Mycology — MCQs

On this page
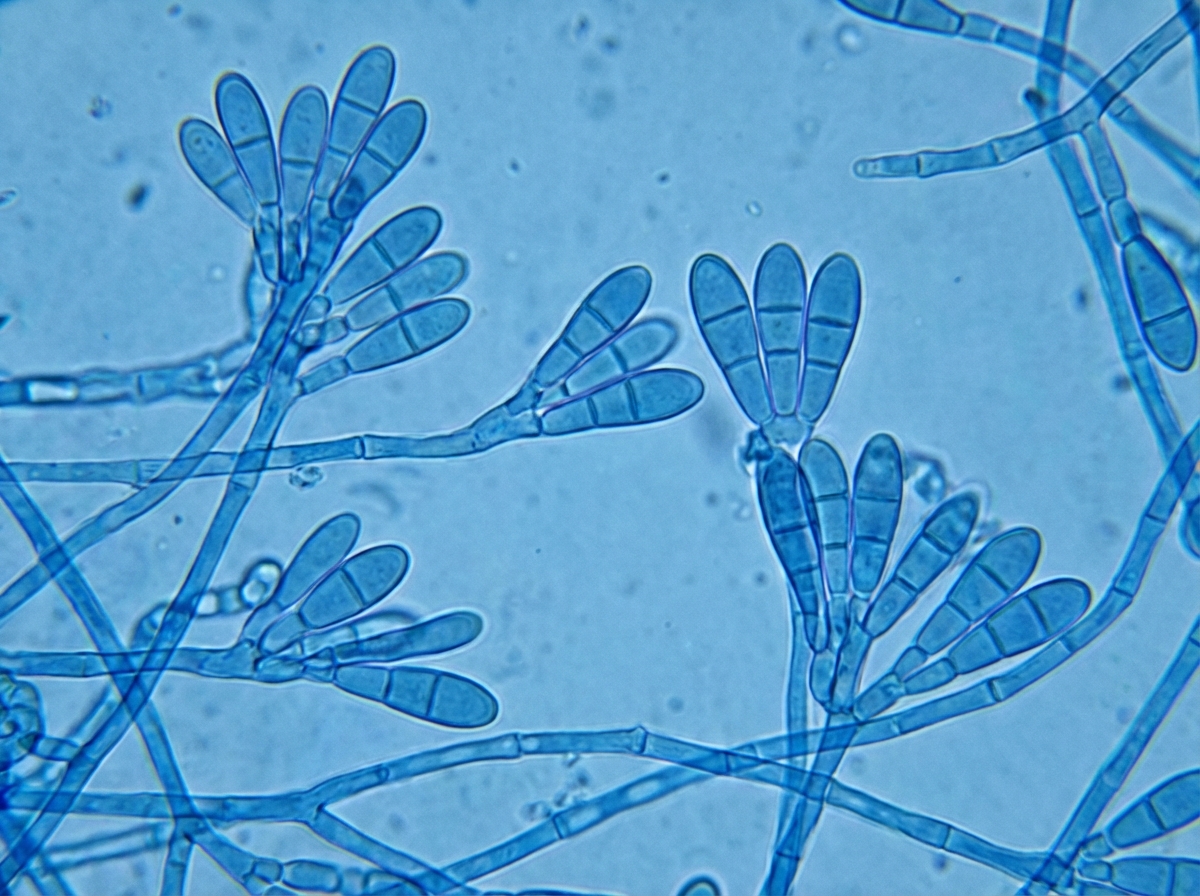
An 18-year-old white male high-school student presents with a diffuse, painful rash on his thighs extending to his navel. He reports using topical hydrocortisone from a teammate for a previous groin rash. A KOH scraping of the current lesion shows hyaline hyphae. A schematic of the microscopic observation of the culture is provided. What is the most likely etiology?
What is the most important risk factor for invasive aspergillosis?
Renauld-Braud phenomenon is seen in which of the following?
Which of the following is NOT an 'all except' characteristic of acute pseudomembranous candidiasis?
Mycetoma is caused by the following agents except?
Which of the following stains is used to detect the capsule of Cryptococcus neoformans in a CSF sample?
Black coloured hard nodules in hair are produced by which organism?
A 28-year-old HIV-positive male complains of pain on swallowing. Physical examination is remarkable for white plaque-like material on his tongue and buccal mucosa, which is scraped and sent to the laboratory. Based on these findings and the laboratory results, the man is diagnosed with acquired immunodeficiency syndrome (AIDS). With which of the following agents is the man most likely infected?
Which staining method is used to identify Cryptococcus neoformans?
Which of the following is an occupational disease of gardeners?
Practice by Chapter
Classification of Fungi
Practice Questions
Superficial Mycoses
Practice Questions
Dermatophytes
Practice Questions
Subcutaneous Mycoses
Practice Questions
Candidiasis
Practice Questions
Aspergillosis
Practice Questions
Cryptococcosis
Practice Questions
Zygomycosis
Practice Questions
Endemic Mycoses
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Antifungal Agents
Practice Questions
Laboratory Diagnosis of Fungal Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
