Pulmonology — MCQs

On this page
Which of the following conditions can present with miliary mottling?
Which of the following routes of infection is most responsible for lung abscess?
Which of the following statements is true regarding pulmonary arterial hypertension (PAH)?
Which of the following is FALSE regarding Allergic bronchopulmonary aspergillosis?
Brock's Syndrome is associated with which of the following conditions?
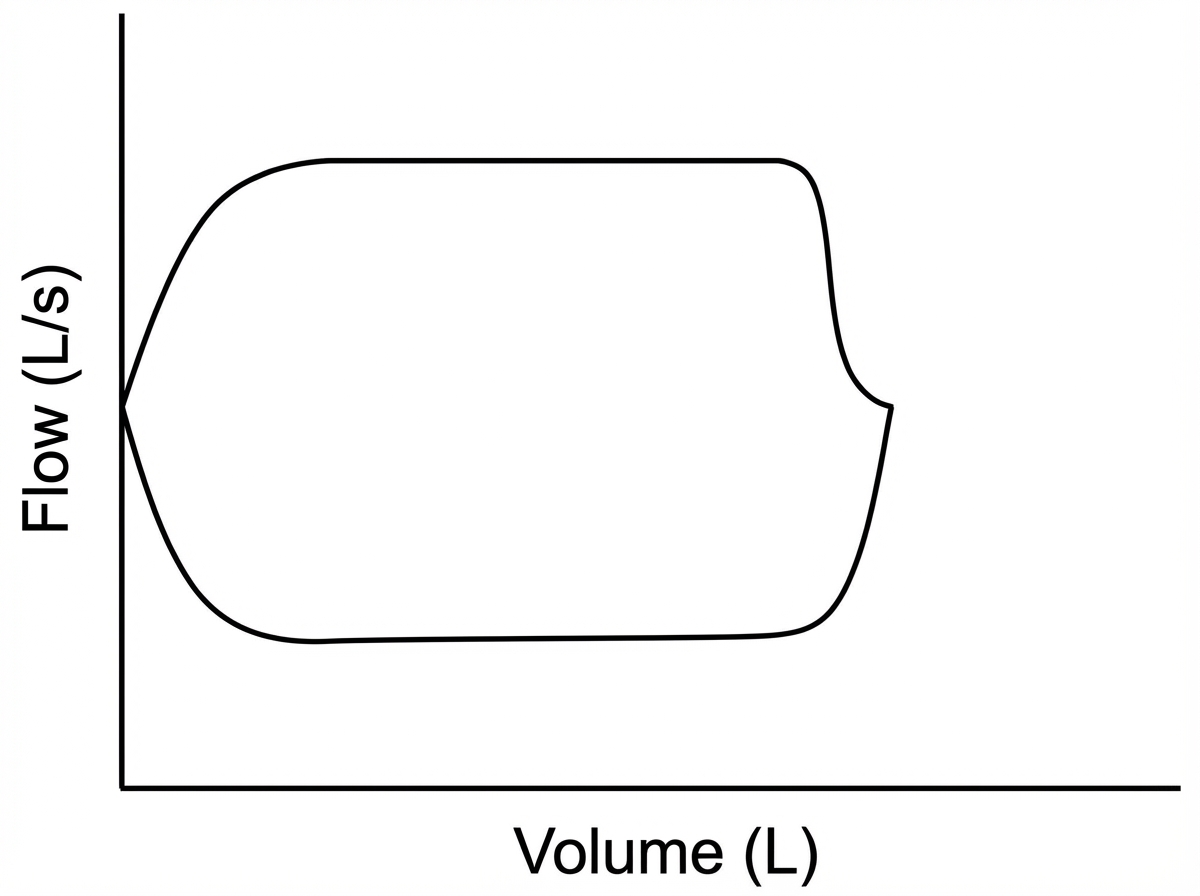
A 65-year-old male presented with progressive dyspnea on exertion for 3 months. His past medical history includes necrotizing pancreatitis and ARDS, for which he was mechanically ventilated. He is a chronic smoker. On examination, low-pitched inspiratory and expiratory wheezes are heard over the mid-chest area. Pulmonary function tests revealed an FEV1 of 78% of predicted and an FEV1/FVC ratio of 60%. A flow-volume curve was also obtained. What is the most likely diagnosis in this case?
A 28-year-old woman complains of chest pain for 1.5 months. Three months prior to the current visit, she developed a cough with expectoration, worse in the early morning. There was no shortness of breath or hemoptysis. About 2 months after the onset of the cough, she began to have intermittent pleuritic chest pain, increasing fatigue, and weight loss of 3 kgs but no loss of appetite. On auscultation, fine crackles in the suprascapular areas bilaterally were present (left greater than right). The left upper lobe was dull to percussion. Which of the following is NOT a component of the classic medium used for the diagnosis of the likely disease?
Which of the following is NOT associated with Loeffler's syndrome?
A 27-year-old man with a history of chronic sinus and pulmonary infections presents for evaluation. He works as a salesperson and denies specific occupational exposure. He is married and has no children. Family and travel history are noncontributory. Examination reveals crackles in both lower lung zones and extremities show no clubbing. Chest X-ray shows the cardiac apex displaced to the right side of the chest with the gastric bubble also noted on the right. What is the most likely diagnosis?
Empyema necessitans is defined as when?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
