Toxicology and Overdose Management — MCQs

On this page
All are true about aspirin poisoning except?
A 26-year-old female presents to the emergency department with a history of consuming hair dye containing paraphenylenediamine. What is the expected outcome in such a patient?
Acute liver failure is a clinical feature of which of the following?
An industrial worker was brought to a medical facility due to health problems. On his workup including laboratory tests, a finding of basophilic stippling of Red Blood Cells (RBC) was observed. Which among the following is he/she likely to be having?
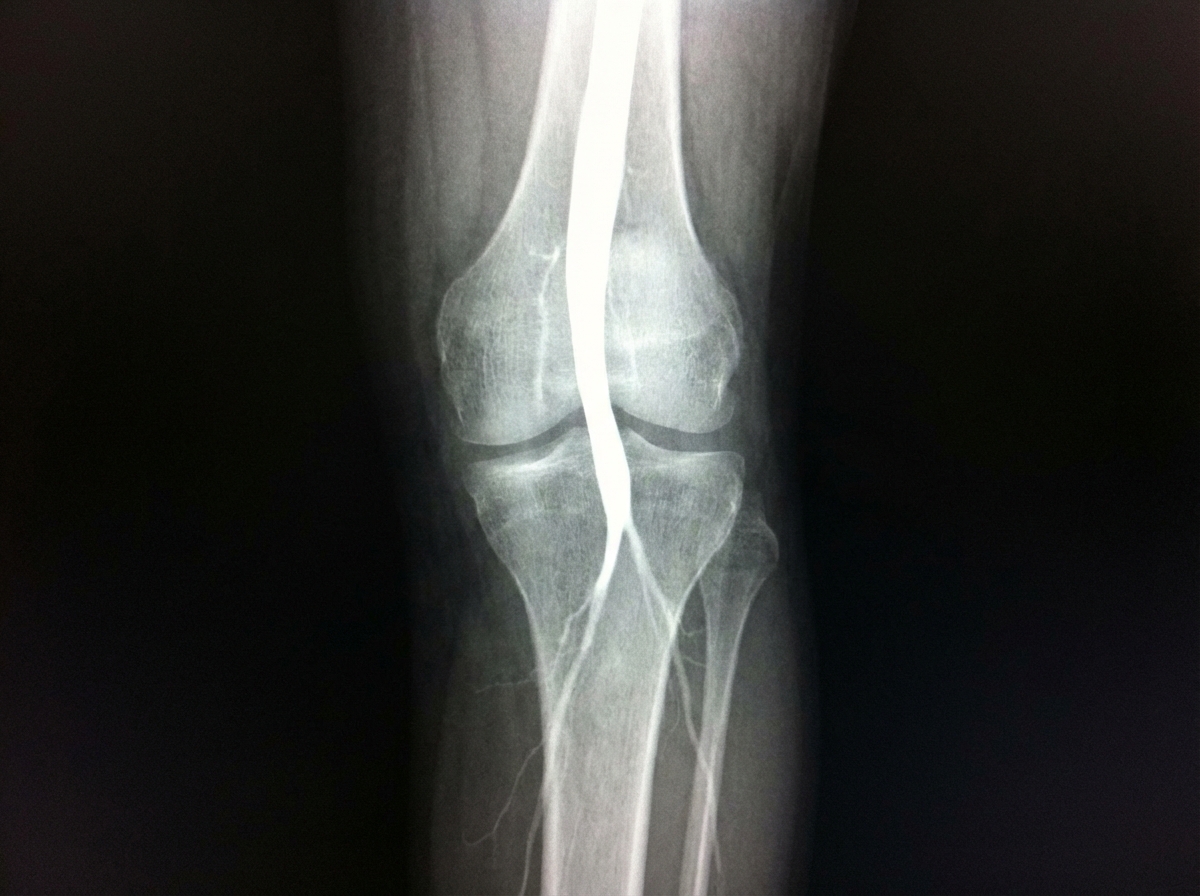
An HIV positive woman on ART was prescribed ergotamine for a migraine attack 4 days back. She presented with complaints that she is unable to feel her legs from the mid - thigh to her toes, for the past two days. The angiography image is given below. What is the likely diagnosis?
Gastric lavage is contraindicated in?
Gastric lavage is contraindicated in the following:
A farmer with pinpoint pupils, increased secretions and urination. What is the most likely diagnosis?
A 35-year-old construction worker presents with a 3-month history of abdominal pain, fatigue, and recent onset of numbness and tingling in his hands and feet. He works in renovation of old buildings. Physical examination reveals mild pallor and decreased sensation in a stocking-glove distribution. Blood tests show microcytic anemia with basophilic stippling on peripheral smear. What is the most likely diagnosis?
Miosis is caused by all EXCEPT -
Practice by Chapter
General Principles of Toxicology
Practice Questions
Antidotes and Specific Therapies
Practice Questions
Drug Overdose Management
Practice Questions
Heavy Metal Poisoning
Practice Questions
Pesticide and Insecticide Poisoning
Practice Questions
Plant and Food Toxins
Practice Questions
Household Chemical Exposure
Practice Questions
Environmental Toxins
Practice Questions
Occupational Exposures
Practice Questions
Toxicological Screening and Diagnosis
Practice Questions
Extracorporeal Removal Techniques
Practice Questions
Poisoning Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
