Rheumatology and Immunology — MCQs

On this page
What is the treatment for the lesions seen in Behcet syndrome?
Multiple cavitary lesions in the lungs, hematuria, and renal insufficiency are features in a patient with:
Extreme widening of the periodontal ligament space on dental radiograph is the characteristic feature of which condition?
A 72-year-old man injures his right knee, which is now swollen and extremely painful to bend. X-rays of the knee rule out a fracture, and joint fluid aspiration reveals an opaque-colored fluid containing rhomboid crystals with weak-positive birefringence. Which of the following is the most appropriate next step in management?
Which condition is associated with Coombs positive hemolytic anemia?
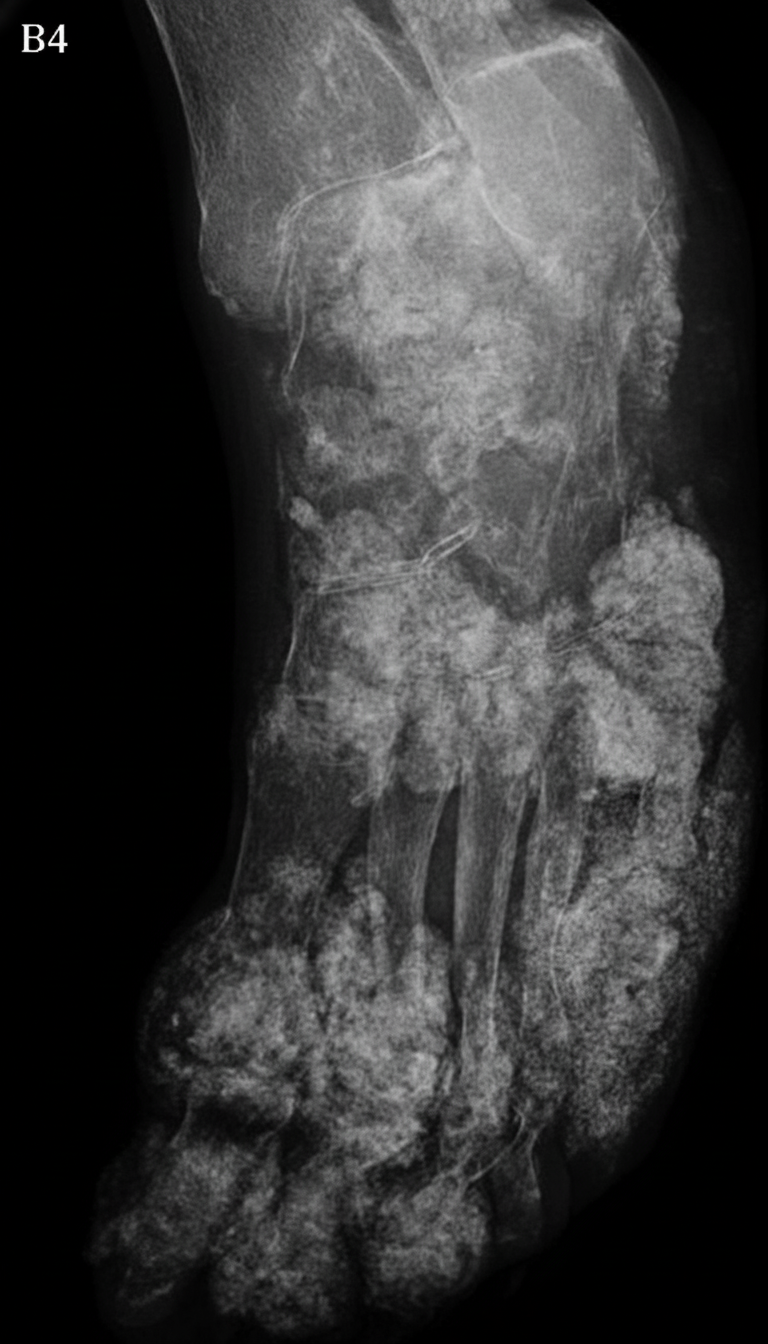
What is the most likely diagnosis of this case?
A 57-year-old man, previously asymptomatic and on no medications, develops a painful left big toe. It is so painful that even the weight of his sheets is excruciating. On examination, there is a swollen red toe. Which of the following medications is relatively contraindicated?
Which of the following statements is FALSE regarding HIV-related arthritis?
Which one of the following disorders is not associated with carpal tunnel syndrome?
Which of the following conditions is characterized by non-deforming arthritis?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
