Rheumatology and Immunology — MCQs

On this page
A 30-year-old male presents with numbness of both lower limbs and right upper limb. Examination reveals pulse 88/min and BP 160/110 mmHg. He also has digital gangrene involving the right 2nd and 3rd fingers. Urine routine examination is unremarkable. Microscopic examination shows RBCs. Hemogram and serum biochemistry are within normal limits. What is the most probable diagnosis?
Which of the following is NOT a small vessel vasculitis?
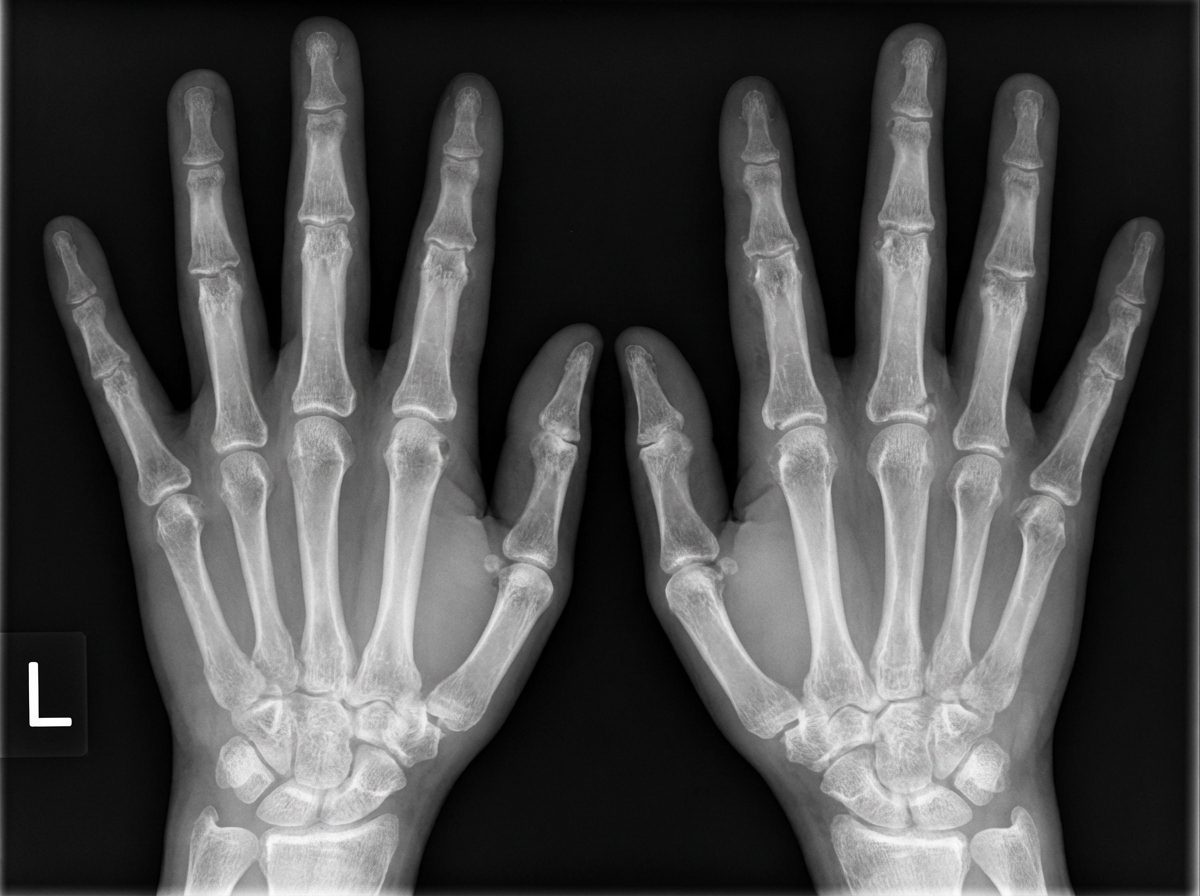
A 40-year-old female presents with a history of fever, weight loss, and polyarthralgia. Given the radiological findings, what is the most likely diagnosis?
Strawberry gingivitis is classically seen in which of the following conditions?
Pseudolymphoma is a known association with which of the following conditions?
In idiopathic polymyositis, which of the following is typically NOT seen?
The most common pulmonary manifestation of Systemic Lupus Erythematosus (SLE) is:
What tests should be performed before initiating infliximab therapy in a 60-year-old female patient with rheumatoid arthritis?
Myopathy is seen in all except?
A 65-year-old male develops sudden onset of severe knee pain, redness, swelling, and tenderness. He has a history of diabetes mellitus and cardiomyopathy. An X-ray of the knee shows linear calcification. Which of the following investigations is best for making a definitive diagnosis?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
