Immunology — MCQs

On this page
Which cells secrete Interferon gamma?
What reaction is due to the lysis of bacterial cell wall and necrotic cell products?
Perforins are produced by which of the following cells?
Which one of the following statements best describes immunological tolerance?
A 27-year-old male patient with blood group O presents with massive intestinal bleeding and has lost half his blood volume. He is transfused with blood group AB blood. Within minutes, he develops fever, chills, dyspnea, and a dramatic drop in blood pressure. What is the most likely cause of this reaction?
All are true regarding superantigens except?
All of the following agents have polysaccharide capsule related antigen-antibody responses, EXCEPT?
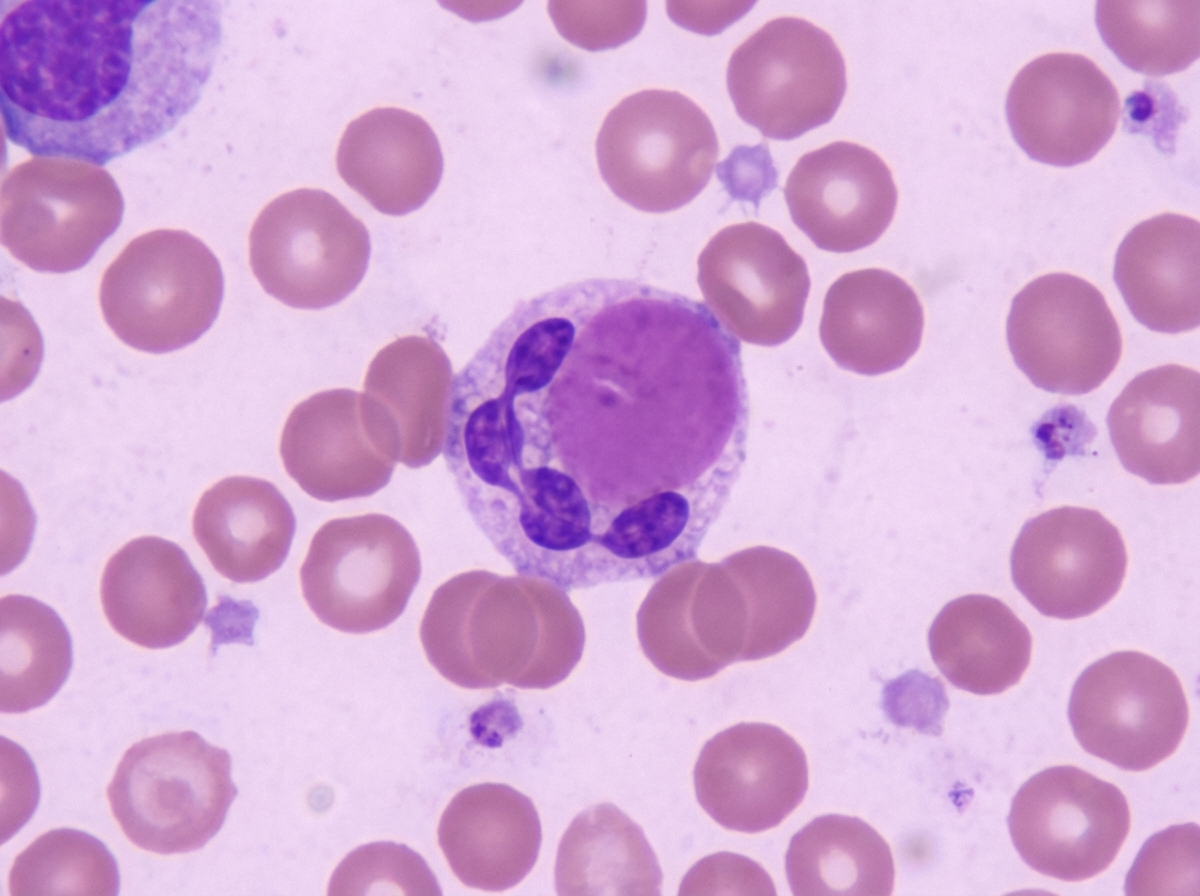
The image shows a cellular finding in a peripheral blood smear. This finding is most characteristic of which condition?
The Weil-Felix reaction is based on the sharing of antigens between which of the following?
Which ion controls the activity of the classical complement pathway (C1)?
Practice by Chapter
Cells and Organs of Immune System
Practice Questions
Innate Immunity
Practice Questions
Adaptive Immunity
Practice Questions
Antigens and Antibodies
Practice Questions
Major Histocompatibility Complex
Practice Questions
Complement System
Practice Questions
Cytokines and Chemokines
Practice Questions
Hypersensitivity Reactions
Practice Questions
Autoimmunity and Autoimmune Diseases
Practice Questions
Immunodeficiency Disorders
Practice Questions
Transplantation Immunology
Practice Questions
Tumor Immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
