Rheumatology and Immunology — MCQs

On this page
A young man presents with chronic lower back pain and morning stiffness and pain on bending that improves with activity. X ray of LS spine is normal. Ocular examination shows anterior uveitis. Which diagnostic modality will pick up the disease process at the earliest?
A 20-year-old man presents with chronic back pain that is worse in the morning and improves with physical activity. He also has a history of anterior uveitis. A lumbar spine X-ray shows no abnormalities. Which of the following is the most appropriate next investigation for early diagnosis?
A 40-year-old man presents with discomfort in one of his joints. Synovial fluid aspiration reveals rhomboid-shaped, positively birefringent crystals under polarized light microscopy. Which of the following is the most likely diagnosis?
Which of the following is the most common clinical feature observed during the progression of systemic lupus erythematosus (SLE)?
Identify the following abnormality?
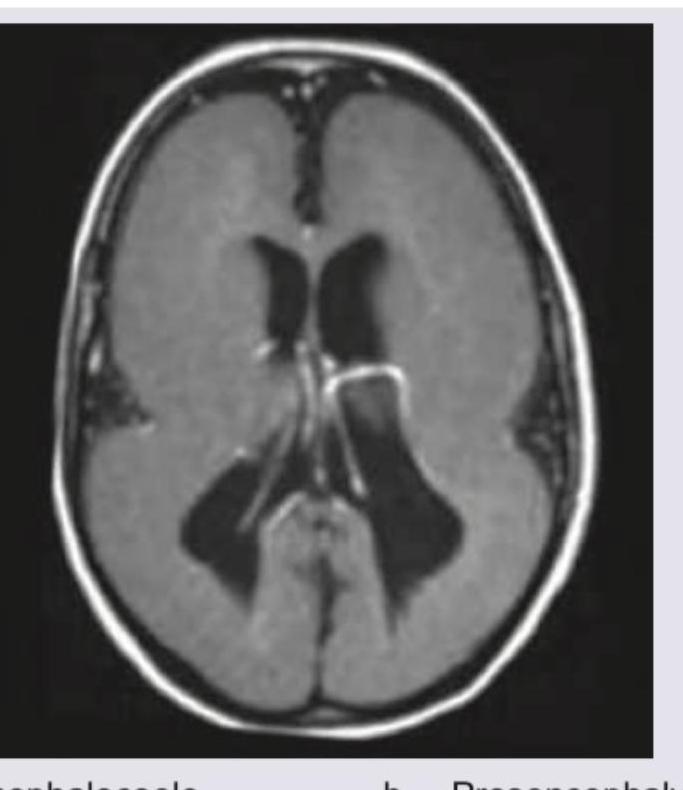
The clinical diagnosis favors development of chronic gout and the image shows presence of eccentric juxta-articular lobulated soft-tissue masses. Which of the following is the most definitive diagnostic test for gout shown in the image?
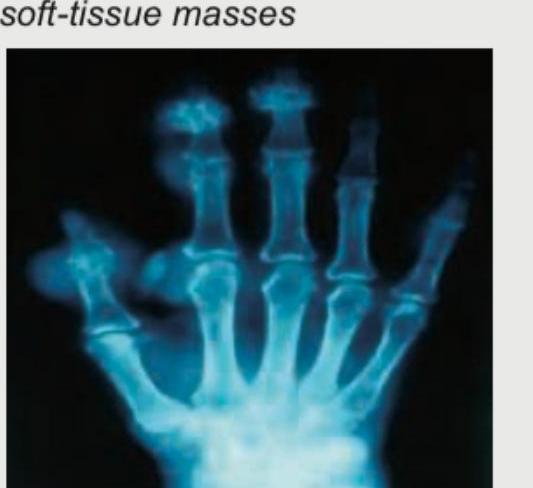
A 30-year-old female patient presents with erythematous rash over the neck, involving the back. Her investigations reveal presence of anti-MI-2 antibody. What is the diagnosis?
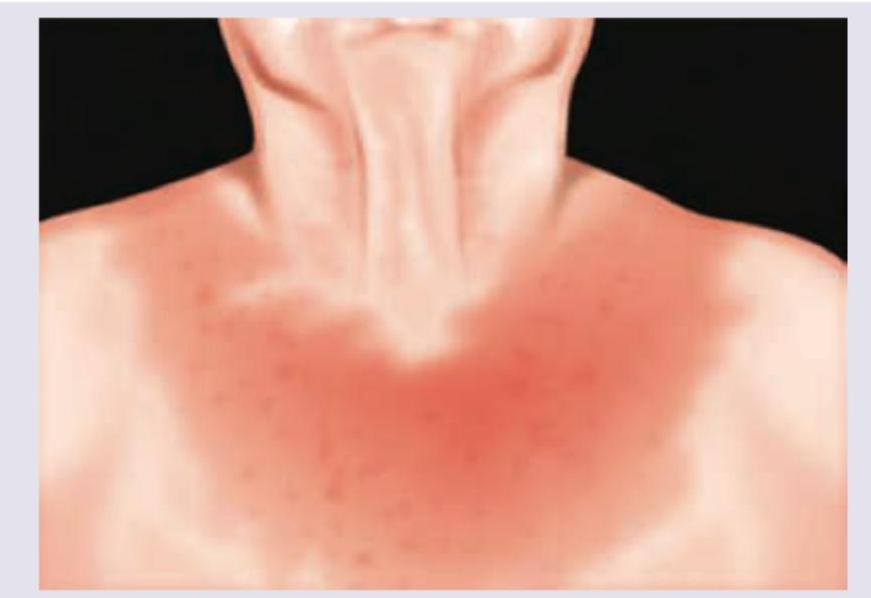
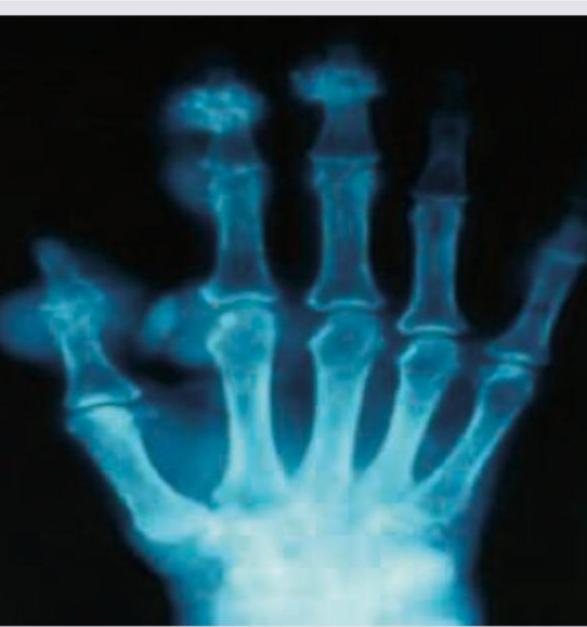
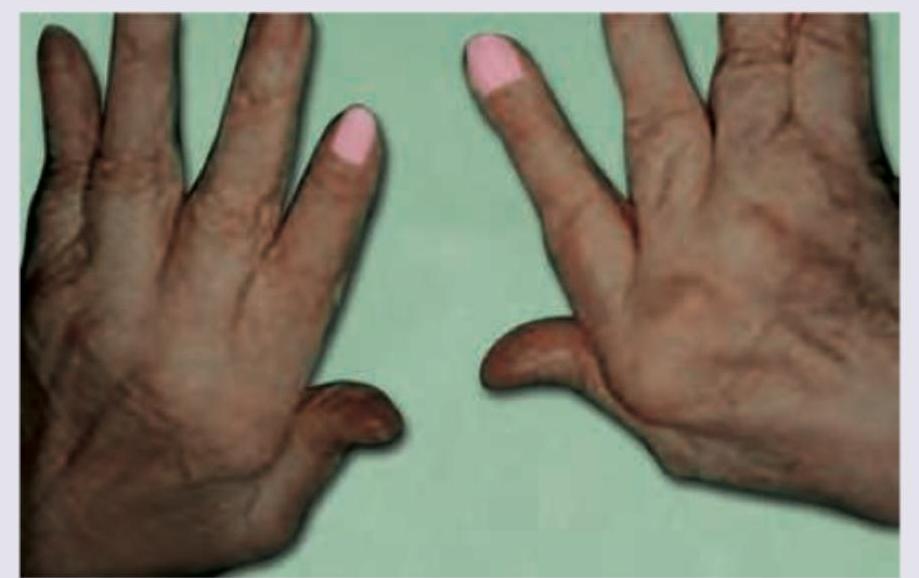
This elderly male came with a history of recurrent attacks of pain and swelling in the great toe in the past. This is the present X-ray of the hands. The diagnosis can be confirmed by:
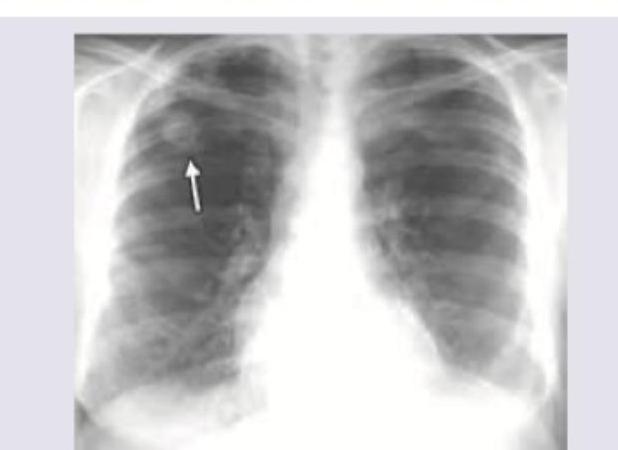
A 35-year-old crane operator at construction site with pre-existing seropositive rheumatoid arthritis complains of progressive difficulty in breathing. Chest X-ray was performed. What is the diagnosis?
A 55-year-old female on methotrexate presents with continuous pain and swelling of bilateral hand joints. What is the best treatment plan for this patient?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
