Rheumatology and Immunology — MCQs

On this page
A 50-year-old man presents with a month of muscle pain and fever, noting darker colored urine for the past two weeks. Physical examination reveals palpable purpuric skin lesions. Urinalysis shows hematuria and proteinuria. Serum laboratory findings include mixed cryoglobulinemia with a polyclonal increase in IgG, and a high titer of antimyeloperoxidase (MPO-ANCA), also known as P-ANCA. A skin biopsy is performed. What pathologic finding is most likely to be observed in this biopsy?
Which condition characteristically involves the lungs?
Which of the following joint findings is most suggestive of an inflammatory cause of joint pain, rather than osteoarthritis?
ASO titre is diagnostic in?
A young male presents with painful ulcers on the mouth and glans penis, blurred vision, and a history of recurrent epididymitis. What is the most probable diagnosis?
DNA topoisomerase 1 autoantibody is specific for which condition?
All of the following are true about Raynaud's disease except?
Gout can be precipitated by all of the following EXCEPT?
A 22-year-old man presents with low back pain and stiffness, which have progressively worsened over several months. He also reports nocturnal stiffness and hip pain. Physical examination reveals paravertebral muscle tenderness and limited lumbar spine flexion. Radiographic findings of the lumbar spine are shown. What is the most likely diagnosis?
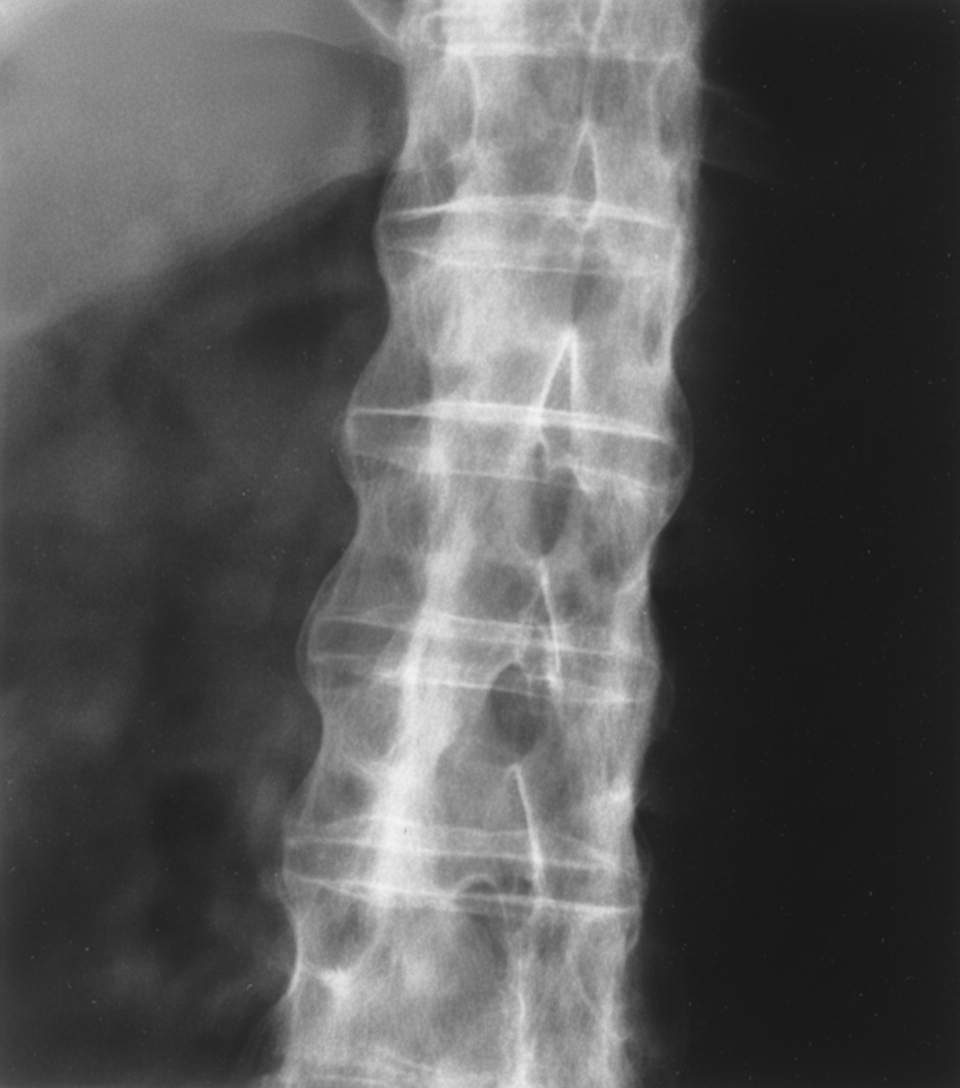
Ankylosing spondylitis may be associated with which of the following conditions?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
