Pulmonology — MCQs

On this page
A 40-year-old woman presents with fever and cough for several days, producing green-colored sputum. She has a history of productive cough and documented bronchiectasis. Her temperature is 103°F, and examination reveals diffuse coarse wheezes and mild clubbing of fingers and toes. A Gram stain of expectorated sputum was performed. Into which of the following possible genera could the causative organism fit?
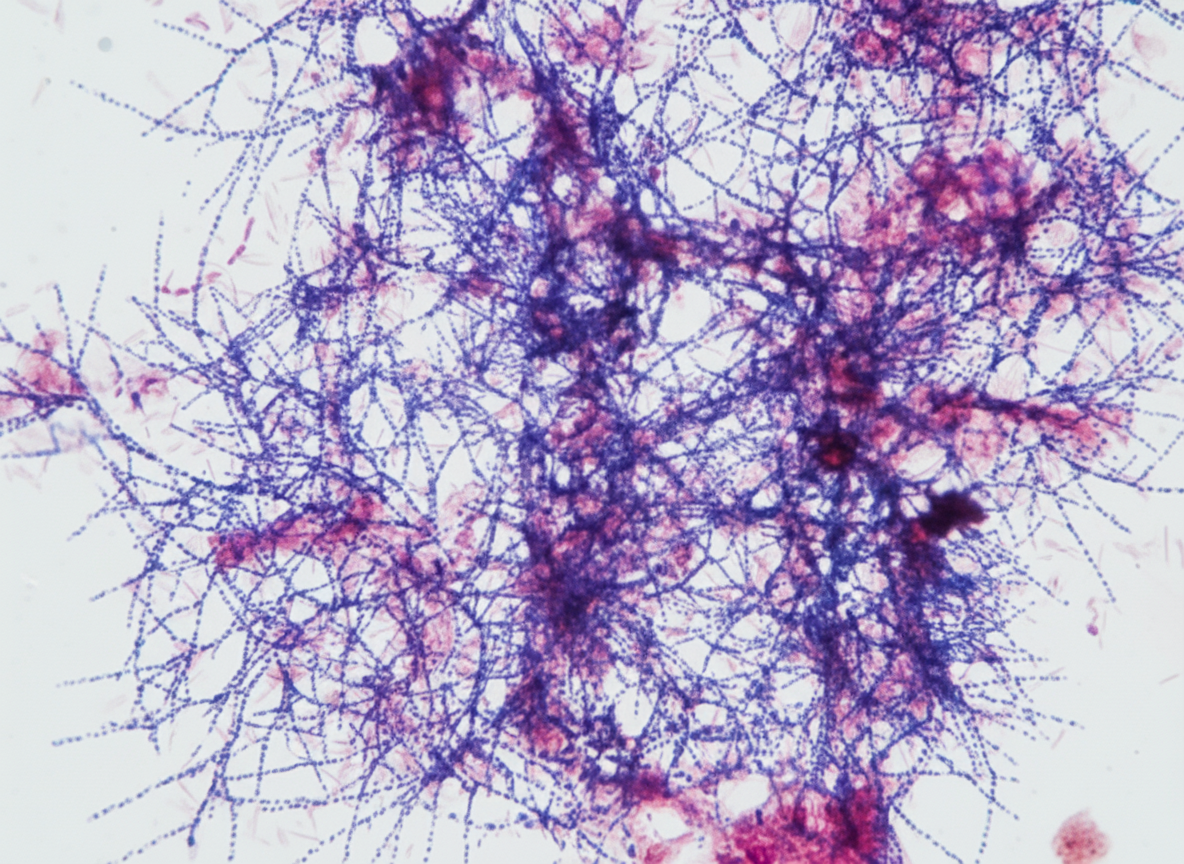
A patient presents with high fever, tachycardia, hemoptysis, and a lobar consolidation on chest X-ray. What is the most likely diagnosis?
A 40-year-old man presents with fever, weight loss, and cough. His Mantoux test result is 18 x 19 mm, and sputum cytology is negative for Acid-Fast Bacilli (AFB). What is the most likely condition?
Pulmonary hypertension may occur in all of the following conditions, EXCEPT?
All of the following conditions may predispose to pulmonary embolism except?
A middle-aged man presented with blood in the sputum. Which artery is primarily responsible for bleeding in hemoptysis?
What are the diagnostic criteria for allergic bronchopulmonary aspergillosis?
All of the following are features of Superior Vena Cava (SVC) Syndrome except?
Which of the following syndromes is associated with bronchiectasis?
Which of the following statements regarding hypersensitivity pneumonitis is FALSE?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
