Pulmonology — MCQs

On this page
Which of the following is not part of the definition of chronic bronchitis?
A 55-year-old male has a 5 cm cavitating lesion of unknown duration at the apex of the right lung. Which investigation should be carried out next?
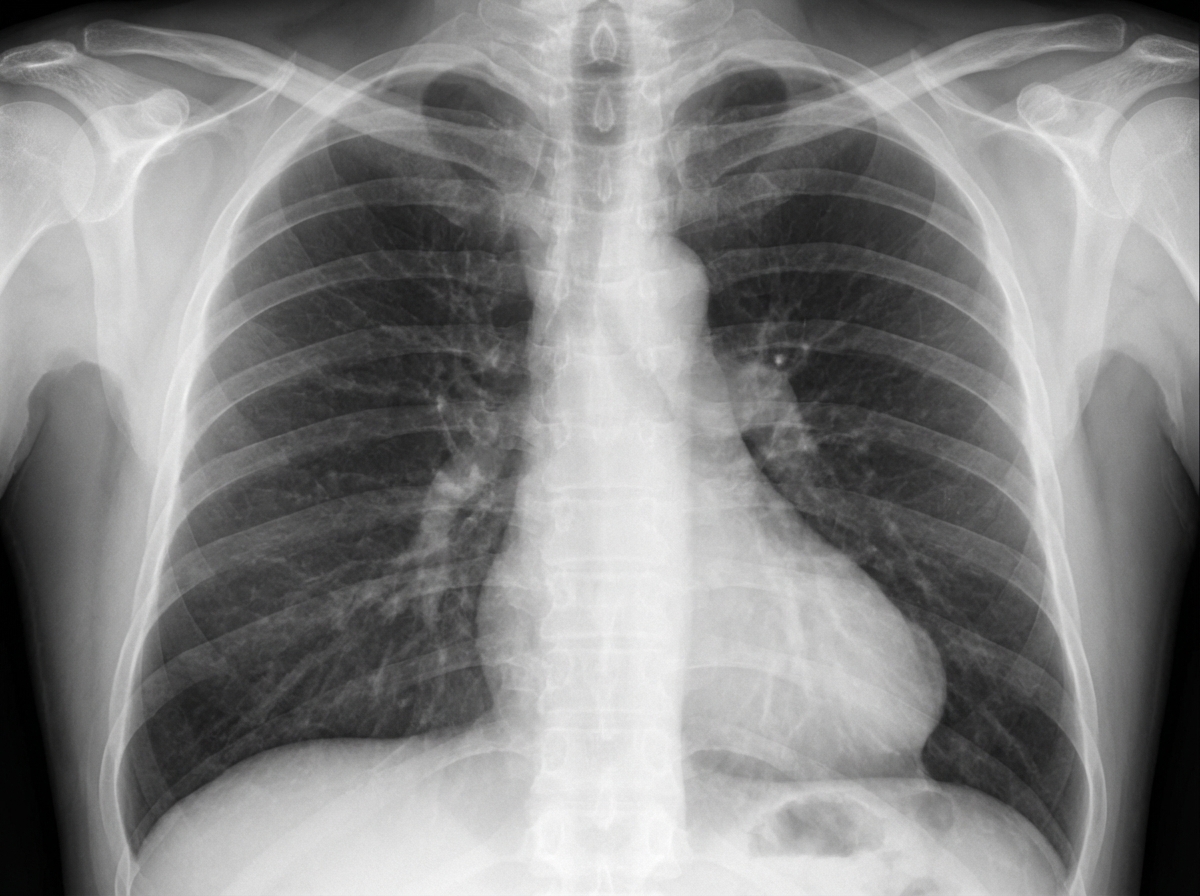
A 67-year-old male smoker presents with cough and was treated for acute bronchitis. A chest X-ray prompted a referral to the chest clinic. The patient has a past history of myocardial infarction but is currently asymptomatic. Blood pressure is 128/80, and cardiopulmonary examination is unremarkable. A purified protein derivative (PPD) test result is 7 mm. The chest X-ray is shown. What is the likely diagnosis?
The Ellis curve is characteristic of which of the following conditions?
Which of the following is not a feature of granulomatosis with polyangiitis (Wegener's syndrome)?
Which of the following is NOT a cause of decreased DLCO?
Carbon monoxide diffusion capacity decreases in all, except?
A 40-year-old man presents with recurrent hemoptysis and purulent cough. Chest X-ray was found to be normal. What is the next investigation to aid in diagnosis?
Fleeting pulmonary infiltrates on sequential chest skiagrams in an individual who suffers from asthma are characteristic of?
Which of the following is NOT true about Interstitial Fibrosis?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
