Pulmonology — MCQs

On this page
Extraparenchymal causes of respiratory failure include:
A 53-year-old man, a smoker for 35 years at a 2-pack-a-day rate, presents with a persistent cough and dyspnea. A chest X-ray reveals an increased anterior-posterior diameter, flattened diaphragms, and air trapping, ruling out malignancy. The patient is informed that his condition is irreversible and that smoking cessation is crucial to halt disease progression. At the molecular level, this disease is caused by which one of the following?
A 51-year-old male smoker presents with fever and a cough productive of greenish-yellow sputum. The patient states that he has had a morning cough with excessive mucus production for the past 5 years. Which of the following abnormalities would most likely be found in this patient?
All of the following are associated with Kartagener syndrome (immotile cilia syndrome) except?
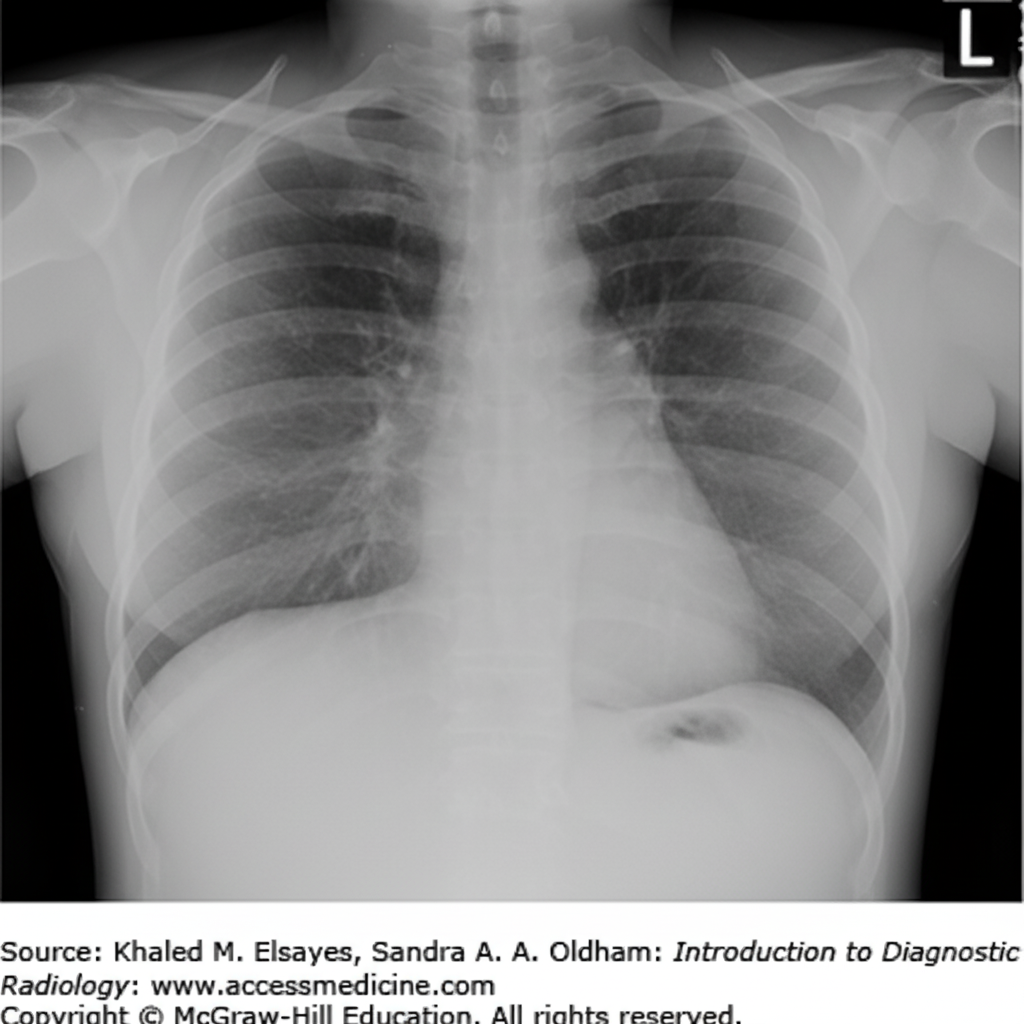
A 41-year-old man presents with severe shortness of breath. He reports a 25-lb weight loss over the last 2 months and occasional vomiting after meals. His vital signs are: pulse 110 bpm, temperature 98 F, respirations 24/min, and blood pressure 110/70 mm Hg. Physical examination reveals dullness to percussion on the left posterior chest with decreased breath sounds. Egophony is heard over the left upper lung field posteriorly. A PPD test is 15 mm. A chest X-ray is shown. What is the most likely diagnosis?
Which of the following is NOT secreted by a bronchogenic carcinoma?
What is a genetic risk factor for COPD?
A 54-year-old smoker presents with severe hemoptysis, weight loss, and oligoarthritis. Serial skiagrams show fleeting opacities. What is the diagnosis?
Bilateral pleural effusion may occur in all of the following conditions except?
Which of the following is NOT used in the management of Idiopathic Pulmonary Fibrosis (IPF)?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
