Mycology — MCQs

On this page
Aseptate hyphae and asexual spores are seen with which of the following?
Rhinosporidium seeberi grows in which of the following?
Which of the following are neurotropic fungi?
A HIV-positive female presents with an indurated ulcer over the tongue. Laboratory findings show growth in cornmeal agar at 20°C, microscopy showing hyphae, and growth in human serum at 37°C showing budding yeasts. What is the probable causative agent?
All of the following are true regarding Cryptococcus neoformans except?
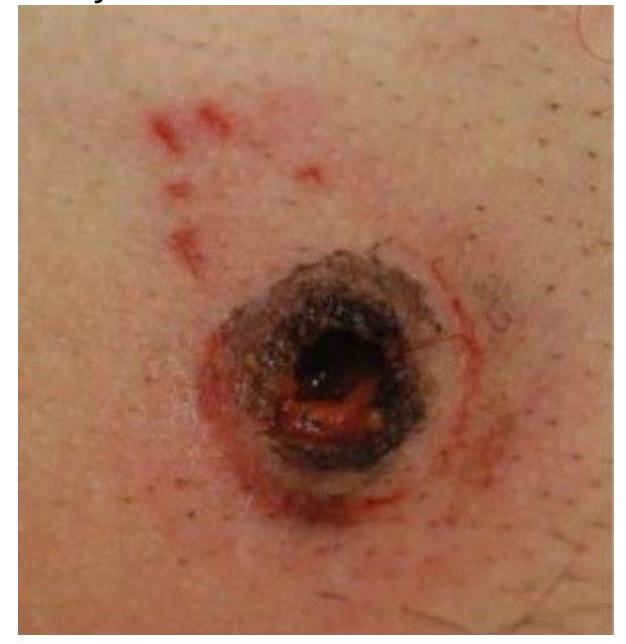
What is the likely cause of this manifestation?
Which of the following are endemic fungal infections?
Candidiasis is a complication of all of the following except?
Darlings disease is:
What is the causative organism in Madura Mycosis?
Practice by Chapter
Classification of Fungi
Practice Questions
Superficial Mycoses
Practice Questions
Dermatophytes
Practice Questions
Subcutaneous Mycoses
Practice Questions
Candidiasis
Practice Questions
Aspergillosis
Practice Questions
Cryptococcosis
Practice Questions
Zygomycosis
Practice Questions
Endemic Mycoses
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Antifungal Agents
Practice Questions
Laboratory Diagnosis of Fungal Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
