Mycology — MCQs

On this page
Which of the following is NOT a cause of Madura foot?
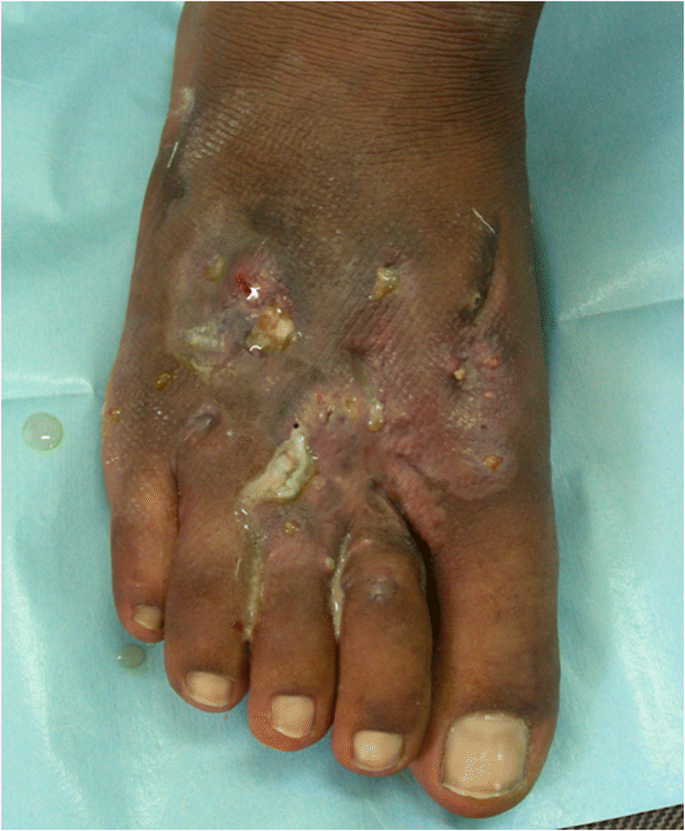
A 40-year-old man presented with swelling over his foot with multiple sinus discharge. What is the likely diagnosis?
Cigar-shaped yeast cells are seen with which of the following organisms?
All of the following are dimorphic fungi EXCEPT:
Madura foot is caused by?
A man developed a pustule after being pricked by a thorn in the garden. Laboratory examination of the tissue specimen shows cigar-shaped budding yeasts. What is the most probable causative agent?
Which of the following statements about mucormycosis is TRUE?
Penicillium marneffei is commonly associated with which of the following conditions?
Pneumocystis jirovecii causes infection primarily in which species?
All of the following forms sulphur granules except?
Practice by Chapter
Classification of Fungi
Practice Questions
Superficial Mycoses
Practice Questions
Dermatophytes
Practice Questions
Subcutaneous Mycoses
Practice Questions
Candidiasis
Practice Questions
Aspergillosis
Practice Questions
Cryptococcosis
Practice Questions
Zygomycosis
Practice Questions
Endemic Mycoses
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Antifungal Agents
Practice Questions
Laboratory Diagnosis of Fungal Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
