Respiratory Microbiome — MCQs

A 6-year-old boy presents with fever and chills, cough, rapid breathing, difficulty breathing, and chest pain. A culture from a respiratory sample shows Gram-positive bacteria. What is the most likely organism causing this infection?
Which pathogen is most commonly associated with a productive cough in chronic bronchitis?
A patient with a cavitary lung lesion who coughs up sputum containing thin, acid-fast positive rods. Which of the following features would most likely be associated with these bacteria?
Which is the MOST COMMON cause of atypical pneumonia in the community setting?
A 12-year-old girl presents with fever, shortness of breath, and cough. A chest X-ray reveals complete consolidation of the left lower lung lobe. What is the most probable organism?
Which of the following bacteria is microaerophilic?
NOT a cause of bacterial community acquired pneumonia:
Which is the most common bacterial organism causing bacterial upper respiratory tract infections (including sinusitis, otitis media, and pharyngitis) in adults?
Brain abscess in immunodeficient person is due to :
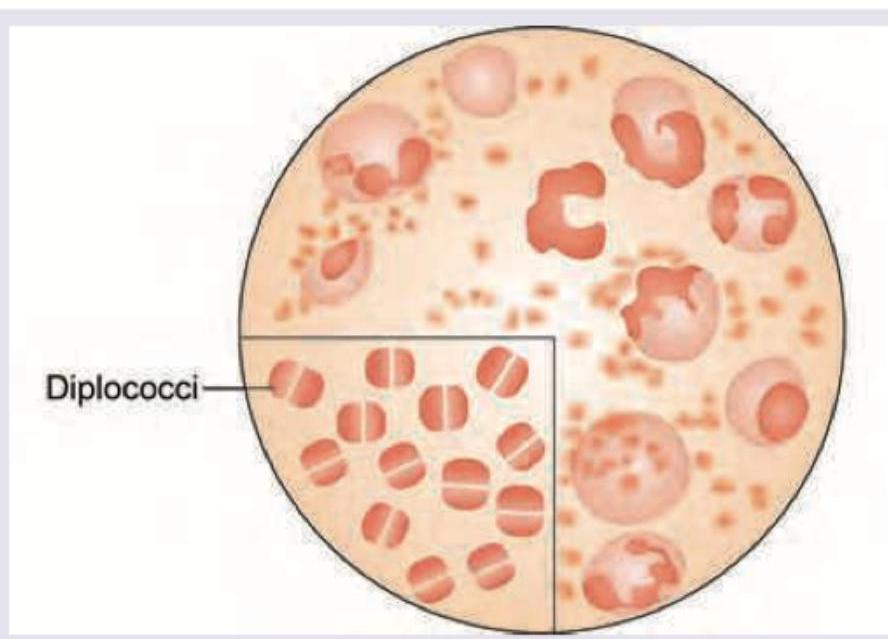
All are true about the bacteria shown in the figure except: (Recent NEET Pattern 2016-17)
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
