Pulmonology — MCQs

On this page
Which of the following is NOT a sign of advanced COPD?
The CURB-65 criteria for assessing the severity of pneumonia includes all of the following EXCEPT:
The CURB-65 criteria for assessing the severity of pneumonia includes all of the following EXCEPT:
A 72-year-old man with COPD develops acute shortness of breath and presents to the hospital. He appears uncomfortable; blood pressure is 120/90 mm Hg, pulse 100/min, oxygen saturation 85% on room air. On examination of the chest, there is absent fremitus, absent breath sounds, and hyper resonant percussion of the right lung. The trachea is shifted to the left. For the above patient with abnormal pulmonary physical findings, what is the most likely diagnosis?
Which of the following is NOT a feature of pneumothorax?
Peripheral eosinophilia is not a characteristic feature of which of the following conditions?
What is the minimum concentration of reduced hemoglobin required for cyanosis?
Which of the following is NOT included in the CURB-65 criteria for community-acquired pneumonia?
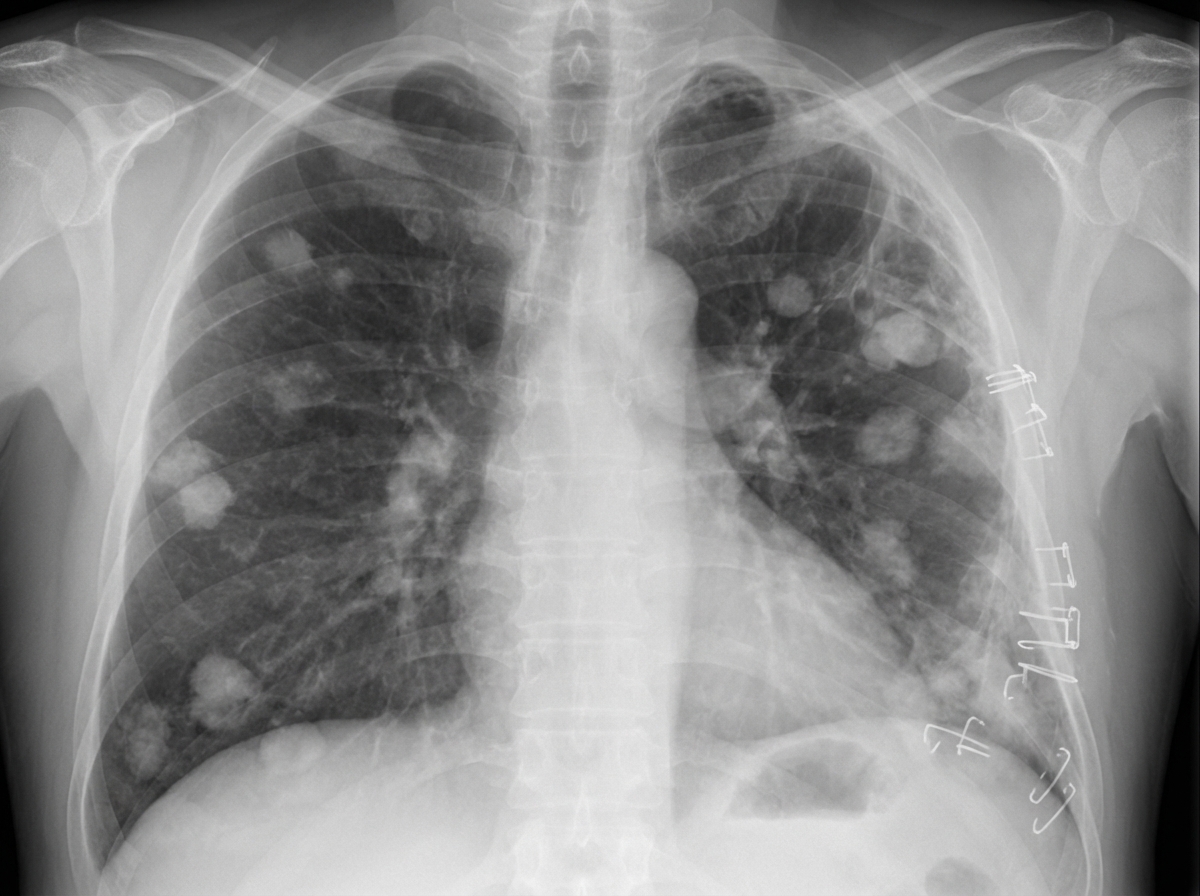
A 70-year-old man with a history of emphysema and progressive dyspnea is admitted with mild hemoptysis. On examination, he is afebrile; he has a left-sided chest wall scar from a previous thoracotomy with decreased breath sounds in the left lung field. There are wheezes and rhonchi heard in the right lung field. Based on the clinical history and the CXR shown, what is the most likely diagnosis?
Which of the following findings is NOT seen in primary pulmonary hypertension?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
