Pulmonology — MCQs

On this page
Adult respiratory distress syndrome is defined by all except:
Bronchiectasis is most common in which lobe?
A 27-year-old man presents with new left-sided chest pain and feeling unwell. He describes a 2-day history of cough with some blood-tinged sputum, fever, and chills. His past medical history is negative, and he smokes about 1 pack of cigarettes per day. On physical examination, there is dullness and crackles in the left lower chest. Which of the following is the most likely diagnosis?
What is the gold standard for diagnosing pulmonary embolism?
Which one of the following distinguishes ARDS (acute respiratory distress syndrome) from cardiogenic pulmonary edema?
All the following conditions cause type I respiratory failure EXCEPT?
A 26-year-old male presents with a history suggestive of tuberculosis and pleural effusion on examination. Which of the following parameters is NOT used for the analysis of pleural fluid in this context?
Which viral infection is associated with exacerbation of asthma in COPD patients?
Velcro crackles are heard in which condition?
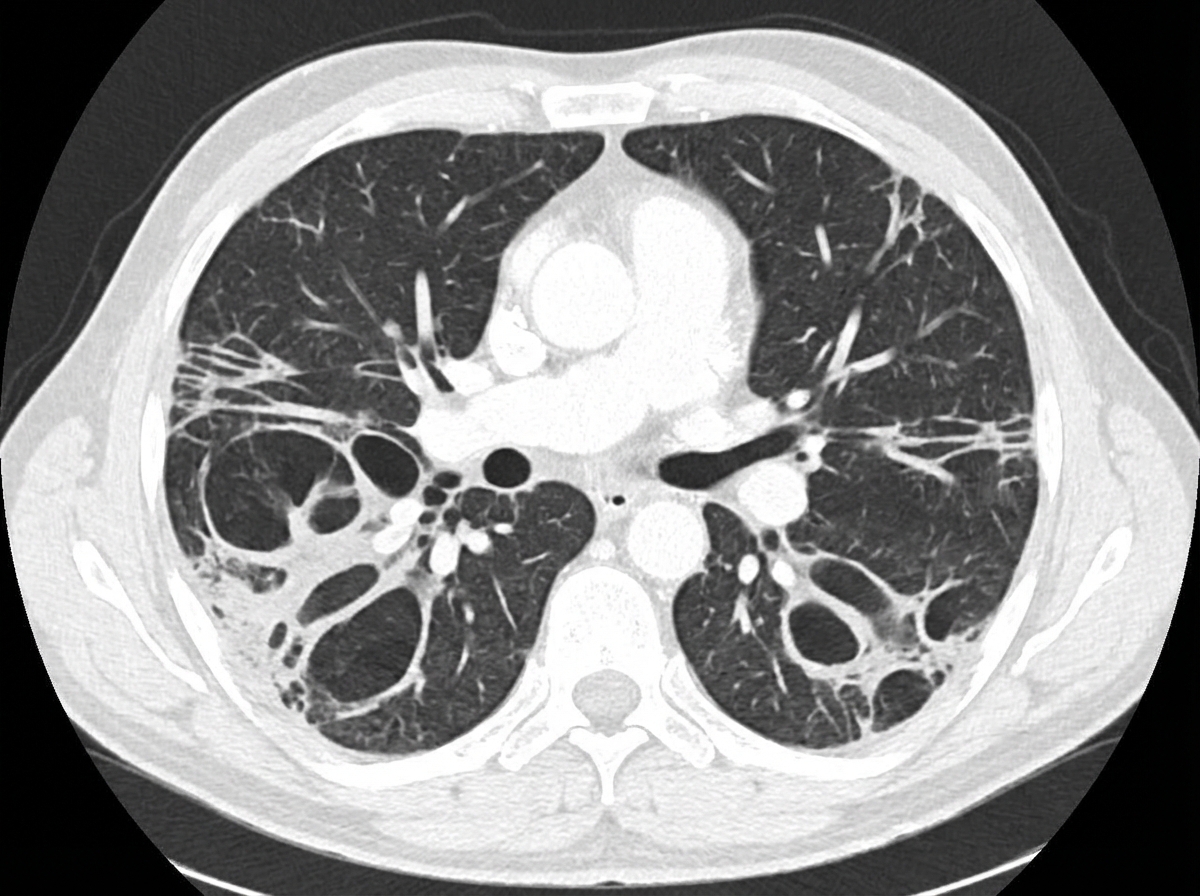
A 55-year-old non-smoker lady presented with on and off haemoptysis and productive cough for 1 year. There was no fever or constitutional symptoms. Physical examination showed clubbing of fingers and coarse crepitations over the lung base. Blood tests were essentially normal and an initial CXR and CT scan were performed. What is the radiological diagnosis?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
