Pulmonology — MCQs

On this page
Which of the following conditions is most sensitively detected by D-dimer testing?
What is the drug of choice in interstitial lung disease?
A 28-year-old bank employee presents with infertility and oligospermia. He reports a history of recurrent pancreatitis and chronic cough since childhood, with evident digital clubbing. Which test is most likely to reveal the cause of his chronic lung disease?
Dyspnoea at rest is which grade?
Which of the following statements regarding Sarcoidosis is correct?
A 60-year-old man with a past history of smoking for 30 years (he stopped 3 years ago, prior to cardiac bypass surgery) is admitted with cough and mild hemoptysis. He is afebrile with no shortness of breath. Physical exam is negative except for rhonchi in the left upper lung zone on auscultation. What is the finding or abnormality most likely to occur with the lesion seen on the chest X-ray?
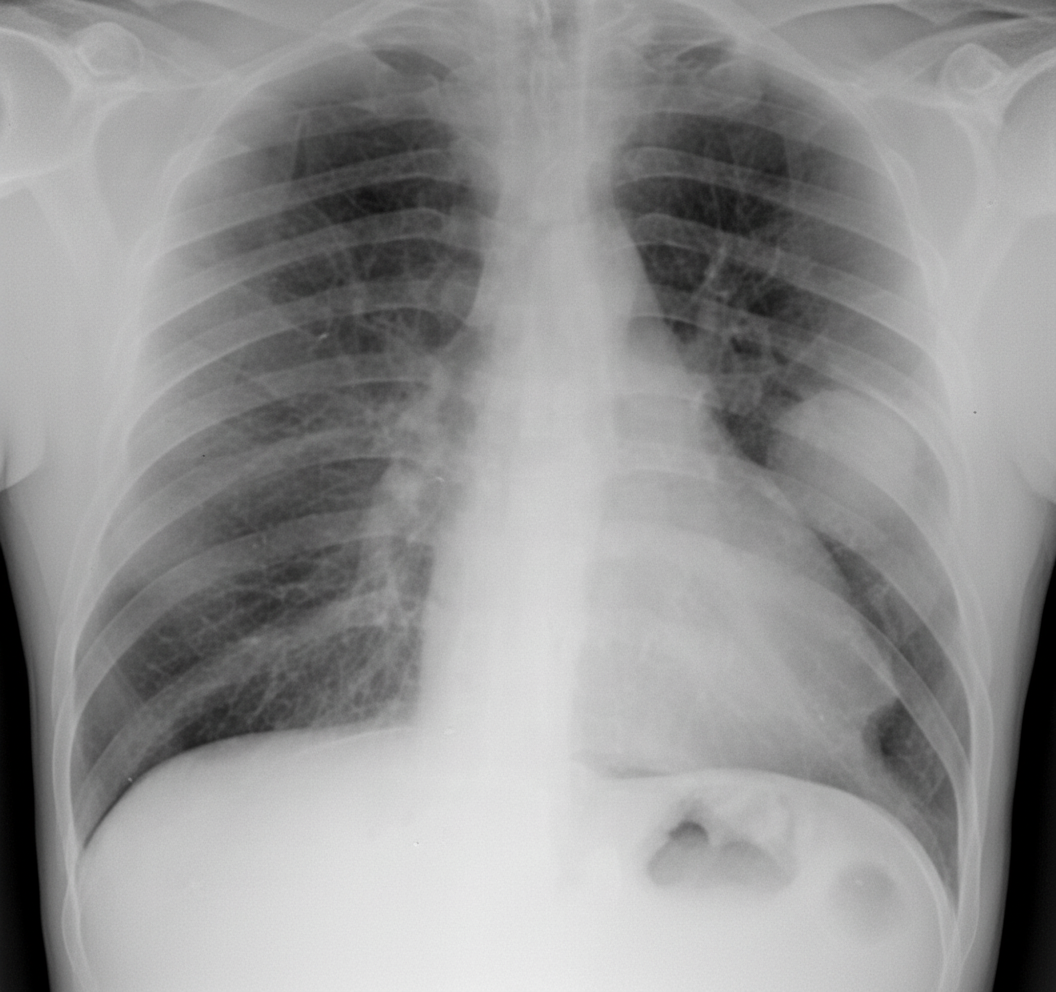
Which of the following conditions typically presents with an exudative pleural effusion?
A 52-year-old man presents with a chronic cough and shortness of breath. He admits to smoking two packs of cigarettes a day for 30 years and has been diagnosed with chronic obstructive pulmonary disease. In counseling this patient, you advise him to stop smoking immediately and inform him that, in addition to emphysema, which of the following organs carries a significantly increased risk of smoking-related cancer?
Which of the following is NOT a common cause of acute exacerbation of COPD?
What is the most common cause of unilateral diaphragmatic paralysis?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
