Classification of Fungi — MCQs

A 55-year-old woman presents with persistent cough, fever, and hemoptysis. Sputum shows branching septate hyphae. What is the likely pathogen?
A patient presented with some unknown fungal infection. Microscopic examination revealed brown coloured spherical fungi with septate hyphae. Possible condition:
Broad-based budding yeasts are seen in:
What type of spore is produced by Ascomycota during sexual reproduction?
Aseptate hyphae is not seen in which of the following fungi?
All are correct about the image shown except:

Beta 1,3 Glucan test is positive in all except?
Which statement is false regarding Cryptococcus neoformans?
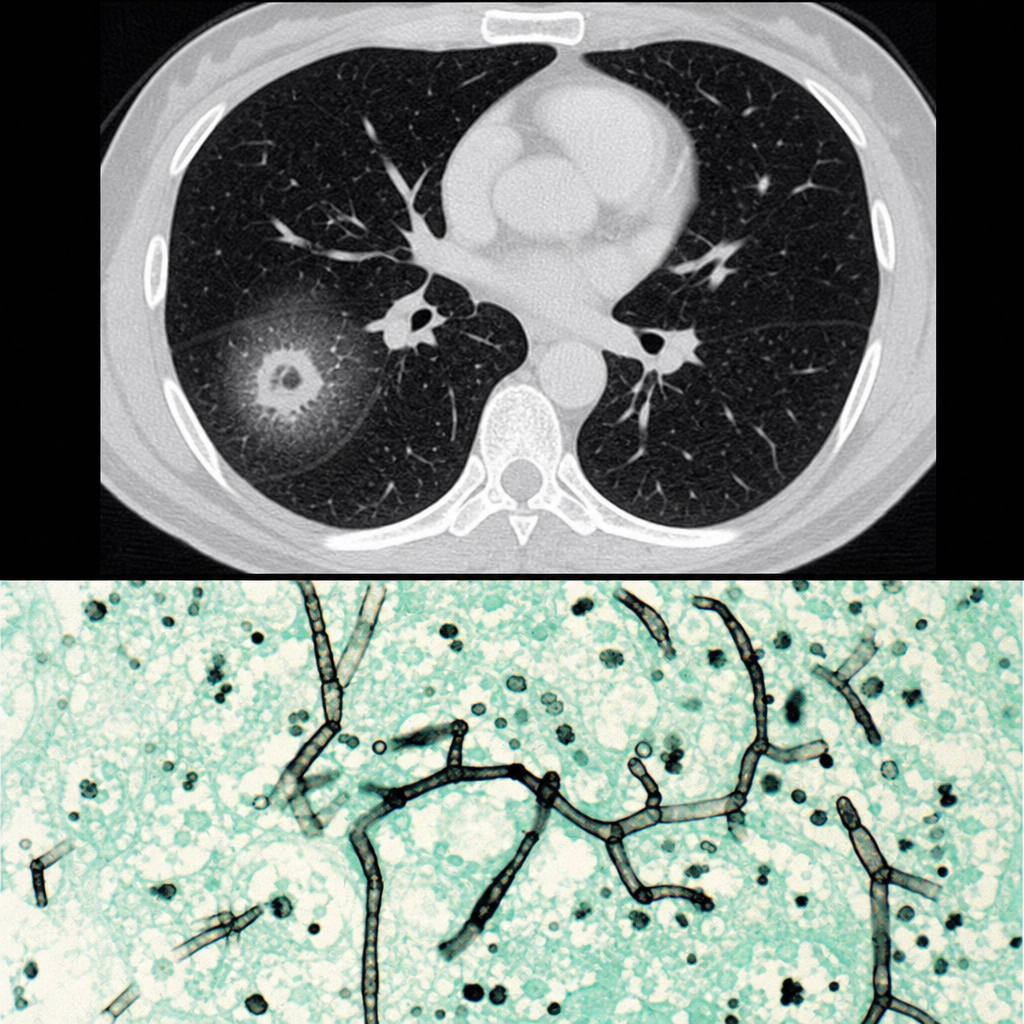
About 90 days post-bone marrow transplant, a 55-year-old white woman began to complain of dry cough, shortness of breath, and chest pain. She was started on antibiotics and blood culture obtained at the time was negative and there was not improvement. A computed tomography (CT) scan of the lungs showed a halo of low attenuation around a nodular lesion. Analysis of lung biopsy was similar to methenamine silver-stained section below. What is the most likely diagnosis for this patient?
Brown, spherical, septate bodies found in pus are diagnostic of which condition?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
