Rheumatology and Immunology — MCQs

On this page
Which of the following features of rheumatic fever is not due to molecular mimicry?
Rheumatoid factor in rheumatoid arthritis is important because:
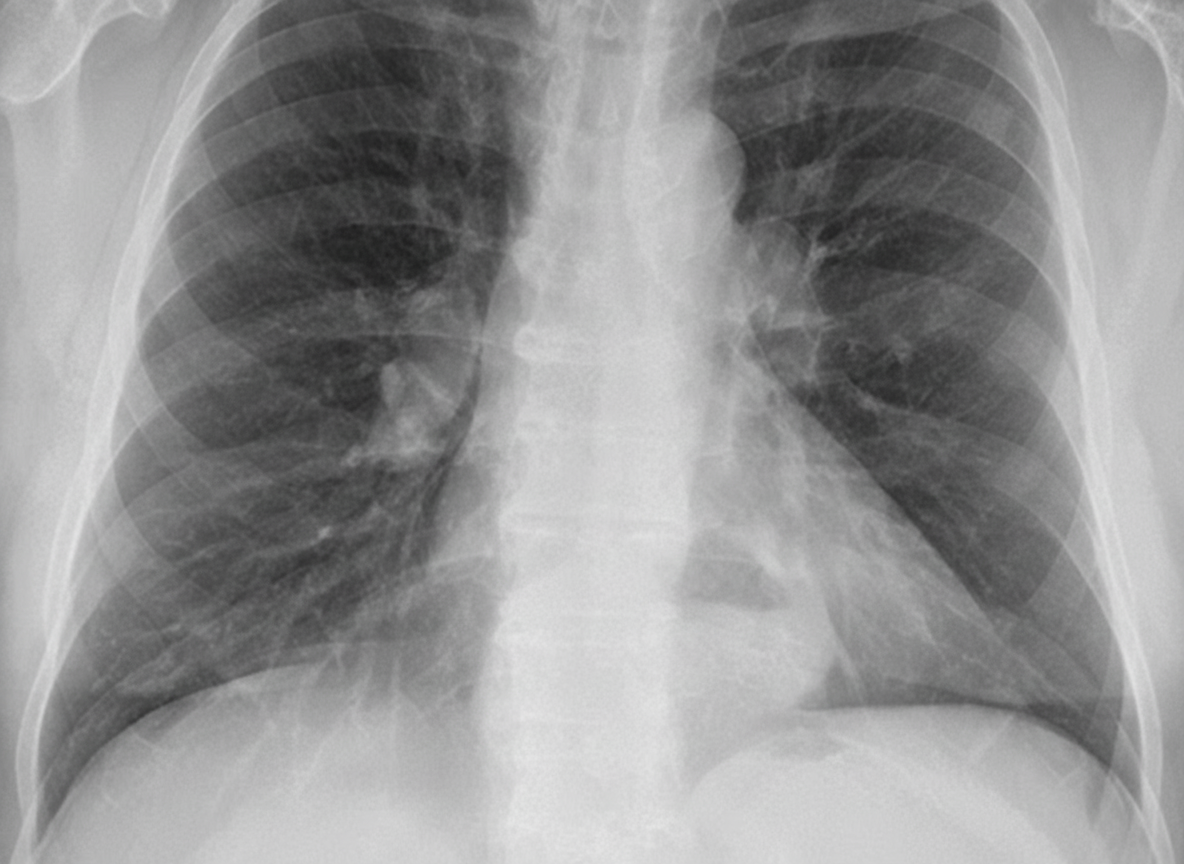
A 64-year-old woman with a longstanding diagnosis of mixed connective tissue disorder and pulmonary fibrosis is admitted with symptoms of recent increase in postprandrial retrosternal distress, heartburn, and nocturnal cough. Her ECG shows nonspecific T-wave changes and she finds minimal relief of her symptoms with sublingual NTG. On examination, she is not in any acute distress and is afebrile. Chest exam reveals bilateral crackles. CXR is shown. What is the most likely cause of this patient's acute symptoms?
Temporal arteritis is associated with all of the following except?
A 43-year-old woman presents with a year of progressive dysphagia. She notes that her hands turn white and become painful upon exposure to cold. She also observes that her face and hands lack wrinkles, despite her age. Physical examination reveals a blood pressure of 115/75 mm Hg and taut, shiny skin on her face and hands. A punch biopsy of the hand skin shows dermal collagenous fibrosis and focal calcification. She undergoes yearly esophageal dilation for 20 years, with no serious illnesses developing during this period. Which of the following serologic test results is most likely to be positive in this woman?
What is the mechanism of acute rheumatic fever?
A 36-year-old woman presents with increased trouble swallowing. Physical examination finds hypertension and sclerodactyly. Lab tests find Anti-Scl-70 antibodies. Which of the following biopsies is most characteristic of this disorder?
What is the drug of choice for an acute attack of hereditary angioneurotic edema?
A 45-year-old woman presents with pain in her fingers upon cold exposure, arthralgias, and dysphagia for solids. She has a few telangiectasias over the chest but no facial erythema or erythema of extensor surfaces. Physical examination reveals slight skin thickening of the hands, arms, and torso. What is the most appropriate diagnostic workup?
What is a cause of nail bed infarctions?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
