Mycology — MCQs

On this page
Vascular invasion is a characteristic feature of which of the following fungal infections?
Confirmation of Cryptococcus species is done by all the following methods except?
The clinical appearance shown in the image is caused by which organism?
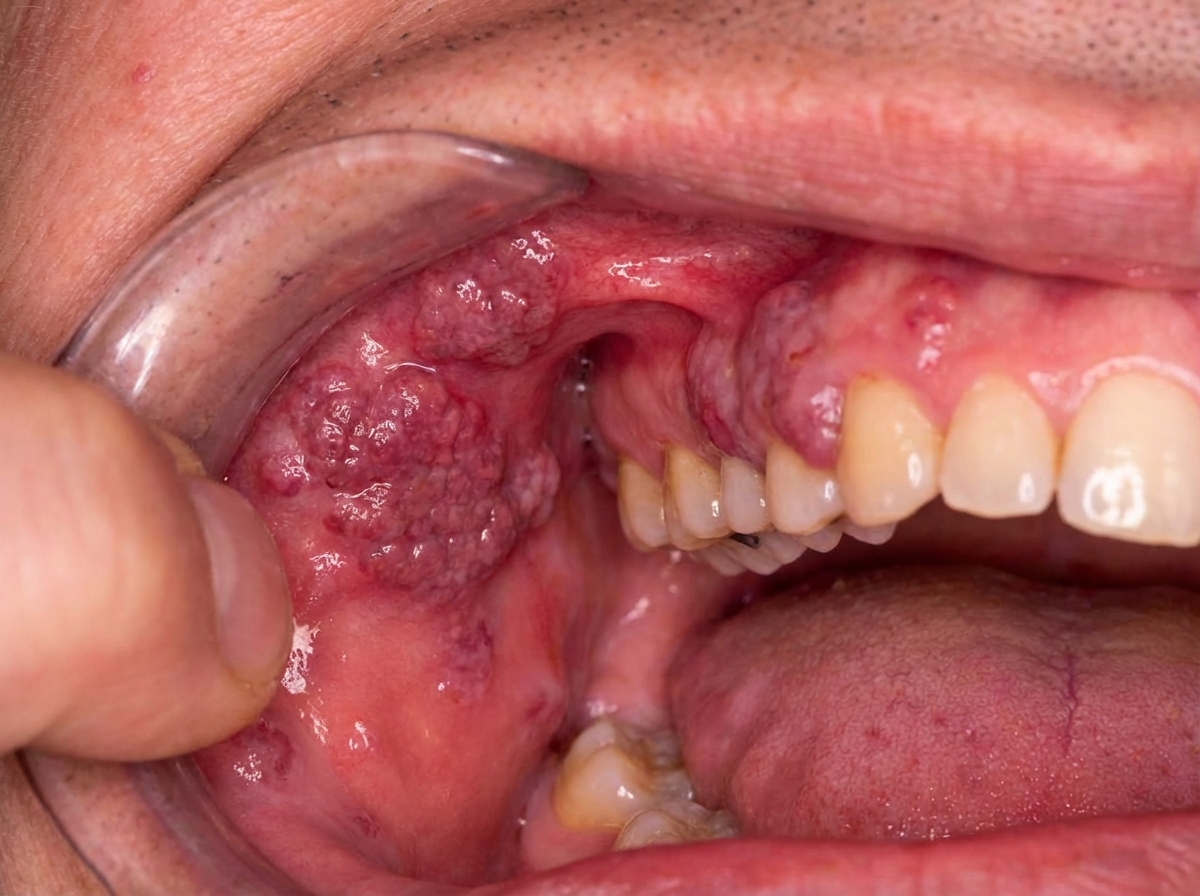
Which of the following fungi infects hair, skin, and nails?
The 'cigar body' yeast form is characteristic of which of the following fungal infections?
Which test is used for the diagnosis of Pneumocystis jirovecii?
What is true about Echinococcus Granulosus?
What is the most common causative agent for meningitis in the immunocompromised patient?
Which of the following fungal infections is characterized by vascular involvement and thrombosis?
Meningitis caused by Cryptococcus neoformans is most often acquired by?
Practice by Chapter
Classification of Fungi
Practice Questions
Superficial Mycoses
Practice Questions
Dermatophytes
Practice Questions
Subcutaneous Mycoses
Practice Questions
Candidiasis
Practice Questions
Aspergillosis
Practice Questions
Cryptococcosis
Practice Questions
Zygomycosis
Practice Questions
Endemic Mycoses
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Antifungal Agents
Practice Questions
Laboratory Diagnosis of Fungal Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
