Rheumatology and Immunology — MCQs

On this page
Which of the following is true about Systemic Lupus Erythematosus (SLE)?
All of the following are increased in rheumatoid arthritis, except?
During the winter months, a 65-year-old man presents with livedo reticularis and purple fingertips. Other symptoms include arthralgia and weakness. Renal impairment is present on laboratory testing. Which of the following is the most likely diagnosis?
All of the following are true about Drug Induced Lupus, except?
Which of the following conditions does NOT typically cause bone erosion?
A 19-year-old man has a chronic papulosquamous skin disorder involving his knees and elbows. He now has dull low back pain and morning stiffness that lasts a few hours. On examination, forward flexion at the lumbar spine is reduced, but neck movements are normal. There is stress tenderness of both sacroiliac joints. Which of the following is the most likely diagnosis?
In giant cell arteritis, which of the following is true?
A 25-year-old normotensive patient presents to the emergency department with breathlessness and palpitations. The patient has a history of allergy to peanuts and accidentally ingested them. On examination, the patient's heart rate is 120/min and blood pressure is 100/60 mm Hg. An urgent X-ray was performed. What is the most likely diagnosis?
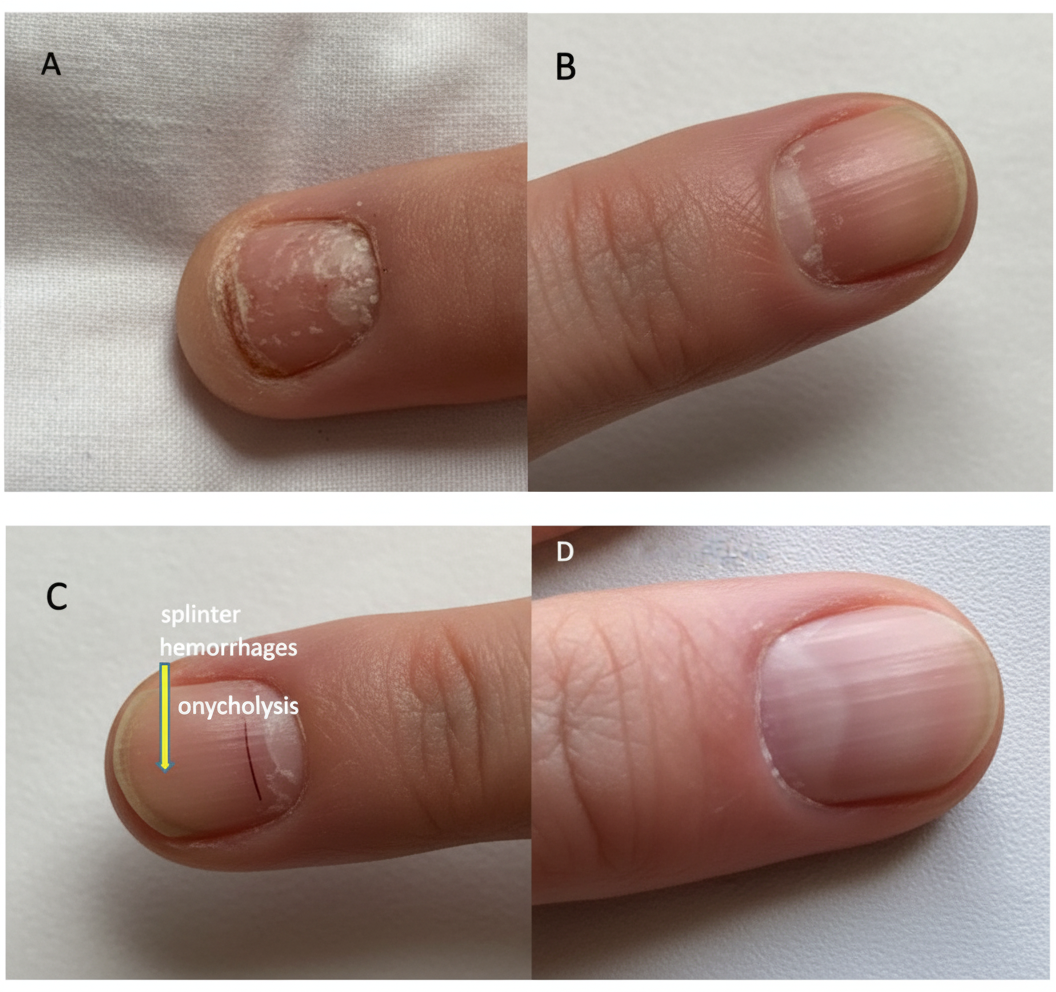
This lesion is most commonly seen in which disease?
What is the first-choice disease-modifying antirheumatic drug (DMARD) in rheumatoid arthritis?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
