Mycology — MCQs

On this page
Sclerotic bodies 3-15 microns in size, multiseptate, and chestnut brown in colour are seen in which condition?
Which of the following is the commonest cause of farmer's lung?
The organism most frequently related to mediastinal fibrosis is?
For examination of fungus from a sample, which stain is uniformly used?
A section of tissue from the foot of a person with Eumycotic mycetoma shows a white, lobulated granule composed of fungal hyphae. What is the most common etiologic agent of this condition?
A KOH wet mount is prepared for which of the following?
Discharging sinus is seen in which of the following conditions?
All are true regarding filariasis EXCEPT?
All of the following are bacterial diseases except:
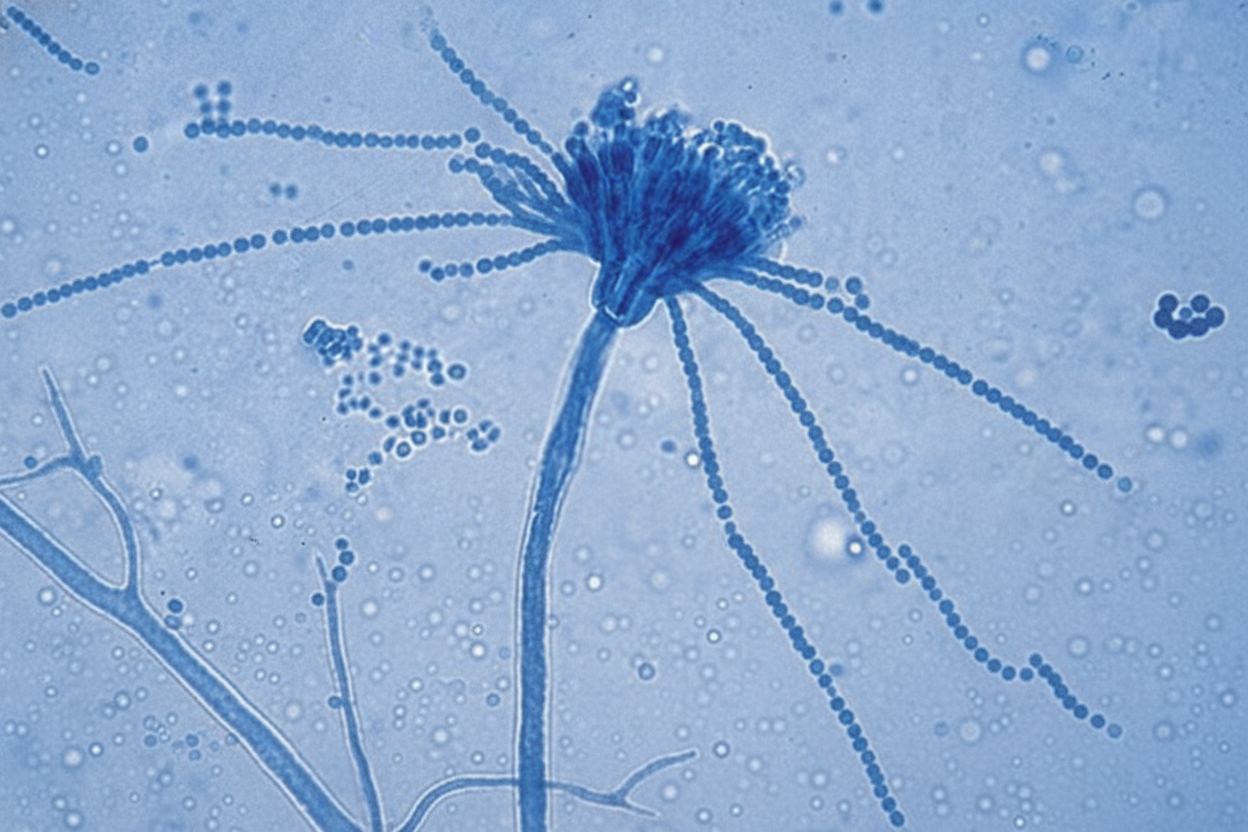
The organism shown below is:
Practice by Chapter
Classification of Fungi
Practice Questions
Superficial Mycoses
Practice Questions
Dermatophytes
Practice Questions
Subcutaneous Mycoses
Practice Questions
Candidiasis
Practice Questions
Aspergillosis
Practice Questions
Cryptococcosis
Practice Questions
Zygomycosis
Practice Questions
Endemic Mycoses
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Antifungal Agents
Practice Questions
Laboratory Diagnosis of Fungal Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
