Rheumatology and Immunology — MCQs

On this page
A 37-year-old woman presents with complaints of severe heartburn with or without meals. She has a history of hypertension, which has been treated with captopril. She also has a history of Raynaud disease, multiple facial telangiectasias, and very taut skin on the dorsum of both hands. She has failed to obtain relief for her heartburn with large doses of antacids or omeprazole. Esophageal manometry is ordered. What are the most likely results of this test?
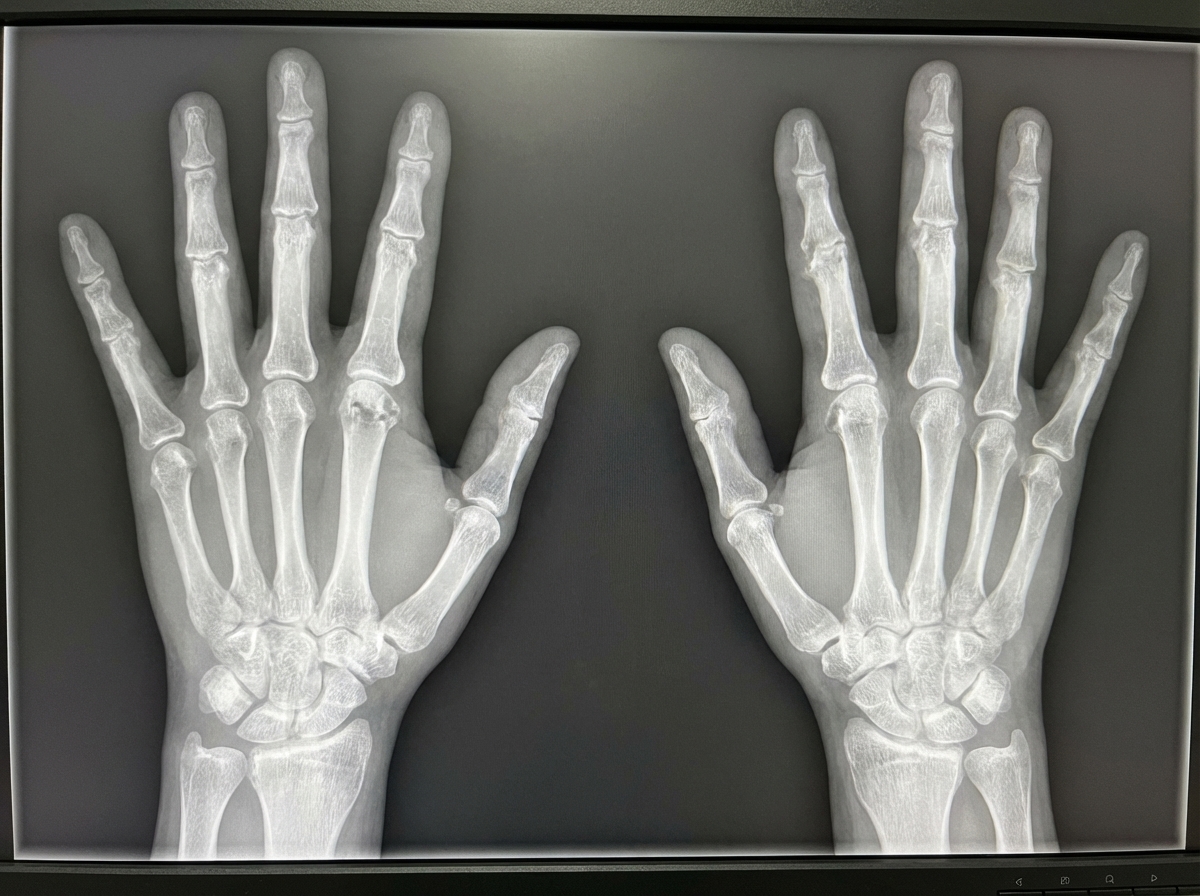
A patient suffering from morning stiffness lasting more than 1 hour presents with the following abnormality in the X-ray. What is the most possible diagnosis?
All of the following is true about Felty syndrome, except?
Felty's syndrome is associated with which of the following conditions?
Which of the following organs is least likely to be involved in Behcet's disease?
Which of the following is FALSE regarding antiphospholipid antibody syndrome (APLA)?
Reactive arthritis is associated with which of the following pathogens?
Which test evaluates lacrimal gland function for the diagnosis of Sjogren syndrome?
A man developed frequent facial swelling with occasional laryngeal edema. What is the most probable diagnosis?
Felty's syndrome is associated with which of the following?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
