Central Nervous System Infections — MCQs

Which of the following is NOT typically seen in cerebrospinal fluid (CSF) in tubercular meningitis?
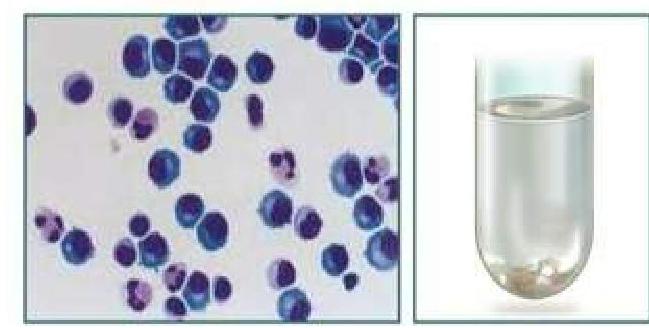
A patient comes to ED with fever and headache. On examination he has neck stiffness. CSF analysis was done: Glucose 55 mg/dl (normal 50-80), Protein 0.50 g/L (normal 0.18-0.45), ICT 35 cmH2O (normal 5-20), WBC 25 (predominantly lymphocytes). Most likely diagnosis is:
CSF in meningococcal meningitis shows -
Herpes virus involves which lobe?
A patient with a history of chronic ear infection now presents with manifestations, including headache and vomiting. A CT brain image is shown. What is the most probable diagnosis?

Brain abscesses in cyanotic heart disease are commonly located in
All of the following statements are true regarding central nervous system infections, except:
A young child with recurrent bacterial meningitis should be clinically evaluated for the presence of
Which of the following is the MOST accurate statement about CSF?
In severe CNS infections in children with complications, treatment may include:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
