Rheumatology and Immunology — MCQs

On this page
All of the following are true about temporal arteritis except?
Diffuse cutaneous systemic sclerosis is characterized by which of the following?
Perioral and periorbital skin lesions are seen in which condition?
This type of lesion is most commonly seen in which disease?
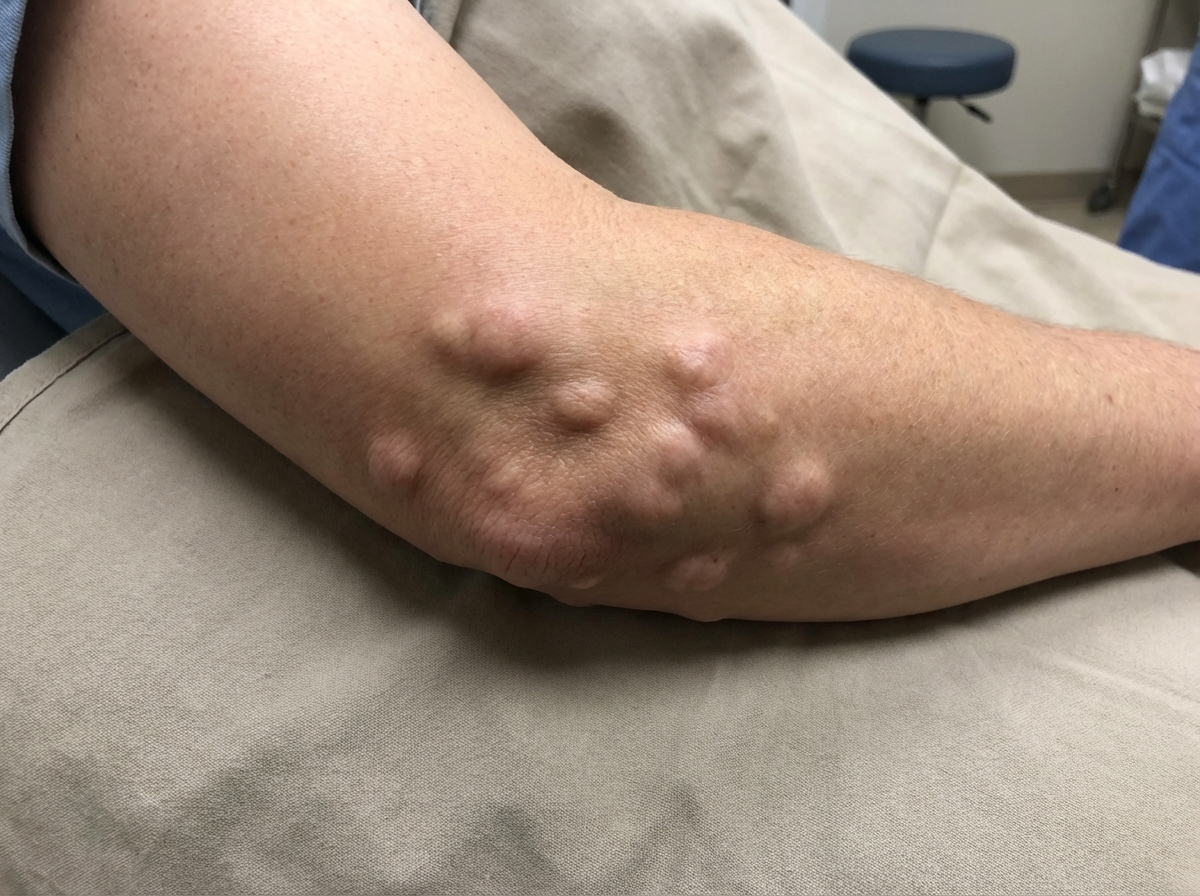
Groton's sign is seen in which of the following conditions?
A 33-year-old woman has experienced episodes of fatigue, pleural effusion, pericardial effusion, carpal tunnel syndrome, and macrocytic anemia. What is the best test for diagnosis?
A 25-year-old woman presents with concerns about systemic lupus erythematosus, citing intermittent oral ulcers and right knee pain. She has no significant past medical history and uses only occasional ibuprofen. Physical examination reveals no alopecia, skin rash, or joint swelling. Her blood work shows a positive ANA at a titer of 1:40, with no other abnormalities. Which of the following statements is true?
Which of the following is a feature of osteoarthritis?
SS-A (Ro) and SS-B (La) antibodies found in Sjogren syndrome are targeted against which cellular component?
Which of the following statements regarding an acute attack of gouty arthritis is EXCEPT?
Practice by Chapter
Rheumatoid Arthritis
Practice Questions
Spondyloarthropathies
Practice Questions
Systemic Lupus Erythematosus
Practice Questions
Vasculitis Syndromes
Practice Questions
Scleroderma and Related Disorders
Practice Questions
Inflammatory Myopathies
Practice Questions
Crystal Arthropathies
Practice Questions
Osteoarthritis
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Autoinflammatory Syndromes
Practice Questions
Sjögren's Syndrome
Practice Questions
Antiphospholipid Syndrome
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
