Mycology — MCQs

On this page
What is the most common cause of persistent vaginal candidiasis despite appropriate antifungal therapy?
A patient in the ICU with a central venous catheter (CVC) develops an infection. Microscopy reveals ovoid budding yeast cells. What is the most likely organism?
Broad-based budding yeasts are seen in:
Desert rheumatism is caused by:
A hair perforation test was performed on a yeast isolate, and the result was positive. Which of the following organisms is associated with a positive hair perforation test?
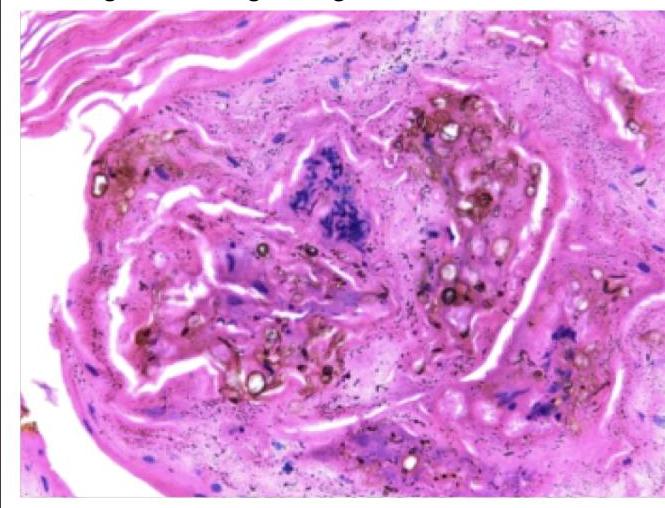
A forest worker developed skin lesions over the forearm, which initially started as macules but then became nodules. Histology of the nodule shows the following findings. Which of the following is true regarding this condition?
A man has undergone renal transplant and is taking immunosuppressant drug. On biopsy there was presence of budding cells with pseudohyphae. Identify the organism?
Identify the correct 'organism-drug to which it is intrinsically resistant' pair.
A 34-year-old woman presents with multiple round, scaly patches on her chest and back. The lesions are hypopigmented and slightly pruritic. KOH preparation of skin scrapings shows short, angular hyphae. Which of the following best describes the causative organism's morphology in culture?
A fungal culture shows 'rising sun' pattern. Which microscopic finding would confirm Microsporum canis?
Practice by Chapter
Classification of Fungi
Practice Questions
Superficial Mycoses
Practice Questions
Dermatophytes
Practice Questions
Subcutaneous Mycoses
Practice Questions
Candidiasis
Practice Questions
Aspergillosis
Practice Questions
Cryptococcosis
Practice Questions
Zygomycosis
Practice Questions
Endemic Mycoses
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Antifungal Agents
Practice Questions
Laboratory Diagnosis of Fungal Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
