Bacterial Identification Techniques — MCQs

A frequent traveler presented with 4 days of continuous fever, abdominal pain, and bradycardia. What is the best diagnostic test to confirm the pathogen?
What is the best investigation for identifying malaria species?
A child presented with bloody stools and abdominal pain. Which enrichment medium should be used for processing the fecal sample?
A farmer presents to the emergency department with painful inguinal lymphadenopathy and a history of fever and flu-like symptoms. Clinical examination reveals an ulcer on the leg. Which of the following stains should be used to detect suspected bipolar-stained organisms?
A farmer presents with pustules that show Gram-positive cocci on smear. The culture shows beta hemolysis, and the organisms are catalase-negative. To confirm that the identified organism is group A streptococcus, which of the following tests should be performed?
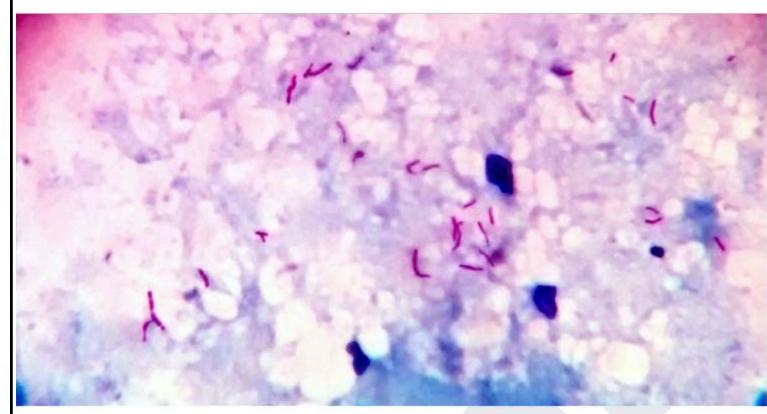
A 32 year old laborer working at a construction site presented with fever and hemoptysis. The sputum sample collected for examination showed the following. The smear will be stained by which of the following sequences?
A patient presented with meningitis, and the CSF sample shows Gram-negative diplococci on Gram staining and microscopy. Which of the following features/tests will be characteristic of the organism?
Most sensitive test for detecting microfilariae?
A female patient presents with dysuria and frequency. A coagulase-negative, novobiocin-resistant Staphylococcus species (>10^4 CFU/mL) was grown in urine culture. What does this indicate?
A patient with a suspected bacterial infection undergoes an antigen-antibody reaction test for pathogen identification. Which of the following is a key characteristic of such immunological tests?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
