Pulmonology — MCQs

On this page
Which of the following is NOT caused by sarcoidosis?
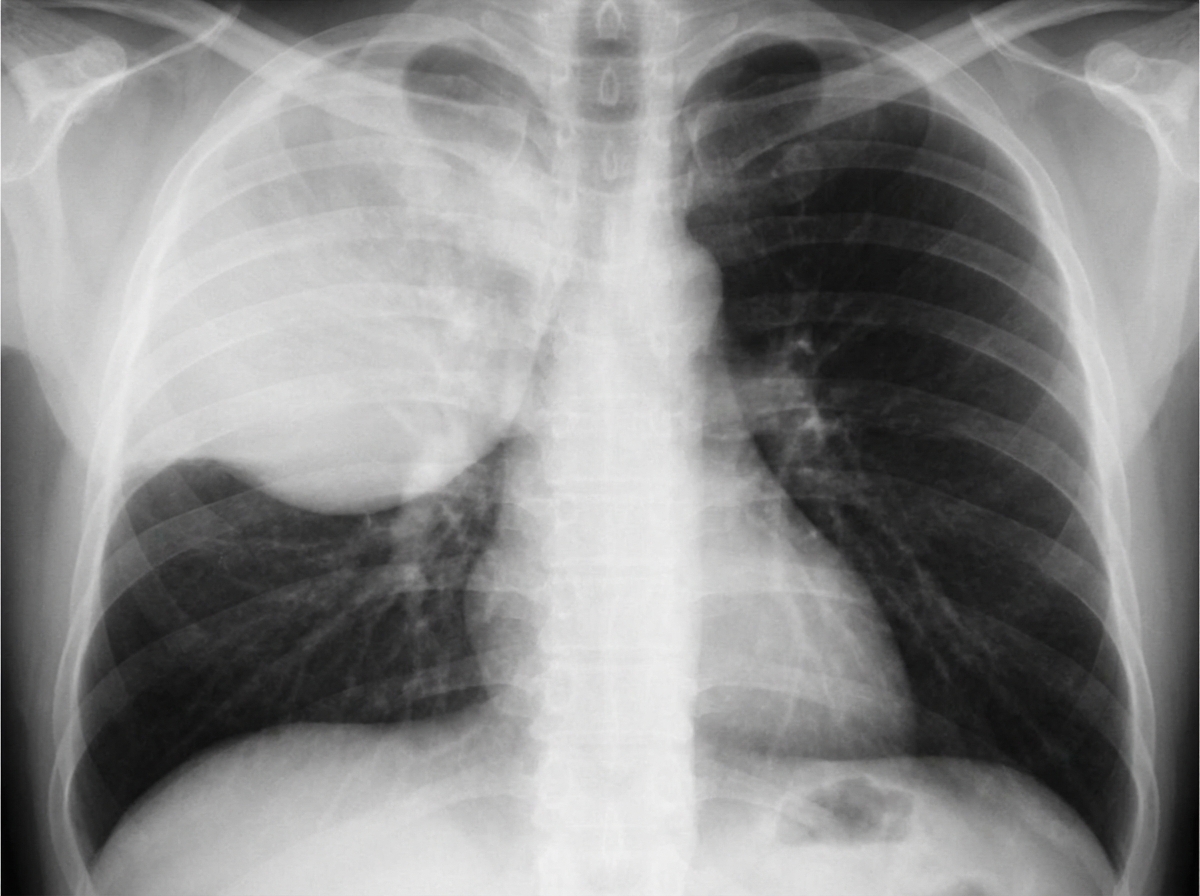
A 34-year-old woman is admitted with a history of fever, chills, and greenish sputum for 10 days. She has a history of alcohol and substance abuse. On physical examination, vital signs are: pulse 113 bpm; temperature 101degF; respirations 25/min; blood pressure 110/78 mm Hg. She appears ill and has crackles with egophony and E to A changes in the right upper lung field. Laboratory data: Hb 12 g/dL; Hct 37%; WBCs 15.0/uL; differential BUN 48 mg/dL; creatinine 1.7 mg/dL. Chest radiographs are shown. What is the most likely diagnosis?
The absence of which of the following signs or symptoms makes a diagnosis of pulmonary embolism unlikely?
Although asthma is a heterogeneous disease, which of the following is most likely to be present in all individuals with asthma?
Which of the following are true about Kartagener's syndrome?
All of the following are true about emphysema except:
A 50-year-old male presents with dyspnea, dry cough, fatigue, and anorexia. Investigations reveal a raised ESR and a restrictive pattern in pulmonary function tests. HRCT shows honeycombing in subpleural and basal locations. What is the probable diagnosis?
What is the typical feature of interstitial lung disease?
Which of the following patient groups is NOT at increased risk for pneumococcal pneumonia?
Which organ's primary involvement is not reported to be affected by sarcoidosis?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
