Pulmonology — MCQs

On this page
A 32-year-old female presents to the medicine outpatient department with stridor and a dry cough for the last few weeks. She complains of difficulty in breathing on exertion and in resting condition as well. On examination, she had erythema nodosum on lower limbs along with painful arthritis. Bilateral hilar lymphadenopathy was noted. Laboratory investigations showed raised levels of Angiotensin-converting enzymes (ACE). Her chest radiograph is shown below. What is the probable diagnosis in this case?
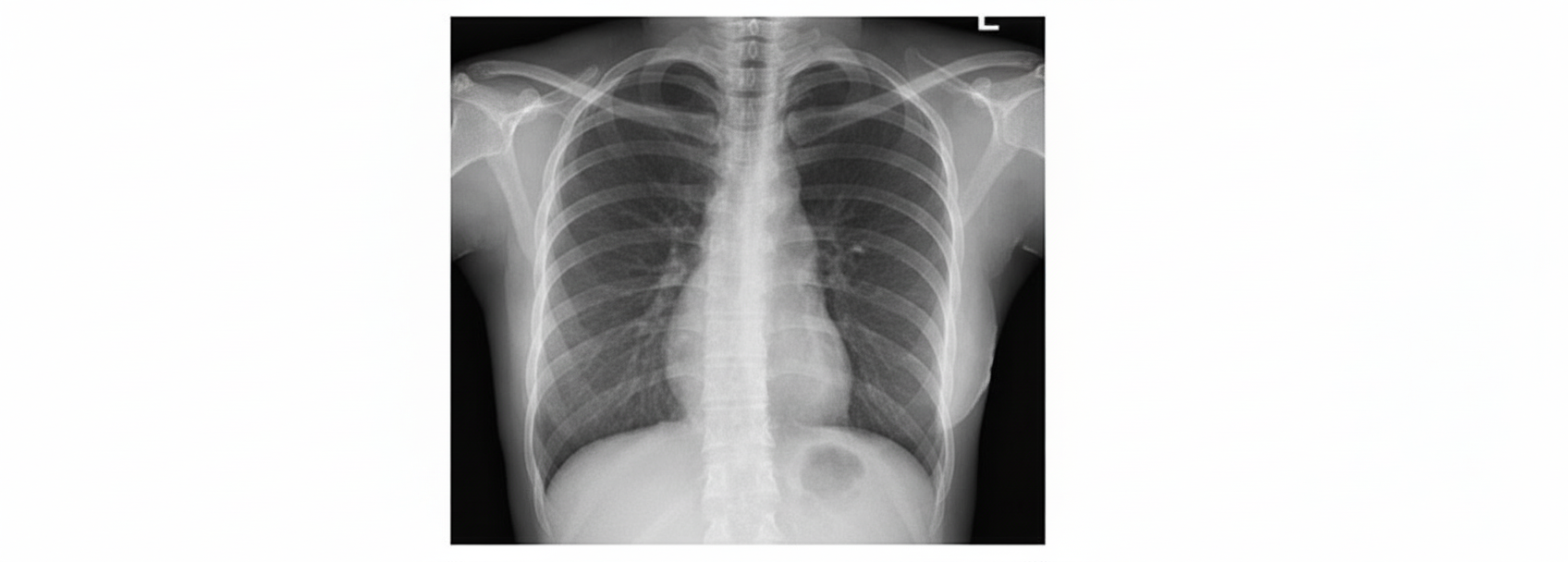
All the following statements about Emphysema are true except?
Based on the provided pulmonary function test results, what is the most likely diagnosis?
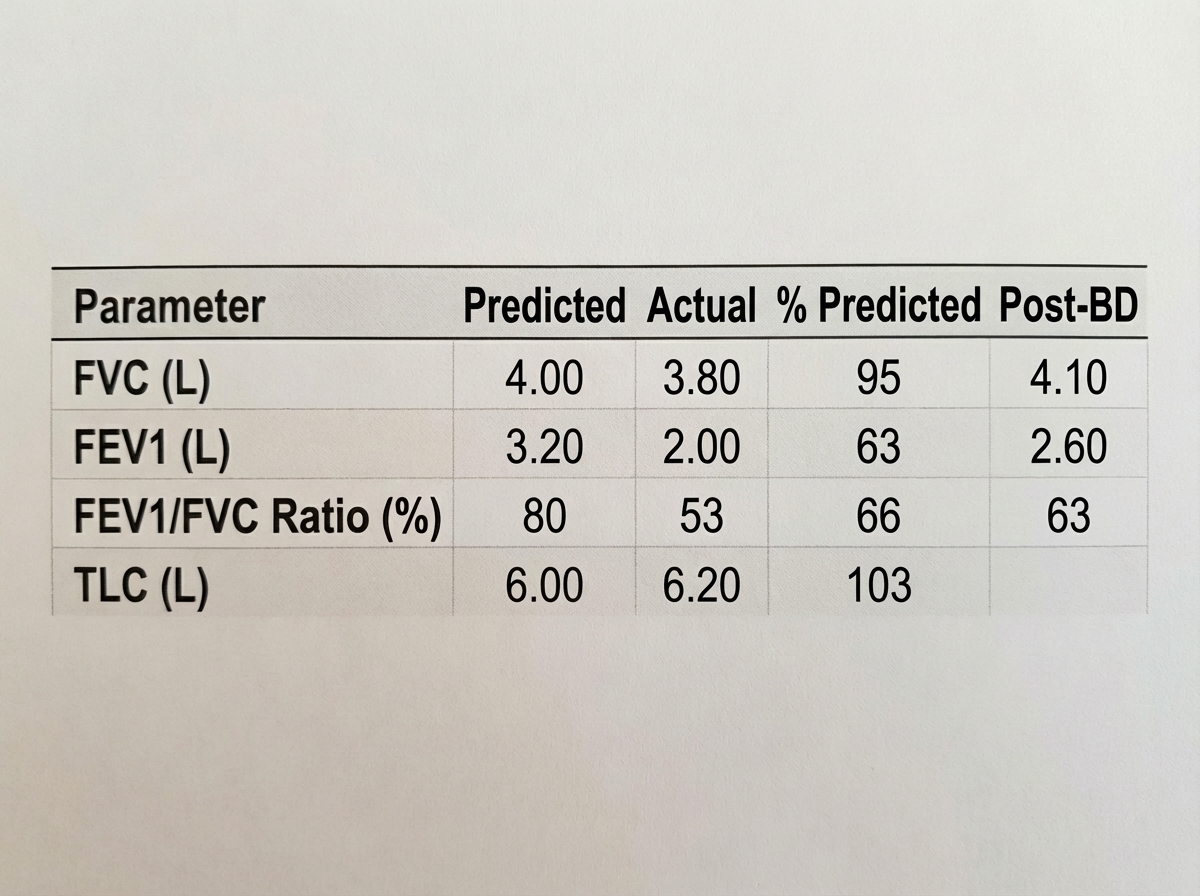
What is the most common ECG change in pulmonary embolism?
Which of the following are risk factors for pulmonary embolism?
A 23-year-old woman has had several episodes of severe wheezing over the past 3 years. She is a nonsmoker and feels well in between episodes. She has no personal or family history of atopy. The wheezing episodes are most likely to occur in spring. Which of the following is the most likely mechanism of wheezing in this woman?
Which of the following conditions is associated with pruning of pulmonary arteries?
Which of the following is an example of Type I respiratory failure?
Pulmonary edema associated with normal PCWP is observed. Which of the following is NOT a cause?
The Kveim-Siltzbach test is used in the diagnosis of which condition?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
