sugar, and low chloride levels in the cerebrospinal fluid. This is most likely due to what?
A 9-year-old child presented to OPD with complaints of high-grade fever, vomiting, and one episode of seizure. CSF examination was done and Gram staining of the culture showed lanceolate-shaped gram-positive diplococci. What is the probable causative agent?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
