Toxicology and Overdose Management — MCQs

On this page
What is the initial management for a snake bite?
Antifreeze ingestion leads to which of the following?
A 32-year-old lethargic male presented to the emergency department with a history of drug consumption. Investigations revealed hypocalcemia, serum creatinine of 3.8 mg/dL, and elevated BUN. Arterial blood gas analysis showed metabolic acidosis. Urine examination revealed calcium oxalate crystals. The patient was treated with 4-methylpyrazole. What is the most probable drug ingestion leading to this condition?
Hemodialysis is useful in treating poisoning with all of the following agents, EXCEPT:
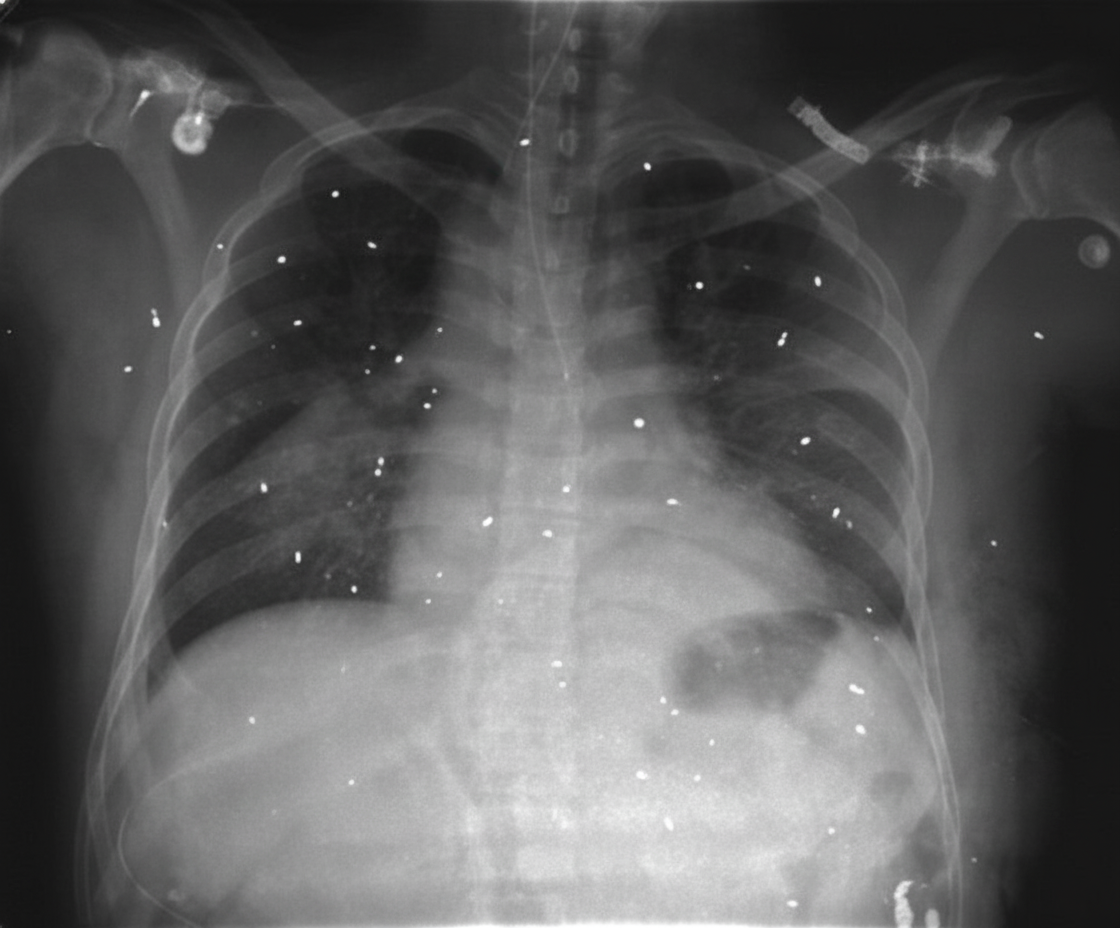
A 29-year-old man with a history of substance abuse presented with headache, fever, and metallic taste in his mouth. His physical exam was normal except for needle tracks in his right arm. A chest X-ray was performed. Based on the chest X-ray findings, what is the most likely diagnosis?
A young man with a known history of heroin addiction is brought to the emergency department in an unconscious state by his friends. On examination, his pupils are pinpoint. What is the treatment of choice?
A family of four presents with a burning sensation over the extremities. Some members also experience vomiting, diarrhea, dilated pupils, and occasional muscle spasms. What is the MOST likely cause of these symptoms?
A patient with a long history of depression on antidepressants presents with bradycardia, hypersalivation, and miosis after consuming an unknown substance. What is the most probable diagnosis?
Hemodialysis is used in the management of poisoning by all of the following agents except:
Which of the following drugs is most likely to result in addiction among those who have ever used it?
Practice by Chapter
General Principles of Toxicology
Practice Questions
Antidotes and Specific Therapies
Practice Questions
Drug Overdose Management
Practice Questions
Heavy Metal Poisoning
Practice Questions
Pesticide and Insecticide Poisoning
Practice Questions
Plant and Food Toxins
Practice Questions
Household Chemical Exposure
Practice Questions
Environmental Toxins
Practice Questions
Occupational Exposures
Practice Questions
Toxicological Screening and Diagnosis
Practice Questions
Extracorporeal Removal Techniques
Practice Questions
Poisoning Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
