Pulmonology — MCQs

On this page
A 25-year-old male smoker presents with high-grade fever, chills, severe right-sided pleuritic chest pain, and cough with expectoration. Physical examination of the patient is likely to show which of the following?
Residual lung volume is increased in which of the following conditions?
Foreign body aspirated during dental procedures can be retrieved by?
Type II Respiratory failure is characterized by?
Type II respiratory failure best relates to which of the following?
What is the most likely diagnosis?
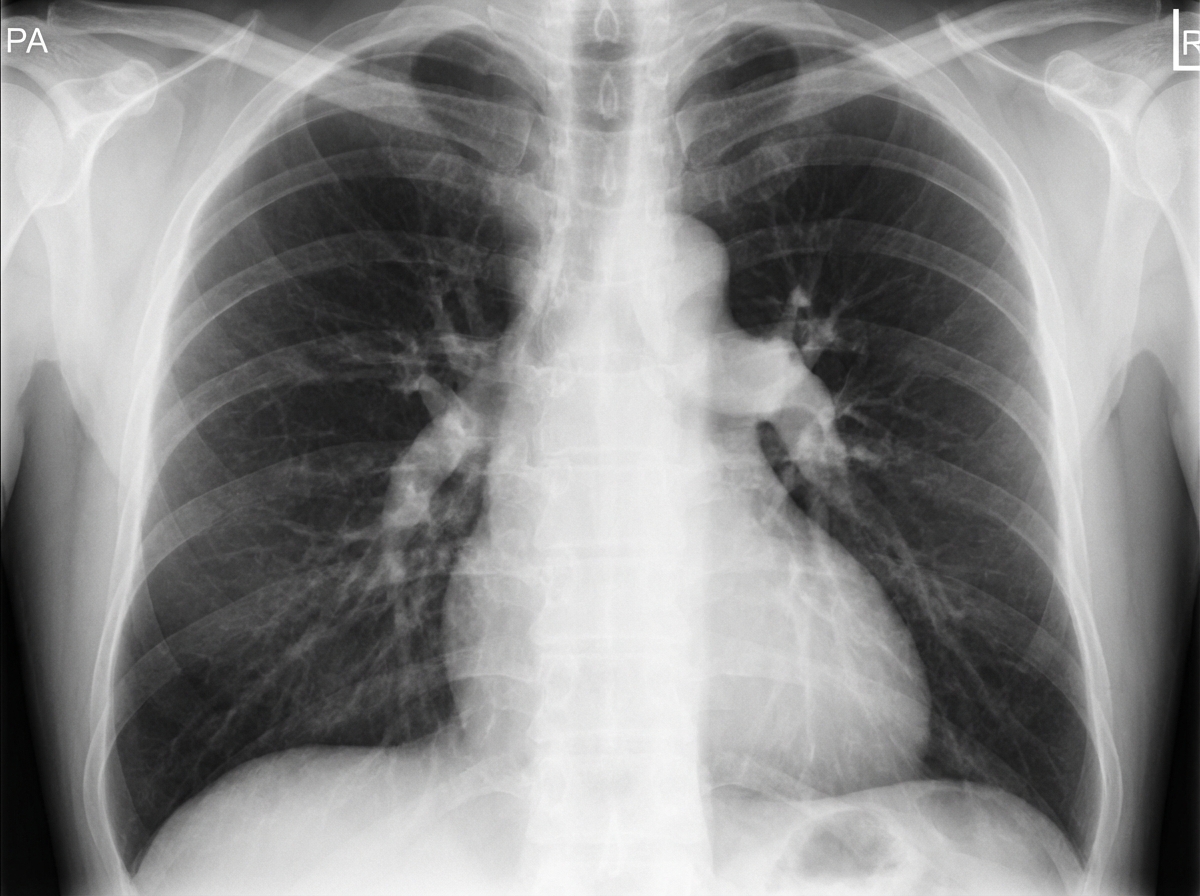
Lower lobe fibrosis is typically seen in which of the following conditions?
In ARDS, all are seen except:
A chest X-ray shows a homogenous opacity on the right side with shifting of the mediastinum to the opposite side. What is the most probable diagnosis?
Which of the following is not a feature of consolidation?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
