Gastrointestinal Infections — MCQs

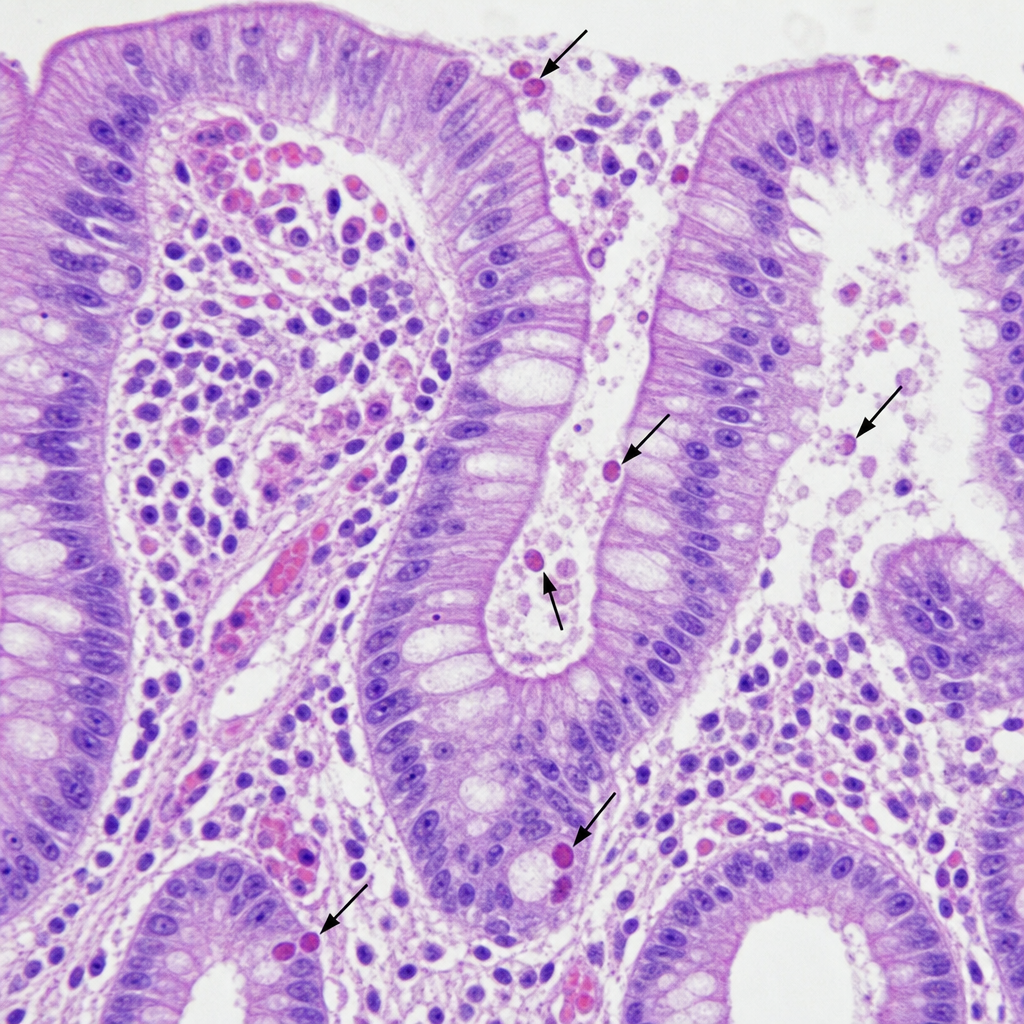
A 35-year-old heterosexual patient diagnosed with HIV presents with watery diarrhea. The colonoscopic biopsy is shown below. Which of the following is your most probable diagnosis?
A child with fever with abdominal cramps & pus in stools, causative organism is ?
A tourist with a travel history to India presents with complaints of abdominal pain and multiple episodes of watery diarrhea. He reports having food at a local restaurant the previous night. Which of the following antidiarrheal agents is used in this condition?
A 17 year old adolescent, presented with fever since one week which is step-ladder in pattern. He also has loose stools which are "pea-soup" in consistency. Rose spots are seen on his body. He is most probably infected with:
The most common causative organism for traveler's diarrhea is which of the following?
A 7-year-old girl passed 15 stools in the last 24 hours and vomited thrice in the last 4 hours. She is irritable but drinking fluids. What is the optimal therapy?
All of the following cause hemolytic uremic syndrome except
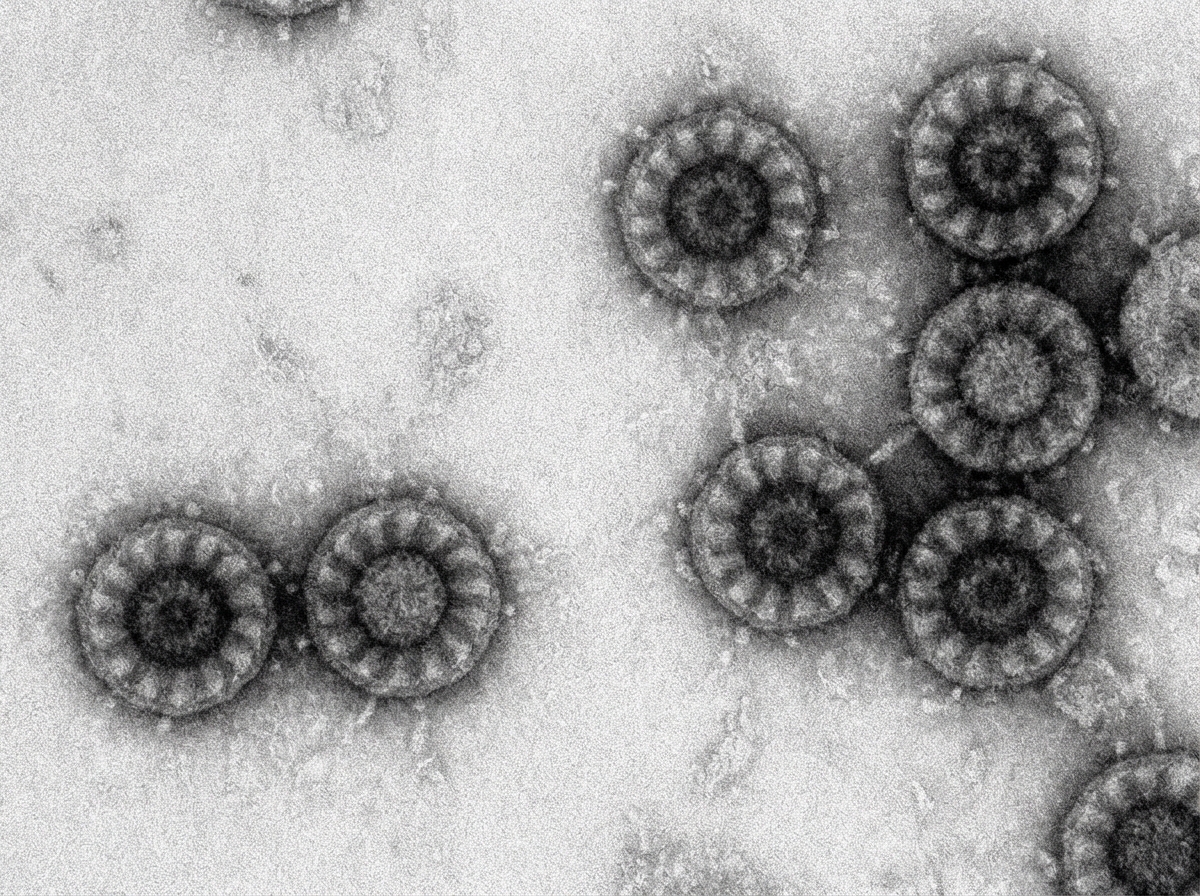
A 2 year old child came with watery diarrhea. Electron Microscopy (EM) Image is shown here. Choose the correct pathogen.
Patient presenting with abdominal pain, diarrhea taking clindamycin for 5 days. Treated with metronidazole symptoms subsided. What is the causative agent -
Traveller's diarrhoea is caused by:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
