Pulmonology — MCQs

On this page
What is the characteristic symptom of asthma?
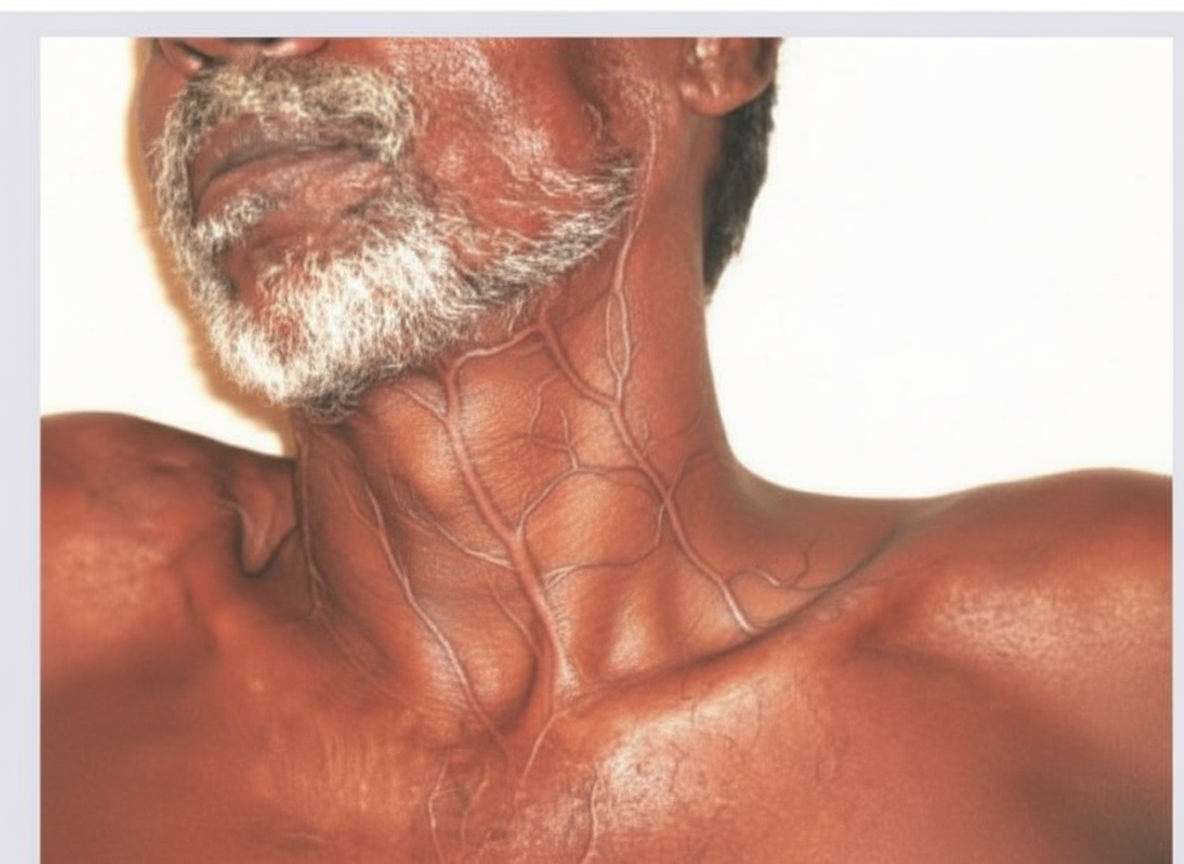
A 63-year-old man is presenting with facial swelling. What condition is the most likely cause of these findings?
Which condition is associated with bronchopulmonary aspergillosis?
Which of the following is NOT a component of Lofgren syndrome?
Acute severe lung injury is characterized by:
A truck driver presents with a one-month history of chronic cough and fever. Chest X-ray reveals bilateral reticulonodular infiltrates in the mid and lower lung zones. What is the most likely diagnosis?
Which of the following is true about obstructive lung disease?
A 50-year-old male with a known case of emphysema presents with a two-week history of shortness of breath. A chest X-ray reveals a 3 cm pneumothorax on the right side. What is the appropriate management approach for this patient?
Which artery is most frequently responsible for bleeding in massive hemoptysis?
Which of the following statements is FALSE regarding interstitial lung disease?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
