Skin and Soft Tissue Infections — MCQs

What is the diagnosis of an umbilicated, pearly white, asymptomatic skin lesion?
A diabetic patient developed cellulitis due to S. aureus, which was found to be methicillin resistant on the antibiotic sensitivity testing. All of the following antibiotics will be appropriate except ?
A diabetic patient presents with sudden-onset perineal pain. On examination, foul-smelling discharge and necrotic tissue are noted. Which of the following is the most characteristic feature of this condition?
A 50-year-old diabetic presents with a foot ulcer. Which pathogen is most likely?
What is the first-line treatment for gas gangrene?
Which of the following conditions is caused by Staphylococcus aureus?
Cellulitis is characterized as:
A child presents with grouped vesicles on the lips. What is the bedside investigation that you would like to do?
A 50-year-old diabetic presents with a foot ulcer. Which pathogen is most likely?
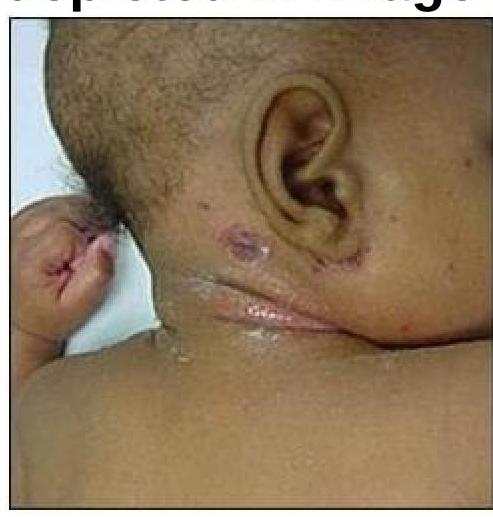
What is the causative organism for the condition depicted in the image?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
