Rheumatology and Immunology — MCQs

On this page
Which of the following is NOT a feature of Ankylosing spondylitis (AS)?
A patient presents with melaena, normal renal function, hypertension, and mononeuritis multiplex. What is the most probable diagnosis?
Reactive arthritis is usually caused by which pathogen?
A patient with primary Sjogren syndrome treated with tear replacement for symptomatic relief notes continued parotid swelling for the last 3 months. She also has enlarged posterior cervical lymph nodes. Evaluation shows leukopenia and low C4 complement levels. What is the most likely diagnosis?
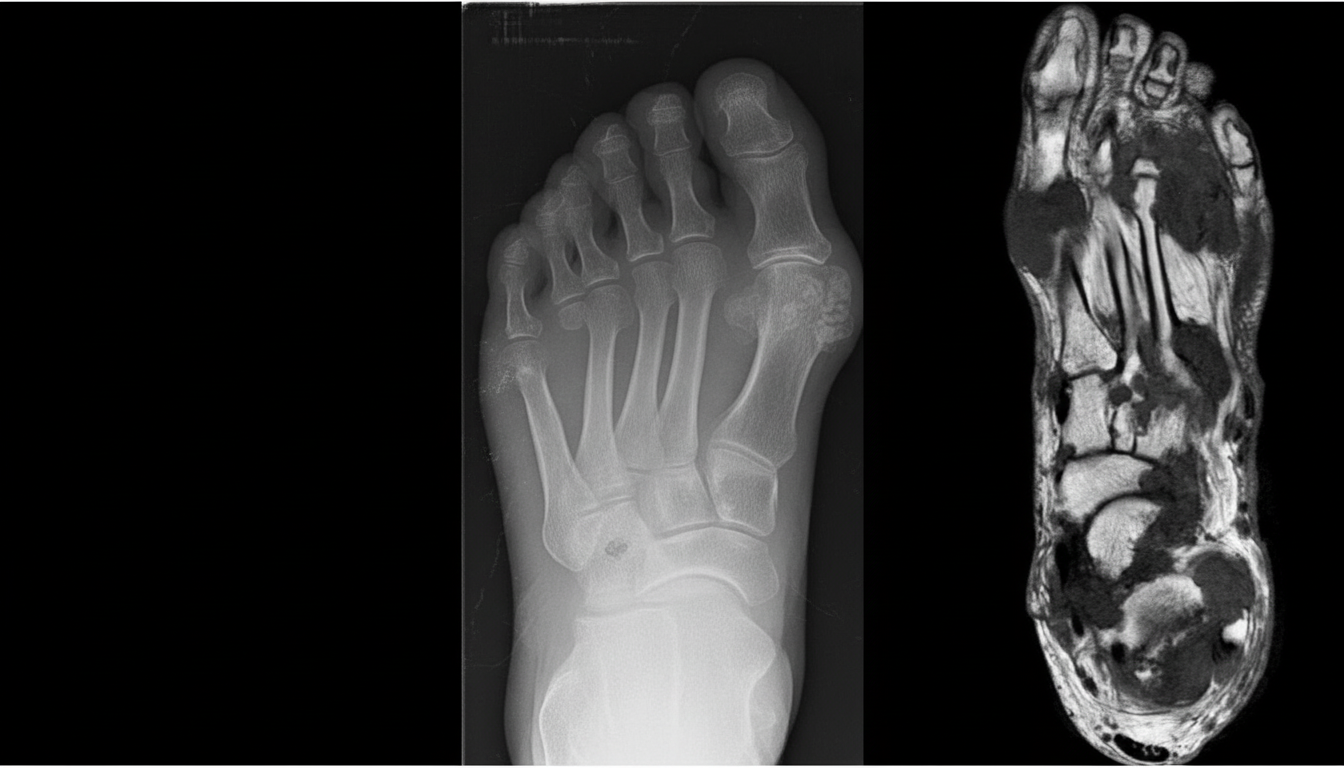
A person presented with swelling of the right 3rd toe. X-ray shows deposition of multiple crystals. A defect in which of the following pathways caused the problem?
A 25-year-old male presented to the OPD with a complaint of recurrent oral ulcers and congested eyes. On enquiry, he has a history of prior hospital admission for venous thrombosis. What is the condition he is suffering from?
Which of the following is FALSE about Sjögren's syndrome?
A 72-year-old man is newly diagnosed with bullous pemphigoid. Which of the following is the most appropriate next step in the management?
A patient presents with gritty pain in the eye and joint pain, following a recent urinary tract infection. What is the most probable diagnosis?
Which of the following is NOT an ANCA-associated vasculitis?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
