Oncology — MCQs

On this page
Tumor lysis syndrome is associated with all of the following laboratory features except?
In humoral hypercalcemia of malignancy, what serum calcium level indicates severe hypercalcemia, which may present with symptoms such as fatigue, mental status changes, dehydration, or nephrolithiasis?
What is the primary treatment for Superior Vena Cava (SVC) syndrome caused by Small Cell Lung Carcinoma?
What is the standard treatment regimen for metastatic testicular carcinoma?
A 74-year-old man presents with fatigue, shortness of breath on exertion, and back and rib pain worsened by movement. Investigations reveal anemia, elevated calcium, urea, and creatinine. X-rays show multiple lytic lesions in long bones and ribs, and protein electrophoresis is positive for an immunoglobulin G (IgG) paraprotein. What is the most likely mechanism for the renal injury?
A young man with leukemia is treated with methotrexate. What is the mechanism of action of this drug?
Which of the following are symptoms of carcinoid syndrome?
What is the drug of choice for chronic myeloid leukemia?
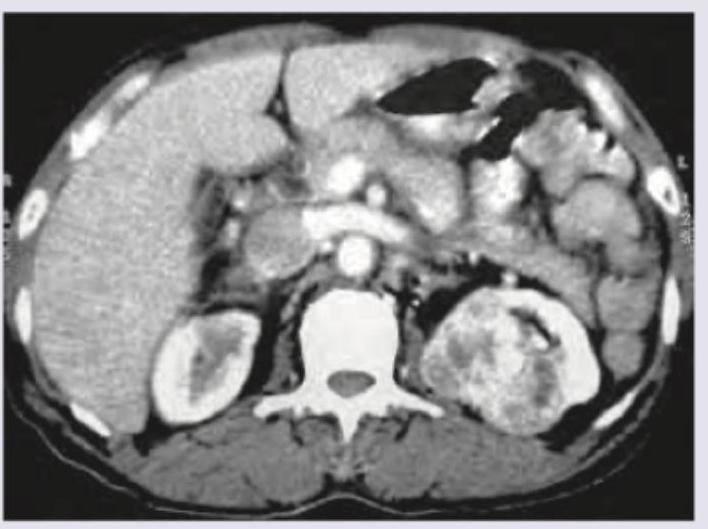
A 64-year-old man is admitted to the hospital for the assessment of hematuria after being involved in a motor vehicle accident. His physical examination is normal. A CT scan of the abdomen is shown in Figure below. Which of the following is the most likely diagnosis?
A 62-year-old woman with a family history of breast cancer (her mother died of breast cancer at age 63) is concerned about her future risk. Which of the following features is a recognized risk factor for breast cancer?
Practice by Chapter
Cancer Biology and Carcinogenesis
Practice Questions
Principles of Cancer Diagnosis and Staging
Practice Questions
Solid Tumor Management
Practice Questions
Hematological Malignancies
Practice Questions
Cancer Emergencies
Practice Questions
Principles of Chemotherapy, Immunotherapy and Targeted Therapy
Practice Questions
Radiation Oncology Basics
Practice Questions
Palliative Care in Oncology
Practice Questions
Cancer Screening and Prevention
Practice Questions
Paraneoplastic Syndromes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
